After steep positive aspects since 2020, state Medicaid businesses count on Medicaid enrollment to start to say no in FY 2023, following the expiration of the COVID-19 public well being emergency (PHE), which most states assumed would happen throughout FY 2023, in accordance with KFF’s new state Medicaid funds survey.
Projections of declining enrollment tied to the tip of the federal steady enrollment requirement are additionally anticipated to translate into slower complete Medicaid spending progress in FY 2023. On the similar time, the lack of momentary pandemic-era enhanced federal matching funding is anticipated to end in a rebalancing of the combination of federal and state spending, growing state spending although complete Medicaid spending progress is anticipated to sluggish. Medicaid officers reported that uncertainty associated to the tip of the PHE makes it troublesome for states to plan for unwinding of the PHE and to develop state budgets.
The twenty second annual survey of state Medicaid administrators finds that states count on progress in Medicaid enrollment to sluggish to eight.4 % in FY 2022 (down from 11.2 % the earlier 12 months) earlier than declining by 0.4 % in FY 2023.
Enrollment declines are more likely to speed up over time, as many states anticipated the general public well being emergency and steady protection requirement to run till the tip of this calendar 12 months, halfway via fiscal 12 months 2023 for many states. The Biden Administration just lately introduced that the PHE will go till mid-January, and has promised to provide states 60 days discover earlier than ending the emergency declaration.
The survey additionally finds that complete Medicaid spending progress – federal and state spending mixed – is anticipated to peak at 12.5 % in FY 2022, earlier than slowing to 4.2 % in FY 2023. State Medicaid officers reported that the state (nonfederal) share of Medicaid spending grew by 9.9 % in FY 2022. They projected sharper state spending progress of 16.3 % in FY 2023 with the federal authorities anticipated to finish its momentary enhanced funding.
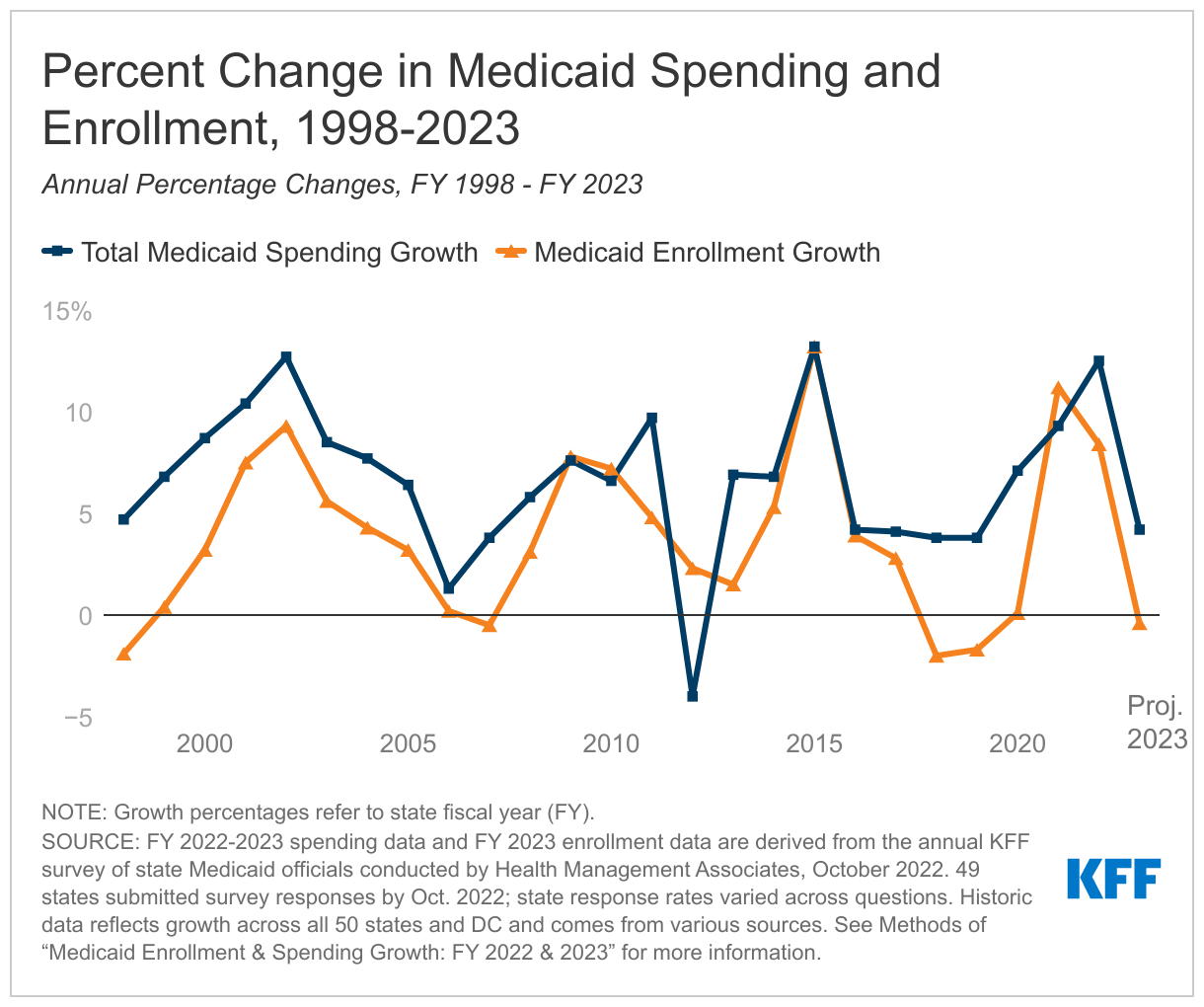
Along with enrollment progress, different drivers of elevated Medicaid spending reported by state Medicaid businesses included inflationary pressures, elevated service utilization, and elevated dwelling and community-based providers (HCBS) spending.
