Managed care performs a serious function within the supply of well being care to Medicaid enrollees. With 69% of Medicaid beneficiaries enrolled in complete managed care plans nationally, plans have performed a key function in responding to the COVID-19 pandemic and within the fiscal implications for states. This temporary describes 10 themes associated to using complete, risk-based managed care within the Medicaid program and highlights important knowledge and developments. Understanding these developments supplies necessary context for the function managed care organizations (MCOs) play within the Medicaid program general in addition to in the course of the ongoing COVID-19 public well being emergency (PHE) and in its anticipated unwinding. CMS launched steerage for state Medicaid businesses outlining how managed care plans can promote continuity of protection for people as states resume regular operations when the continual protection requirement in the course of the public well being emergency ends. Whereas we will observe state necessities for Medicaid managed care plans, plans have flexibility in sure areas together with in setting supplier fee charges and plans may select to supply providers past these required within the Medicaid state plan or waivers. States additionally make choices about which populations and providers to incorporate in managed care preparations resulting in appreciable variation throughout states.
1. At this time, capitated managed care is the dominant approach through which states ship providers to Medicaid enrollees.
States design and administer their very own Medicaid applications inside federal guidelines. States decide how they may ship and pay for look after Medicaid beneficiaries. Practically all states have some type of managed care in place – complete risk-based managed care and/or main care case administration (PCCM) applications., As of July 2021, 41 states (together with DC) contract with complete, risk-based managed care plans to supply care to at the very least a few of their Medicaid beneficiaries (Determine 1). North Carolina is the newest state to be included on this rely, having launched complete risk-based Medicaid managed care statewide on July 1, 2021. Medicaid MCOs (additionally known as “managed care plans”) present complete acute care and in some circumstances long-term providers and helps to Medicaid beneficiaries. MCOs settle for a set per member per 30 days fee for these providers and are at monetary danger for the Medicaid providers specified of their contracts. States have pursued risk-based contracting with managed care plans for various functions, searching for to extend funds predictability, constrain Medicaid spending, enhance entry to care and worth, and meet different goals. Whereas the shift to MCOs has elevated funds predictability for states, the proof in regards to the affect of managed care on entry to care and prices is each restricted and blended.,
2. Every year, states develop MCO capitation charges that have to be actuarially sound and should embrace danger mitigation methods.
States pay Medicaid managed care organizations a set per member per 30 days fee for the Medicaid providers specified of their contracts. Underneath federal legislation, funds to Medicaid MCOs have to be actuarially sound. Actuarial soundness implies that “the capitation charges are projected to supply for all cheap, acceptable, and attainable prices which are required underneath the phrases of the contract and for the operation of the managed care plan for the time interval and the inhabitants lined underneath the phrases of the contract.” Not like fee-for-service (FFS), capitation supplies upfront fastened funds to plans for anticipated utilization of lined providers, administrative prices, and revenue. Plan charges are normally set for a 12-month ranking interval (which generally run on a calendar 12 months or state fiscal 12 months foundation) and have to be reviewed and accepted by CMS every year. States could use a wide range of mechanisms to regulate plan danger, incentivize plan efficiency, and guarantee funds aren’t too excessive or too low, together with danger sharing preparations, danger and acuity changes, medical loss ratios (MLRs, which mirror the proportion of whole capitation funds obtained by an MCO spent on medical providers and high quality enchancment), or incentive and withhold preparations.
CMS allowed states to change managed care contracts in response to unanticipated COVID-19 prices and circumstances that led to decreased utilization. States have a number of choices to deal with these fee points together with danger mitigation methods, adjusting capitation charges, masking COVID-19 prices on a non-risk foundation, and carving out prices associated to COVID-19 from MCO contracts (Determine 2). These choices differ broadly by way of implementation/operational complexity, and all choices require CMS approval. Greater than half of MCO states reported implementing COVID-19-related danger corridors of their 2020 or 2021 contracts. Of those states, about half reported that they’ve or will recoup funds, whereas recoupment for the remaining states was undetermined on the time of KFF’s annual 50-state Medicaid funds survey. Evaluation of Nationwide Affiliation of Insurance coverage Commissioners (NAIC) knowledge for the Medicaid managed care market present that annual loss ratios in 2020 (in combination throughout plans) decreased by 4 proportion factors from 2019 (and three proportion factors from 2018), however nonetheless met the 85% minimal even with out accounting for potential changes. As 2022 begins, states and plans face continued uncertainty associated to the pandemic’s trajectory which can proceed to affect utilization patterns and lead to price setting challenges for states.

