Initially of the “unwinding” interval, in April 2023, Medicaid enrollment peaked at 94.5 million, a rise of 23 million or 32% from earlier than the pandemic. As of December 2023, Medicaid enrollment declined by greater than 9% throughout states, a decline of over 8 million folks. The Facilities for Medicare and Medicaid Providers (CMS) continues to focus on the position managed care organizations (MCOs) can play in serving to folks eligible for Medicaid use and hold their protection, as practically three-quarters of Medicaid beneficiaries are enrolled in a managed care plan. This temporary takes a more in-depth have a look at the 5 largest publicly traded corporations (additionally known as “mum or dad” companies) working Medicaid MCOs, which account for half of Medicaid MCO enrollment nationally. This evaluation presents the newest mum or dad agency enrollment and monetary knowledge (via the tip of CY 2023) in addition to key takeaways from the companies’ unwinding expertise. Info and knowledge reported on this temporary come from quarterly firm earnings reviews and calls, monetary filings and different firm supplies in addition to from nationwide administrative knowledge. Key takeaways embrace:
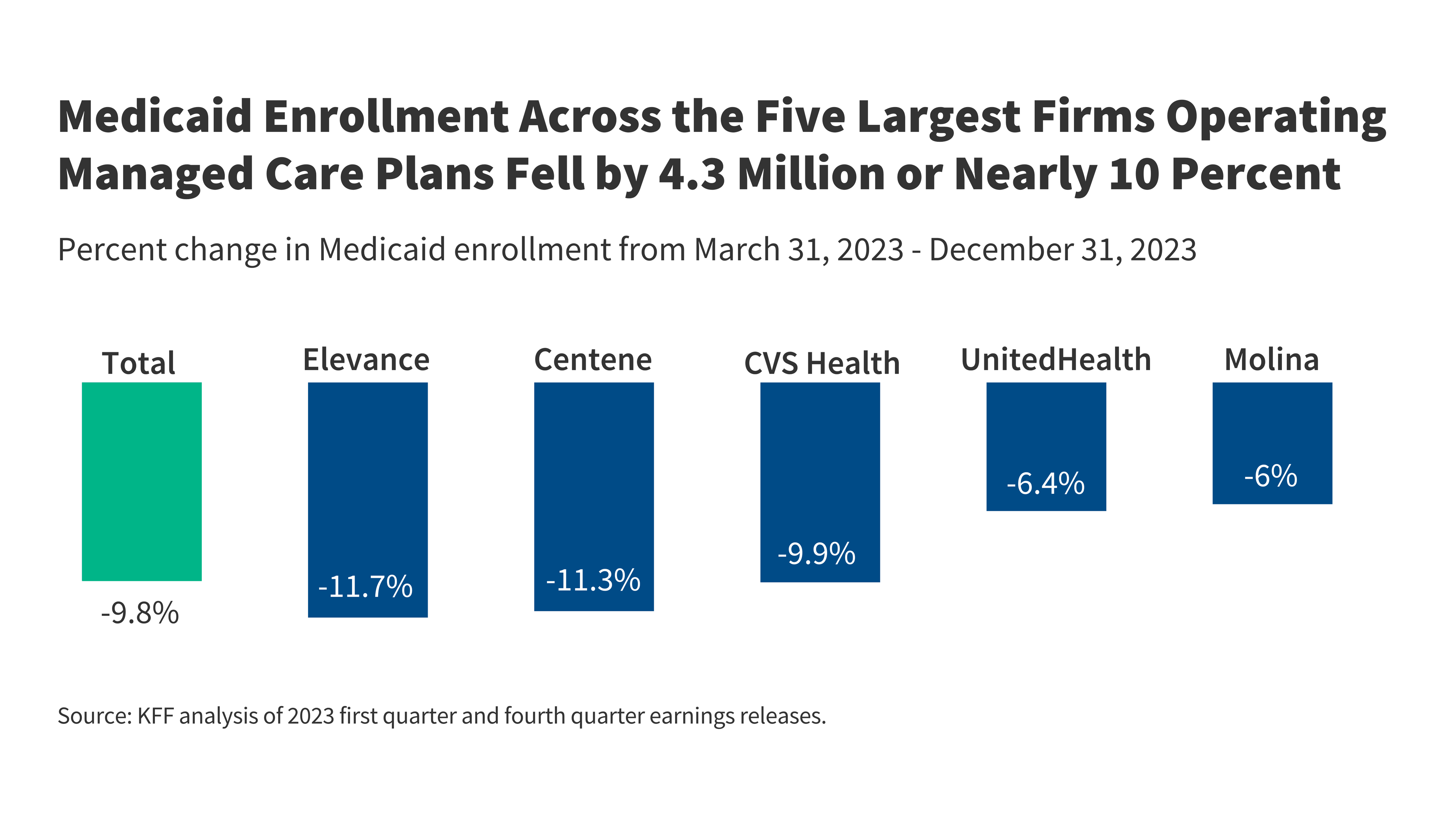
- Medicaid Enrollment. From March 2023 to December 2023, Medicaid enrollment declined by practically 10% throughout the 5 companies, monitoring the speed of decline seen nationally.
- Medicaid Income. Though companies noticed a ten% decline in Medicaid enrollment as of the tip of 2023, the companies that report Medicaid-specific income data reported year-over-year (2023 over 2022) progress in Medicaid income starting from 3% to 18%.
- Unwinding Impacts. In earnings calls, companies have mentioned the impacts of unwinding, together with excessive procedural disenrollment charges of 70% or above and gaps in member protection that may prolong for a number of months. A number of companies reported states have been making mid-cycle and retrospective fee changes to account for the impression of redeterminations on the common danger profile (or “acuity”) of members who stay enrolled.
