Key Takeaways
The COVID-19 pandemic has had a disproportionate impression on individuals with disabilities, together with kids with particular well being care wants, highlighting the significance of medical insurance protection, affordability, and profit package deal contents, like house and community-based providers (HCBS). This subject transient describes key traits of kids with particular well being care wants and explores insurance coverage affordability and advantages for youngsters coated by Medicaid/CHIP in comparison with these with non-public insurance coverage solely. This transient supplies context for ongoing coverage discussions round extra investments in Medicaid HCBS for youngsters with particular well being care wants. Key findings embrace the next:
- Medicaid/CHIP covers nearly half of all U.S. kids with particular well being care wants, although the share varies by state. These kids usually tend to be low-income, a member of a racial or ethnic minority group, and youthful than these kids coated by non-public insurance coverage alone.
- Youngsters with particular well being care wants coated by each Medicaid/CHIP and personal insurance coverage have the best well being care wants, and kids with Medicaid/CHIP solely usually tend to have better well being wants in comparison with these with non-public insurance coverage solely.
- Whereas households of Medicaid/CHIP-only kids with particular well being care wants usually tend to face monetary problem, they discover their well being care extra reasonably priced than these with non-public insurance coverage solely on account of Medicaid’s cost-sharing protections.
- Despite the fact that kids with particular well being care wants coated by Medicaid/CHIP-only have better well being care wants, they’re extra possible than these with non-public insurance coverage alone to report that their advantages are at all times ample to satisfy their wants, permit them to see wanted suppliers, and meet their behavioral well being wants, reflecting Medicaid’s sturdy profit package deal.
Medicaid is the first payer for HCBS and performs a big position in offering kids with particular well being care wants the long-term providers and helps (LTSS) they should stay at house with their households. Whereas unmet want for HCBS for individuals with disabilities pre-dates the COVID-19 pandemic, the pandemic has introduced a heightened concentrate on the necessity for added HCBS. The American Rescue Plan Act supplies a brief improve in federal Medicaid matching funds for state spending on HCBS, and Congress presently is contemplating extra Medicaid HCBS funding as a part of price range reconciliation, which states may use to assist the HCBS supplier workforce, supply new or expanded HCBS advantages, and/or serve extra HCBS enrollees, although the ultimate funding quantity has not but been set.
Introduction
The COVID-19 pandemic has had a disproportionate impression on individuals with disabilities, together with kids, whose well being and repair wants might place them at elevated threat of contracting COVID-19 and changing into severely in poor health. Youngsters on the whole even have skilled well being care disruptions, psychological well being challenges, and financial hardships, because the pandemic has coincided with vital intervals of their bodily, social, and emotional growth. All of those results could also be intensified for the estimated 13.9 million kids, or 19% of all kids within the U.S., who’ve particular well being care wants. As outlined by the U.S. Division of Well being and Social Providers, these kids “have or are at elevated threat for persistent bodily, developmental, behavioral or emotional situations and likewise require well being and associated providers of a kind or quantity past that required by kids usually.” Whereas these information are from 2019 (see Strategies field beneath for particulars), points akin to unmet want for house and community-based providers (HCBS) and well being disparities for low-income kids and kids of coloration usually pre-dated and have been exacerbated by the pandemic. Consequently, medical insurance protection, affordability, and profit package deal contents are particularly vital for youngsters with particular well being care wants.
Attributable to their persistent well being situations, kids with particular well being care wants might depend on long-term providers and helps (LTSS), together with HCBS. Medicaid is the first payer for LTSS and supplies HCBS akin to non-public obligation nursing, attendant care, assistive expertise, non-medical transportation to advertise group integration, and case administration providers that assist kids with particular well being care wants stay at house with their households. These providers might not be coated in any respect, or might not be coated adequately or affordably, by non-public insurance coverage. On the identical time, state Medicaid HCBS applications and suppliers have been challenged by the pandemic and accompanying financial downturn. A current KFF survey discovered that the Medicaid HCBS supplier infrastructure declined in the course of the pandemic, with two-thirds of responding states reporting a everlasting closure of no less than one supplier.