Determine 2: CMS Has Supplied Steerage to States to Tackle MCO Fee Points in Response to the COVID-19 Pandemic.
3. As of July 2019, greater than two-thirds (69%) of all Medicaid beneficiaries obtained their care by complete risk-based MCOs.
As of July 2019, 53.7 million Medicaid enrollees obtained their care by risk-based MCOs. Twenty-five MCO states lined greater than 75% of Medicaid beneficiaries in MCOs (Determine 3).
Though 2019 knowledge (displayed above) are essentially the most present nationwide knowledge obtainable on Medicaid MCO enrollment, enrollment in Medicaid general has grown considerably for the reason that begin of the coronavirus pandemic in February 2020. This enrollment progress displays each modifications within the economic system in addition to provisions within the Households First Coronavirus Response Act (FFCRA) that require states to make sure steady protection for present Medicaid enrollees to entry a short lived improve within the Medicaid match price in the course of the PHE interval. KFF evaluation of newer MCO enrollment knowledge, from the subset of states that make these knowledge obtainable, exhibits progress in Medicaid MCO enrollment in the course of the pandemic tracks general Medicaid enrollment developments. When the continual protection necessities finish, states will start processing redeterminations and renewals and thousands and thousands of individuals may lose Medicaid protection if they’re not eligible or face administrative obstacles in the course of the course of regardless of remaining eligible. CMS has launched steerage and methods for states to assist preserve protection of eligible people after the top of steady enrollment necessities, together with steerage outlining how managed care plans can help states in selling continuity of protection.
4. Kids and adults usually tend to be enrolled in MCOs than seniors or individuals with disabilities; nonetheless, states are more and more together with beneficiaries with complicated wants in MCOs.
As of July 2021, 37 MCO states reported masking 75% or extra of all youngsters by MCOs (Determine 4). Of the 38 states that had applied the ACA Medicaid growth as of July 2021, 31 states have been utilizing MCOs to cowl newly eligible adults and the massive majority of those states lined greater than 75% of beneficiaries on this group by MCOs. Thirty-four MCO states reported masking 75% or extra of low-income adults in pre-ACA growth teams (e.g., mother and father, pregnant ladies) by MCOs. In distinction, solely 19 MCO states reported protection of 75% or extra of seniors and folks with disabilities. Though this group remains to be much less prone to be enrolled in MCOs than youngsters and adults, over time, states have been transferring to incorporate seniors and folks with disabilities in MCOs.
5. Lately, many states have moved to carve in behavioral well being providers, pharmacy advantages, and long-term providers and helps to MCO contracts.
Though MCOs present complete providers to beneficiaries, states could carve particular providers out of MCO contracts to fee-for-service (FFS) programs or restricted profit plans. Companies ceaselessly carved out embrace behavioral well being, pharmacy, dental, and long-term providers and helps (LTSS). Nonetheless, there was important motion throughout states to carve these providers in to MCO contracts. Whereas the overwhelming majority of states that contract with MCOs report that the pharmacy profit is carved in to managed care (35 of 41), 5 states report that pharmacy advantages are carved out of MCO contracts as of July 2021 (Determine 5). Three states report plans to carve out pharmacy from MCO contracts in FY 2022 or later (California, New York, and Ohio).