The survey, performed by analysts at KFF and Well being Administration Associates, offers an annual have a look at Medicaid enrollment and spending tendencies, presently for state fiscal years 2022 and 2023. Forty-nine states responded to the survey, though response charges for particular questions various. A companion survey report affords an in-depth, state-specific examination of insurance policies in place in state Medicaid packages, as effectively essential modifications and initiatives going down across the nation.
Whereas states proceed to reply to pandemic-related well being points comparable to growing vaccination and booster charges and treating long-COVID, states additionally reported actions to concentrate on longstanding points and new priorities together with bettering fairness and lowering well being disparities, sustaining entry to telehealth, bettering behavioral well being entry and helps, and addressing workforce challenges.
Some notable findings from the report embody:
- Well being Fairness. Advancing well being fairness is a vital longstanding precedence that has been elevated throughout the pandemic. Two-thirds of states reported utilizing no less than one technique to enhance race, ethnicity, and language (REL) knowledge completeness. About one quarter of states reported use of monetary incentives linked to well being fairness, principally in Medicaid managed care preparations.
- Advantages: States reported way more profit expansions than profit cuts in each FY 2022 and FY 2023. States are significantly targeted on service expansions throughout the behavioral well being care continuum in addition to expansions of being pregnant and postpartum providers. Different areas of profit growth embody preventive providers, dental providers, and providers to deal with enrollees’ social wants (comparable to meals and housing wants).
- Telehealth. States famous that expanded telehealth insurance policies elevated entry to care throughout the COVID-19 pandemic and resulted in excessive telehealth utilization throughout populations. Most states have carried out or are planning initiatives to evaluate telehealth high quality and to deal with different telehealth challenges (together with entry to expertise and broadband, program integrity, outreach and training, and fairness). Most states have or plan to undertake everlasting Medicaid telehealth coverage expansions that may stay in place even after the pandemic, although some are contemplating including limitations or guardrails.
- Managed Care. Greater than three quarters of states that contract with managed care organizations (MCOs) reported that 75 % or extra of their Medicaid beneficiaries have been enrolled in MCOs as of July 1, 2022. In FY 2022, North Carolina carried out its first MCO program. Missouri enrolled all ACA growth adults in Medicaid MCOs when it carried out the ACA Medicaid growth in October 2021.
- Supplier Charges. Supplier price will increase outnumbered price restrictions for fee-for-service in FY 2022 and FY 2023. Will increase have been extra frequent for nursing services and residential and community-based providers (HCBS) suppliers than for different supplier classes. Whereas most states depend on capitated preparations with managed care organizations to ship Medicaid providers, fee-for-service charges stay essential fee benchmarks for managed care funds. Many states famous that worsening inflation and workforce shortages driving greater labor prices have been leading to stress for price will increase. Some states famous that adopted FY 2023 budgets don’t account for present inflation ranges, although inflation stays a priority.
- Wanting Forward. States are making ready for challenges tied to the unwinding of the continual enrollment necessities and the expiration of different emergency authorities in place throughout the PHE. As well as, states have been dealing with fiscal uncertainty as a consequence of slower income progress projections, rising inflation, and workforce shortages in addition to potential shifts in political landscapes, as 36 states await the outcomes of gubernatorial elections in November 2022, with outcomes that might have implications for state Medicaid insurance policies and for Medicaid enrollees.
The survey is to be mentioned as we speak at Midday ET throughout an online briefing held by KFF with the Nationwide Affiliation of Medicaid Administrators. The 2 new studies launched as we speak upfront of the briefing are:
Medicaid Enrollment & Spending Progress: FY 2022 & 2023
How the Pandemic Continues to Form Medicaid Priorities: Outcomes from an Annual Medicaid Price range Survey for State Fiscal Years 2022 and 2023
For extra knowledge and analyses about Medicaid, go to kff.org.