The American Rescue Plan Act (ARPA) supplies a brief improve within the federal matching charge (FMAP) for state spending on Medicaid HCBS to fund actions that increase or strengthen HCBS. Whereas the ARPA enhanced funds can be found just for one yr, extra federal funding for HCBS is a part of the price range reconciliation package deal proposed by Democratic leaders, although the small print proceed to be labored out. President Biden earlier this yr proposed a $400 billion federal funding in Medicaid HCBS, although it’s unclear how a lot of that funding improve can be accredited by Congress because it considers competing priorities within the price range package deal. The Home Vitality and Commerce Committee just lately launched their suggestions for the price range package deal that features $190 billion for Medicaid HCBS. This subject transient supplies context for ongoing coverage discussions by describing key traits of kids with particular well being care wants, evaluating insurance coverage affordability and entry to key advantages amongst these coated by Medicaid/CHIP and people with non-public insurance coverage, and contemplating the implications of extra Medicaid HCBS funding for youngsters with particular well being care wants.
How are kids with particular well being care wants coated?
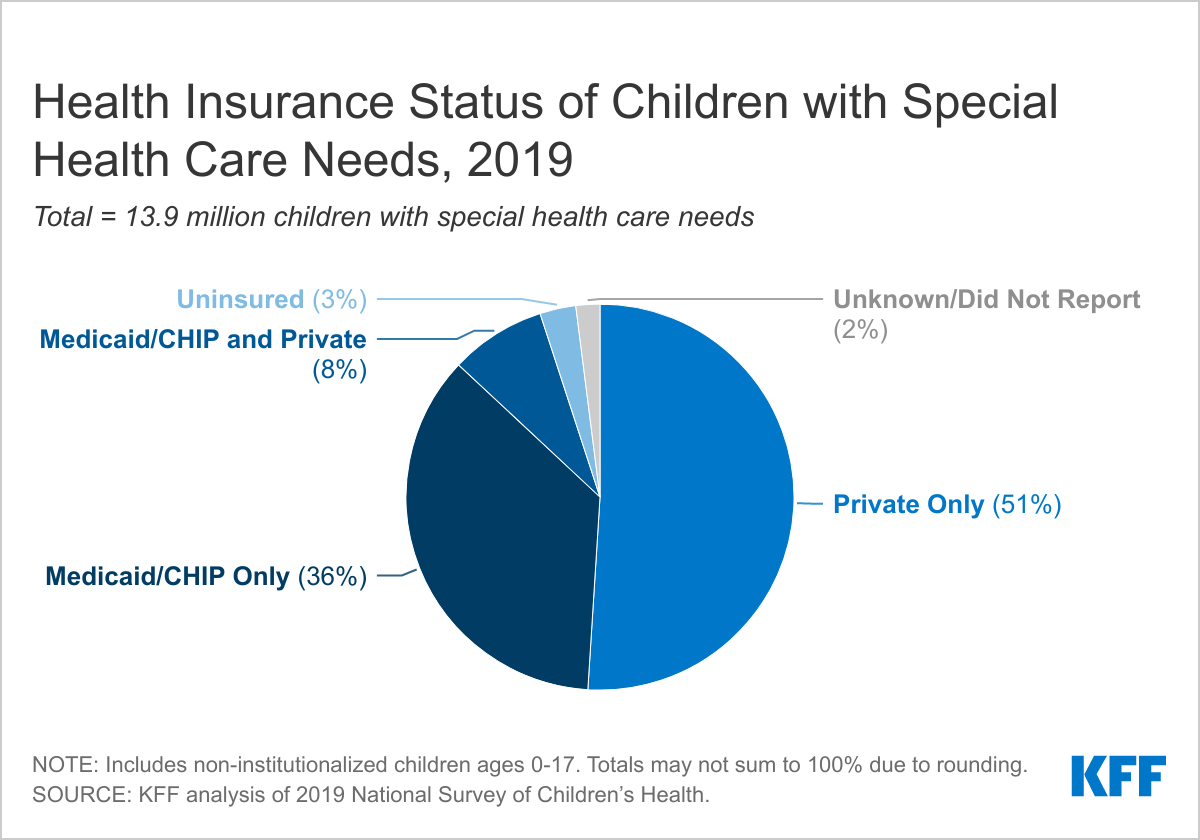
Along with the Youngsters’s Well being Insurance coverage Program (CHIP), Medicaid covers nearly half of all kids with particular well being care wants (Determine 1). Medicaid/CHIP is the one supply of protection for almost 4 in 10 kids with particular well being care wants, whereas one other 8% have Medicaid/CHIP to complement non-public insurance coverage. Simply over half of kids with particular well being care wants have non-public insurance coverage as their sole supply of protection.