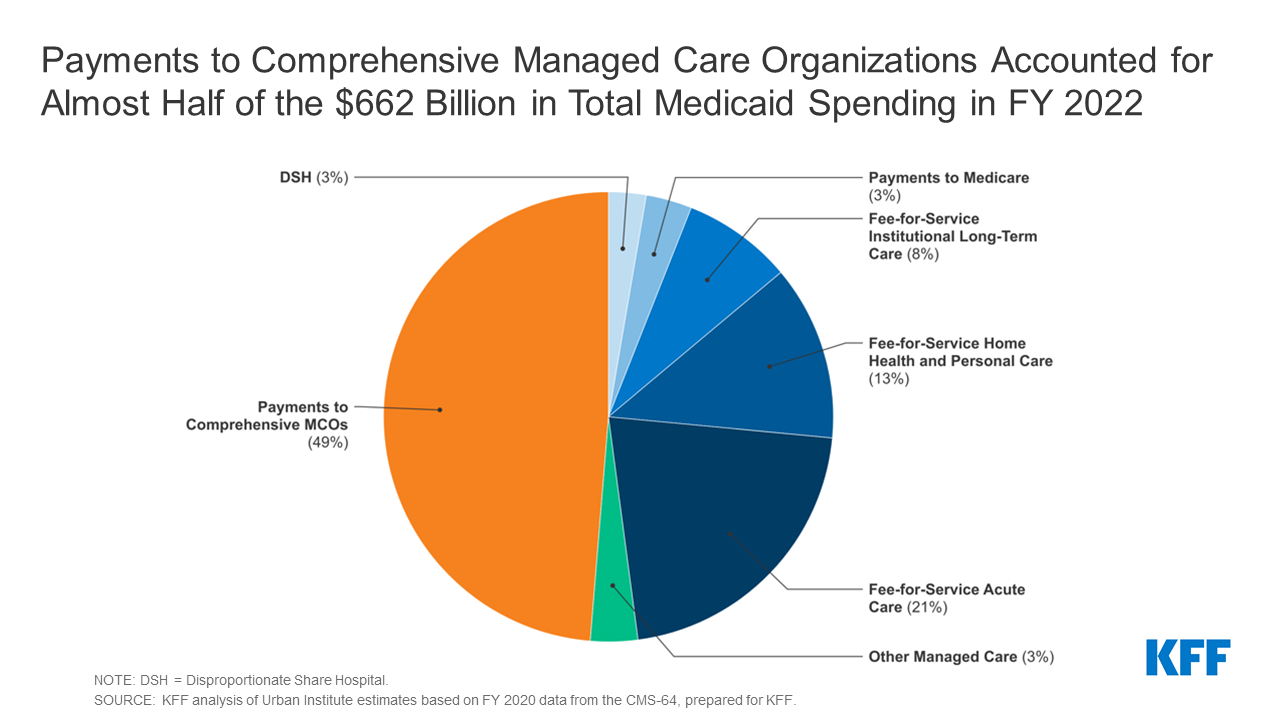
6. In FY 2020, funds to complete risk-based MCOs accounted for the biggest share of Medicaid spending.
In FY 2020, state and federal spending on Medicaid providers totaled over $662 billion. Funds made to MCOs accounted for about 49% of whole Medicaid spending (Determine 6), a rise of just about three proportion factors from the earlier fiscal 12 months. The share of Medicaid spending on MCOs varies by state, however over three-quarters of MCO states directed at the very least 40% of whole Medicaid {dollars} to funds to MCOs (Determine 7). The MCO share of spending ranged from a low of about 2% in Colorado to 88% in Kansas. State-to-state variation displays many components, together with the proportion of the state Medicaid inhabitants enrolled in MCOs, the well being profile of the Medicaid inhabitants, whether or not high-risk/high-cost beneficiaries (e.g., individuals with disabilities, twin eligible beneficiaries) are included in or excluded from MCO enrollment, and whether or not or not long-term providers and helps are included in MCO contracts. As states broaden Medicaid managed care to incorporate higher-need, higher-cost beneficiaries, costly long-term providers and helps, and adults newly eligible for Medicaid underneath the ACA, the share of Medicaid {dollars} going to MCOs will proceed to extend.
