Many people who’re sufferers have the disagreeable expertise of navigating the advanced world of drug utilization administration. This contains figuring out what formulary tier a drug will likely be on, if there are any prior authorization necessities and what our copay will likely be. The burden additionally falls on physicians in that they should justify why particular medicine are wanted for a given affected person to safe protection. Drug firms even have prices for applications to assist sufferers and physicians navigate the utilization administration applications, rebates, free samples, and co-payment help. Payers even have the extra value of administering these utilization administration applications. The truth that utilization administration imposes prices on quite a lot of stakeholders isn’t a surprise. In actual fact, the aim is to impose prices on completely different stakeholders to incentivize using decrease value medicines. One unanswered query, nonetheless, is how giant these prices truly are.
A latest paper in Well being Affairs by Howell, Yin and Robinson, discover that the annual value within the US is $93.3 billion. Sufferers bear the biggest burden at $35.8 billion with physicians ($26.7 billion) and producers ($24.8 billion) coming in at second and third place. Payers value is far smaller however not trivial at $6.0 billion.
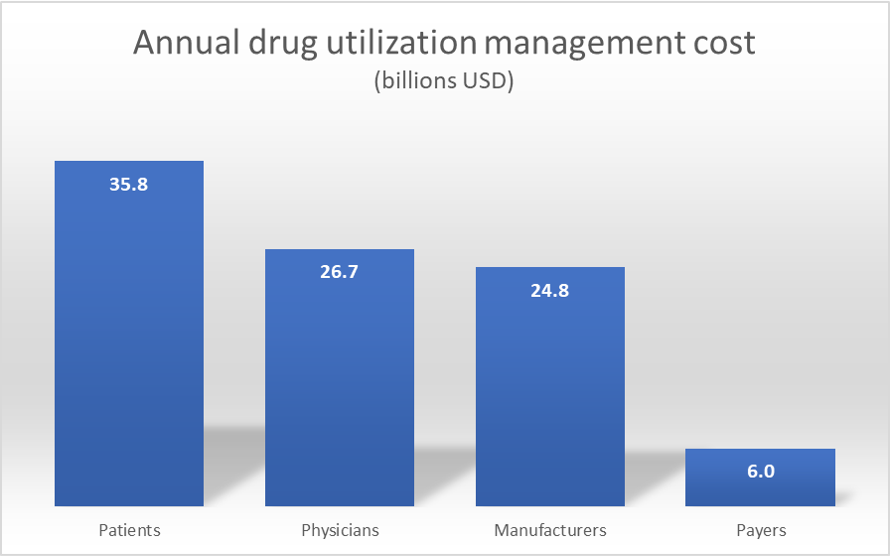
The authors attain these conclusion by conducting a literature overview of peer-reviewed research revealed between 2009 and 2020 supplemented by different information articles.
The authors argue one resolution to the utilization administration arms race, can be for producers to cost medicine primarily based on therapy worth in alternate for PBMs/payers to permit “value-based entry” with minimal utilization administration restrictions. Whereas wise, figuring out an acceptable notion of “worth” is usually difficult. Nonetheless, eradicating boundaries to affected person entry is a laudable aim.