Who Are Youngsters with Particular Well being Care Wants?
Youngsters with particular well being care wants with Medicaid/CHIP as their sole supply of protection usually tend to stay in a low-income family, in comparison with these with non-public insurance coverage solely. Practically two-thirds of Medicaid/CHIP-only kids with particular well being care wants stay in a family with earnings at or beneath 138% of the federal poverty stage (FPL, lower than $30,305/yr for a household of three in 2021) in comparison with 7% of kids with non-public protection solely (Determine 2). Federal Medicaid program guidelines cowl kids with family incomes as much as 138% FPL, however all states choose to increase monetary eligibility to increased earnings ranges: as of January 2021, the median monetary eligibility stage for Medicaid/CHIP kids nationally is 255% FPL ($55,998/yr for a household of three). Some kids with particular well being care wants qualify for Medicaid based mostly solely on their household’s low earnings. Different kids with particular well being care wants might qualify for Medicaid via numerous disability-related pathways, which can increase earnings limits to 300% SSI ($28,584/yr for a person, equal to about 222% FPL) or solely take into account the kid’s personal, and never their mother and father’, earnings.
The share of kids with particular well being care wants coated by Medicaid/CHIP varies by state. State eligibility limits in pathways for youngsters who qualify for Medicaid/CHIP based mostly solely on their low earnings vary from 175% FPL to 405% FPL. Moreover, most disability-related Medicaid eligibility pathways are elective and fluctuate throughout states. States should present Medicaid to kids who obtain federal Supplemental Safety Revenue (SSI) advantages, however solely an estimated 21% of kids with disabilities coated by Medicaid/CHIP obtain SSI. Which means that the overwhelming majority of Medicaid kids with particular well being care wants are eligible both based mostly on their household’s low earnings or via an elective disability-related pathway. Thirty-two states present Medicaid/CHIP to below half of kids with particular well being care wants residing of their state, and 19 states, together with DC, present Medicaid/CHIP to over half of kids with particular well being care wants residing of their state (Determine 3 and Appendix Desk 1). Components that possible contribute states protecting extra kids with particular well being care wants are the state’s earnings eligibility limits, the share of kids with particular well being care wants residing in low-income households within the state, and the state’s disability-related eligibility pathway choices.
Medicaid/CHIP-only kids with particular well being care wants usually tend to be a member of a racial or ethnic minority group in comparison with these with non-public insurance coverage solely. Medicaid/CHIP-only kids with particular well being care wants are nearly 3 times as prone to be non-Hispanic Black and 1.5 occasions as prone to be Hispanic than kids with non-public protection solely (Determine 2). The vast majority of kids with particular well being care wants with non-public insurance coverage solely are non-Hispanic white, whereas a majority of these with Medicaid/CHIP are individuals of coloration.
Medicaid/CHIP-only kids with particular well being care wants usually tend to be youthful in comparison with these with non-public insurance coverage solely. One in 5 (20%) Medicaid/CHIP-only kids with particular well being care wants are age 5 or youthful, with the rest nearly evenly cut up between the 6 to 11 (40%) and 12 to 17 (40%) age teams (Determine 2). These with non-public insurance coverage solely usually tend to be older, with nearly half (49%) between the ages of 12 and 17. The truth that extra Medicaid/CHIP-only kids with particular well being care wants are below 12, in comparison with these with non-public insurance coverage solely, implies that they are going to have an extended wait till a COVID-19 vaccine is out there. A vaccine is presently accredited for ages 12 and older, and medical trials are underway for youthful age teams.
What Well being Situations and Wants do Youngsters with Particular Well being Care Wants Have?