7. Various massive medical health insurance firms have a big stake within the Medicaid managed care market.
States contracted with a complete of 282 Medicaid MCOs as of July 2019. MCOs characterize a mixture of personal for-profit, personal non-profit, and authorities plans. As of July 2019, a complete of 16 companies operated Medicaid MCOs in two or extra states (referred to as “father or mother” companies), and these companies accounted for 63% of enrollment in 2019 (Determine 9). Of the 16 father or mother companies, seven are publicly traded, for-profit companies whereas the remaining 9 are non-profit firms. Six companies – UnitedHealth Group, Centene, Anthem, Molina, Aetna/CVS, and WellCare – every have MCOs in 12 or extra states (Determine 8) and accounted for 51% of all Medicaid MCO enrollment (Determine 9). All six are publicly traded firms ranked within the Fortune 500. KFF evaluation of newer MCO enrollment knowledge, from the subset of states that make these knowledge obtainable, confirmed that 5 for-profit father or mother companies (Centene, Molina, Anthem, UnitedHealth Group, and Aetna/CVS) accounted for nearly 60% of the pandemic-related improve in MCO enrollment from March 2020 to March 2021 in these states. Earnings stories from This fall 2021 for these 5 for-profit father or mother companies (Centene, Molina, Anthem, UnitedHealth Group, and Aetna/CVS) confirmed year-over-year progress in Medicaid membership (2021 over 2020) starting from 10 to twenty% and for the three companies that offered Medicaid-specific income data (Centene, Molina, and UnitedHealth Group) progress in Medicaid revenues starting from 13 to 43%.
8. Inside broad federal and state guidelines, plans usually have discretion in how to make sure entry to look after enrollees and how one can pay suppliers.
Plan efforts to recruit and preserve their supplier networks can play a vital function in figuring out enrollees’ entry to care by components akin to journey occasions, wait occasions, or selection of supplier. Federal guidelines require that states set up community adequacy requirements. States have an excessive amount of flexibility to outline these requirements. The 2020 CMS Medicaid managed care last rule eliminated the requirement that states use time and distance requirements to make sure supplier community adequacy and as an alternative lets states select any quantitative customary. KFF carried out a survey of Medicaid managed care plans in 2017 and located that responding plans reported a wide range of methods to deal with supplier community points, together with direct outreach to suppliers, monetary incentives, automated project of members to PCPs, and immediate fee insurance policies. Nonetheless, regardless of using varied methods, plans reported extra challenges in recruiting specialty suppliers than in recruiting main care suppliers to their networks. Plans reported that these challenges have been extra seemingly resulting from supplier provide shortages than resulting from low supplier participation in Medicaid. In June 2021, CMS introduced plans to introduce a collection of instruments to enhance the monitoring and oversight of managed care in Medicaid and CHIP. CMS plans to launch reporting templates for required managed care stories (Annual Program Oversight Report, MLR Abstract Report, Entry Requirements Report) in addition to technical help toolkits (e.g., behavioral well being entry, methods for guaranteeing supplier community adequacy) to help states in complying with varied managed care requirements and laws.
To assist guarantee participation, many states require minimal supplier charges of their contracts with MCOs which may be tied to fee-for-service charges. In a 2021 KFF annual survey of Medicaid administrators, about two-thirds of responding states with MCO and/or restricted profit contracts (pre-paid well being plans, or “PHPs”) reported a minimal payment schedule that units a reimbursement ground for a number of specified supplier sorts (Determine 10). Moreover, over half of responding states that contract with managed care plans reported a uniform greenback or proportion improve fee requirement in place as of July 2021, mostly for hospitals. In response to the COVID-19 pandemic, states have choices and flexibilities underneath current managed care guidelines to direct/bolster funds to Medicaid suppliers and to protect entry to look after enrollees. A couple of-third of responding MCO states applied new supplier fee and/or pass-through necessities on MCOs in response to the COVID-19 emergency in FY 2021.
9. Over time, the growth of risk-based managed care in Medicaid has been accompanied by larger consideration to measuring high quality and outcomes.
States incorporate high quality metrics into the continued monitoring of their applications, together with linking monetary incentives like efficiency bonuses or penalties, capitation withholds, or value-based state-directed funds to high quality measures. In a 2021 KFF annual survey of Medicaid administrators, over three-quarters of responding MCO states reported utilizing at the very least one monetary incentive to advertise high quality of care (in a specified efficiency space) as of July 2021 (Determine 11). Monetary incentive efficiency areas most ceaselessly focused by MCO states embrace behavioral well being, continual illness administration, and perinatal/beginning outcomes. These focus areas aren’t stunning given the continual bodily well being and behavioral well being wants of the Medicaid inhabitants, in addition to the numerous share of the nation’s births funded by Medicaid. Various states reported making modifications to their high quality incentive applications because of the COVID-19 pandemic, because the pandemic has seemingly affected medical practices and well timed reporting of high quality knowledge. Regardless of exercise on this space, detailed efficiency data on the plan-level shouldn’t be ceaselessly made publicly obtainable by state Medicaid businesses, limiting transparency and the power of Medicaid beneficiaries (and different stakeholders) to evaluate how plans are acting on key indicators associated to entry, high quality, and many others.
As a part of managed care plan contract necessities, state Medicaid applications have additionally been centered on using various fee fashions (APMs) to reimburse suppliers and incentivize high quality. Different fee fashions (APMs) exchange FFS/volume-driven supplier funds and lie alongside a continuum, starting from preparations that contain restricted or no supplier monetary danger (e.g., pay-for-performance (P4P) fashions) to preparations that place suppliers at extra monetary danger (e.g., shared financial savings/danger preparations or world capitation funds). As of July 2021, greater than half of responding MCO states recognized a selected goal of their MCO contracts for the proportion of supplier funds or plan members that MCOs should cowl through APMs. Of those states, about half reported that their MCO contracts included incentives or penalties for assembly or failing to fulfill APM targets. For many states, the necessities for APMs have been within the 25 – 50% vary. States reported setting completely different proportion necessities relying on the providers and inhabitants served underneath the managed care contract. 13 states reported that their APM targets have been linked to the Well being Care Fee Studying & Motion Community’s (LAN’s) APM Framework that categorizes APMs in tiers.
Whereas there’s some proof of constructive impacts from state use of economic incentives to have interaction managed care plans round high quality and outcomes, the outcomes are extra blended and restricted on the supplier degree. ,,
10. States need to Medicaid MCOs to develop methods to establish and deal with social determinants of well being and to cut back well being disparities.
Many states are leveraging MCO contracts to advertise methods to deal with social determinants of well being (SDOH), although how far these efforts will go or how efficient they are going to be stays to be seen. Social determinants of well being (SDOH) are the circumstances through which persons are born, grown, reside, work, and age that form well being. In a 2021 KFF survey of Medicaid administrators, the overwhelming majority of responding MCO states reported leveraging Medicaid MCO contracts to advertise at the very least one technique to deal with social determinants of well being in FY 2021 (Determine 12). Greater than half of responding MCO states reported requiring MCOs to display enrollees for behavioral well being wants, present referrals to social providers, companion with community-based organizations (CBOs), and display enrollees for social wants. About half of responding MCO states reported requiring or planning to require uniform SDOH questions inside MCO screening instruments. Fewer states reported requiring MCOs to trace the outcomes of referrals to social providers or requiring MCO neighborhood reinvestment (e.g. tied to plan revenue or MLR) in comparison with different methods; nonetheless, quite a lot of states indicated plans to require these actions in FY 2022.
Communities of coloration have greater charges of underlying well being circumstances in comparison with White individuals and usually tend to be uninsured or report different well being care entry barrier. The COVID-19 pandemic exacerbated already current well being disparities for a broad vary of populations, however particularly for individuals of coloration. We requested states to establish progressive or notable initiatives on this space in our 2021 KFF survey of Medicaid administrators. About half of responding states reported managed care necessities and/or initiatives to deal with well being disparities, together with Efficiency Enchancment Initiatives (PIPs), necessities that MCOs obtain the NCQA Distinction in Multicultural Well being Care, and pay-for-performance (P4P) initiatives. Lastly, given the massive variety of individuals lined by Medicaid, together with teams disproportionately prone to contracting COVID-19 in addition to many people going through entry challenges, state Medicaid applications and Medicaid MCOs (which enroll over two-thirds of all Medicaid beneficiaries) may also help in COVID-19 vaccination efforts. In response to KFF’s 2021 50-state Medicaid funds survey, states reported a wide range of MCO actions aimed toward selling the take-up of COVID-19 vaccinations. States reported MCOs are utilizing member and supplier incentives, member outreach and training, supplier engagement, help with vaccination scheduling and transportation coordination, and partnerships with state and native organizations.