Medicaid/CHIP-only kids with particular well being care wants usually tend to have better well being wants in comparison with these with non-public insurance coverage solely. Medicaid/CHIP-only kids with particular well being care wants are 3 times as prone to expertise truthful or poor well being and 1.5 occasions as prone to report their well being normally or at all times impacts their every day actions considerably or an ideal deal well being in comparison with kids with non-public insurance coverage solely (Determine 4). Medicaid/CHIP-only kids with particular well being care wants usually tend to have a number of purposeful difficulties than these with non-public insurance coverage solely, with just below half of the Medicaid/CHIP-only group reporting 4 or extra purposeful difficulties, in comparison with lower than one-third with non-public insurance coverage solely (Determine 4). Medicaid/CHIP-only kids with particular well being care wants additionally usually tend to report severe problem in every of the six purposeful areas in contrast these with non-public insurance coverage solely (Determine 4). For instance, Medicaid/CHIP-only kids with particular well being care wants are nearly 3 times extra prone to have severe problem dressing/bathing and two occasions extra prone to have severe tough strolling or doing errands in comparison with kids with non-public insurance coverage alone.
Medicaid/CHIP-only kids with particular well being care wants usually tend to have an mental or developmental incapacity (I/DD) when in comparison with these with non-public insurance coverage solely (Determine 4). Against this, kids with particular well being care wants reported related prevalence of each bodily and behavioral well being disabilities throughout protection sorts. Additional, Medicaid/CHIP-only kids with particular well being care wants reporting I/DD usually tend to have co-occurring persistent situations in comparison with these with non-public insurance coverage solely (Determine 4). Solely 11% of kids with particular well being care wants with non-public insurance coverage alone reported having a bodily incapacity, behavioral well being incapacity, and I/DD collectively, in comparison with 18% of the Medicaid/CHIP solely group.
Youngsters with particular well being care wants who’ve each Medicaid/CHIP and personal insurance coverage have the best well being care wants in comparison with different teams. Over half of these with each Medicaid/CHIP and personal insurance coverage have 4 or extra purposeful difficulties, and over one-third of this group have well being situations that normally or at all times have an effect on their every day actions considerably or an ideal deal (Determine 4). These kids report increased charges of significant problem concentrating, dressing/bathing, and doing errands alone in addition to increased prevalence of I/DD and co-occurring I/DD and behavioral well being disabilities when in comparison with the Medicaid/CHIP-only inhabitants (Determine 4).
How Does Having a Baby with Particular Well being Care Wants Have an effect on Households?
Medicaid/CHIP kids with particular well being care wants discover their well being care extra reasonably priced than these with non-public insurance coverage solely. Medicaid/CHIP-only kids with particular well being care wants are greater than 4 occasions as prone to report that their out-of-pocket well being care prices are at all times affordable in comparison with these with non-public insurance coverage alone (Determine 5). Solely 3% of Medicaid/CHIP-only kids with particular well being care wants reported paying $1000 or extra in out-of-pocket medical bills in comparison with 38% of these with non-public insurance coverage alone (Determine 5). Medicaid program guidelines totally exempt sure populations and providers from premiums and copays and in any other case require cost-sharing to be nominal. This displays the truth that the Medicaid inhabitants tends to have low incomes and, as within the case of kids with particular well being care wants, might have a number of and ongoing service wants which may result in excessive prices with out cost-sharing protections.
Households of Medicaid/CHIP-only kids with particular well being care wants usually tend to face monetary problem in comparison with these with non-public insurance coverage solely. Households of Medicaid/CHIP-only kids with particular well being care wants are over 3 times as prone to discover it considerably or fairly often arduous to cowl their youngster’s primary wants and over 5 occasions as prone to generally or typically not be capable of afford sufficient to eat in comparison with these with non-public insurance coverage alone (Determine 6). Caregivers of Medicaid/CHIP-only kids with particular well being care wants additionally usually tend to scale back their hours or cease working on account of their youngster’s well being and to spend 5 or extra hours every week offering well being care at house when in comparison with these with non-public insurance coverage solely (Determine 6). In addition they are the least prone to be employed 50 weeks per yr in comparison with different protection teams, maybe reflecting the better period of time they spend caring for his or her kids’s well being wants (Determine 6).
Father or mother/caretakers of Medicaid/CHIP-only kids with particular well being care wants usually tend to face challenges with their very own well being in comparison with these with non-public insurance coverage solely. Whereas 10% of privately insured kids with particular well being care wants have a caregiver with truthful or poor bodily or psychological well being, 26% coated solely by Medicaid/CHIP have a caregiver with truthful or poor bodily well being and 19% have a caregiver with truthful or poor psychological well being (Determine 6). Moreover, Medicaid/CHIP-only kids with particular well being care wants are 3 times as prone to stay in a house with just one caregiver in comparison with these with non-public insurance coverage alone (Determine 6).
Entry to Care and Service Utilization Amongst Youngsters with Particular Well being Care Wants
Despite the fact that Medicaid/CHIP-only kids with particular well being care wants have better well being care wants, they’re extra possible than these with non-public insurance coverage alone to report that their advantages are at all times ample to satisfy their wants (Determine 5). The Medicaid/CHIP-only group is also extra prone to report that their insurance coverage meets their behavioral well being wants in comparison with these with non-public insurance coverage alone (Determine 5). These findings possible mirror Medicaid’s sturdy profit package deal for youngsters, which incorporates acute and preventive providers in addition to LTSS and HCBS, that are sometimes not coated by non-public insurance coverage. Medicaid’s Early and Periodic Screening Diagnostic and Remedy (EPSDT) profit consists of common medical, imaginative and prescient, listening to, and dental screenings in addition to the providers essential to “appropriate or ameliorate” bodily or psychological well being situations. These providers have to be offered for youngsters, no matter whether or not a state chooses to cowl them for adults. Medicaid/CHIP-only kids with particular well being care wants are much less prone to have a regular supply of sick and preventive care (Determine 7), however they’re extra prone to report their insurance coverage permits them to see wanted suppliers in comparison with these with non-public insurance coverage alone (Determine 5). The charges of kids with particular well being care wants who’ve had no less than one preventive go to up to now yr and obtained psychological well being therapy when wanted up to now yr are related throughout protection teams (Determine 7). These charges have possible worsened because of the pandemic, with kids experiencing delays in preventive care, and kids with particular well being care wants experiencing difficulties accessing specialised providers and therapies, particularly providers that might not be performed through telehealth.
Whereas Medicaid/CHIP-only kids with particular well being care wants usually tend to discover their insurance coverage advantages ample in comparison with these coated by non-public insurance coverage alone, a gaggle of those Medicaid kids just lately filed a lawsuit arguing {that a} new Part 1115 waiver in Tennessee may worsen entry to care. For particulars, see Field 1 beneath. One other problem is the change in profit package deal skilled by people who age out of complete protection offered via the Medicaid EPSDT profit at age 21. If wanted providers aren’t coated by Medicaid, this could have implications for these with persistent situations as they attempt to keep continuity of care and stay locally as they age into younger maturity, as non-public insurance coverage is unlikely to cowl LTSS and paying for providers out-of-pocket could also be unaffordable. For instance, a current New York Occasions article particulars how in New York, the change from “medically fragile youngster” to “medically fragile grownup” consists of decrease Medicaid cost charges for nurses that might end in younger adults with disabilities dropping entry to in-home providers and being pressured to maneuver into nursing houses.
Field 1: Medicaid Youngsters with Particular Well being Care Wants Problem Tennessee Medicaid Waiver Approval
A gaggle of 13 Medicaid-enrolled kids and younger adults with vital disabilities and a pediatrician who’s a Medicaid supplier have filed a federal lawsuit difficult CMS’s approval of Tennessee’s Part 1115 waiver, McCutchen v. Becerra. They argue that the waiver’s mixture cap and shared financial savings financing mannequin exceeds CMS’s authority and doesn’t additional Medicaid program aims as a result of it is going to lead the state and well being plans to decrease supplier funds and/or improve utilization controls, in flip proscribing enrollees’ entry to medically essential providers. The advanced waiver approval has nationwide significance on account of a lot of provisions, together with the financing mannequin, a closed prescription drug formulary, and a 10-year period.
The plaintiffs have a number of persistent well being situations akin to cerebral palsy, mind accidents, muscular dystrophy, spinal muscular atrophy, seizure issues, developmental delays, and several other uncommon issues. They depend on providers akin to non-public obligation nursing to observe the feeding tubes, tracheostomies, and ventilators that allow them to eat and breath; house well being and private care to assist with mobility and self-care; and prescription medicines. Below Tennessee’s waiver, they’re required to enroll in capitated managed care, and so they allege they’ve skilled service denials or restrictions, putting them vulnerable to getting into hospitals or establishments.
The plaintiffs sued the federal authorities, difficult the waiver approval, issued within the last days of the Trump Administration, although the state of Tennessee has been allowed to intervene within the case to defend the waiver. The case has been placed on maintain after CMS, below the Biden Administration, opened a brand new 30-day public remark interval on August 10, 2021 to obtain enter on the accredited waiver. The remark interval closed on September 9, 2021, and the court docket is now ready for CMS’s resolution about the best way to proceed after it critiques the feedback.
Wanting Forward
Medicaid is a big supply of protection for medical, behavioral well being, and LTSS for youngsters with particular well being care wants. As the first supply of protection for HCBS, Medicaid performs a significant position in offering kids with particular well being care wants the LTSS they should stay at house with their households. Medicaid makes protection reasonably priced by limiting cost-sharing and defending kids from excessive out-of-pocket prices and covers providers that non-public protection sometimes doesn’t, together with LTSS. Throughout the pandemic, kids have skilled well being care disruptions, psychological well being challenges, and financial hardships, and these points might have been intensified for these with particular well being care wants, making medical insurance protection, affordability, and profit package deal contents particularly vital. Specialists be aware that going to highschool in-person is useful for youngsters’s social, emotional, and bodily well being and might present entry to vital well being providers and deal with racial and social inequities. Nevertheless, uncertainty stays round what in-person studying will seem like as circumstances stay excessive because of the Delta variant, and the transition to “the brand new regular” could also be tough for some kids, particularly these whose well being and purposeful wants place them at elevated threat of COVID-19 and who might require particular training providers that might not be adequately offered remotely.
Whereas unmet want for HCBS for individuals with disabilities pre-dates the COVID-19 pandemic, the pandemic additionally has introduced a heightened focus to the necessity for added HCBS. Throughout the COVID-19 public well being emergency (PHE), states have taken a lot of emergency Medicaid LTSS actions, akin to HCBS profit expansions and supplier cost charge will increase for HCBS. CMS has inspired states to think about making these modifications everlasting, although states would require ample financing to retain many coverage modifications. Moreover, state actions to unwind emergency authorities and resume common eligibility renewals on the finish of the PHE have implications for sustaining continuity of protection and providers.
The ARPA supplies a brief 1-year improve in federal matching funds for spending on Medicaid HCBS, although the federal coverage debate in regards to the extent to which elevated HCBS funding ought to be prolonged is continuous. A current KFF survey discovered that a couple of states reported plans to direct a number of the new ARPA funds to assist household caregivers. Current CMS steering confirms that states might use these funds to pay household caregivers, present tools and provides, and supply respite care. Though President Biden earlier this yr proposed a $400 billion federal funding over 10 years to increase entry to Medicaid HCBS and strengthen the direct care workforce, it’s unclear how a lot of that funding improve can be accredited by Congress because it considers competing priorities within the price range package deal and calls amongst some to scale back the general spending stage. The reconciliation invoice being thought of by the Home consists of $190 billion for HCBS. Elevated federal funding for Medicaid HCBS past the present 1-year may allow states to assist the HCBS supplier workforce, supply new or expanded HCBS advantages, and/or serve extra HCBS enrollees, all of which may profit kids with particular well being care wants.
| The info on this evaluation draw from the 2019 Nationwide Survey of Youngsters’s Well being (NSCH), essentially the most present information out there. The NSCH and this evaluation use the CSHCN Screener to determine kids with particular well being care wants. To satisfy the factors for having a particular well being care want, a toddler should expertise a well being consequence that is because of a medical or different well being situation that has lasted or is anticipated to final for 12 months or longer. This evaluation breaks down indicators by medical insurance protection standing for youngsters with particular well being care wants however doesn’t embrace estimates for uninsured kids or kids who didn’t report protection standing. This is because of most of the estimates for these kids not assembly the minimal requirements for reliability. |