Medicaid enrollment within the 5 largest publicly traded corporations working Medicaid MCOs
5 for-profit, publicly traded corporations – Centene, Elevance (previously Anthem), UnitedHealth Group, Molina and CVS Well being – account for 50% of Medicaid MCO enrollment nationally (Determine 1). All 5 are ranked within the Fortune 500, and 4 are ranked within the high 100, with complete revenues that ranged from $34 billion (Molina) to $372 billion (UnitedHealth Group) for 2023. Every firm operates Medicaid MCOs in 14 or extra states (Determine 2).
All 5 companies additionally function within the business and Medicare markets (Determine 3); nevertheless, the distribution of membership throughout markets varies throughout companies. Two companies – Molina and Centene – have traditionally centered predominantly on the Medicaid market. Medicaid members accounted for over 90% of Molina’s total medical membership and practically 65% of Centene’s medical membership as of December 2023 (Determine 3). Because the begin of unwinding, Medicaid membership as a share of complete medical membership has declined for all 5 companies. The unwinding could also be contributing to membership distribution shifts.
Mixed Medicaid enrollment throughout the 5 companies decreased by 4.3 million or 9.8% from March 2023 to December 2023 (Determine 4). Much like the enrollment decline skilled by the 5 mum or dad companies, nationwide knowledge present complete Medicaid/CHIP enrollment declined by greater than 9% from March 2023 to December 2023. Modifications in “internet” enrollment mirror the people who find themselves dropped from Medicaid in addition to those that newly enroll, and people who re-enroll inside a brief timeframe following disenrollment, often known as “churn.” Modifications in mum or dad agency enrollment might mirror exercise together with agency acquisitions or gross sales and new or misplaced Medicaid contracts. Though Medicaid enrollment has declined throughout mum or dad companies for the reason that begin of the unwinding, the three companies that report Medicaid-specific income data (UnitedHealth, Molina, and Centene) reported year-over-year (2023 over 2022) progress in Medicaid income (18%, 6%, and three%, respectively). Molina reported the medical margin earned by the Medicaid phase was $3.0 billion in 2023 (medical margin = premium income – medical prices). Since enrollment declines escalated all through 2023, it’s potential that the Medicaid income image for these companies might worsen within the coming months. Nonetheless, it’s additionally potential that insurers have been in a position to preserve Medicaid revenues regardless of enrollment declines partially via retrospective fee changes.
Influence of unwinding for the 5 largest publicly traded corporations working Medicaid MCOs
All 5 companies report monitoring the impression of unwinding, together with disenrollment, “churn”, protection transitions, gaps in protection, and modifications in member acuity. Key highlights from Q2 – This fall 2023 earnings calls embrace:
- Procedural Disenrollment. In earnings calls for the reason that begin of the unwinding, companies have reported procedural disenrollments make up a big share of their complete disenrollments. Corporations that offered estimates reported procedural disenrollment charges of 70% or above. Procedural disenrollments happen when an enrollee is unable to finish the renewal course of. Elevance reported that disenrolled members are going through obstacles to renewal, together with consciousness of the method and actions required to keep up protection. In Q3 2023, Elevance reported that almost 40% of their Medicaid members procedurally disenrolled have been youngsters/youth (beneath age 18). KFF monitoring exhibits, total, about 70% of disenrollments up to now have been “procedural,” however the fee varies considerably throughout states. Many methods can be found to states to attenuate procedural terminations, together with non permanent waivers that permit states to acquire up to date enrollee contact data from MCOs, allow MCOs to help enrollees in finishing sure components of renewal varieties, and prolong automated reenrollment into an MCO plan from the usual 60 days as much as 120 days.
- “Churn”. In response to agency monitoring, some people who’ve been disenrolled are reenrolling in Medicaid protection. Corporations report persevering with with outreach efforts to assist folks retain or regain their Medicaid protection or discover different inexpensive protection. Of the companies that shared this data, Medicaid reenrollment charges ranged from 20-30%. Centene famous that CMS motion requiring states to reinstate protection as a consequence of programs points has impacted reenrollment charges.
- Protection Transitions. Corporations are additionally monitoring transitions to protection via the Reasonably priced Care Act (ACA) Market. All 5 companies provide a Market plan in lots of states the place they function a Medicaid MCO, nevertheless, there will not be plan alignment if plans function regionally. Centene reported 10-15% of members disenrolled from Medicaid transitioned to their Market product. Different companies haven’t offered particular Market transition charges/estimates however word one driver of Market progress has been Medicaid redeterminations. Some people eligible for protection within the Market (which has greater revenue eligibility thresholds than Medicaid) qualify for plans with zero premiums; nevertheless, Medicaid might present extra complete advantages and decrease cost-sharing in comparison with Market protection. Latest knowledge present that Market signups have reached 21.3 million folks, exceeding final yr’s report excessive by one other 5 million folks. Medicaid unwinding is just one issue contributing to that progress – which is being pushed largely by enhanced premium subsidies – and a comparatively small share of individuals disenrolled from Medicaid are transitioning to Market or Fundamental Well being Plan protection.
- Gaps in Protection. Some enrollees are experiencing gaps in protection that, in response to some companies, can prolong for a number of months. That is in keeping with a pre-pandemic evaluation of nationwide survey knowledge that present two-thirds of enrollees expertise a interval of uninsurance within the 12 months following Medicaid disenrollment. In focus teams performed by KFF in September 2023 with Medicaid enrollees who not too long ago accomplished the renewal course of, a number of contributors who have been disenrolled reported going through substantial out-of-pocket prices for medically needed care throughout gaps in protection. Focus group contributors additionally reported needing one-on-one help from caseworkers and community-based organizations to assist them regain Medicaid protection.
- Member Acuity. In earnings calls, a number of companies reported states have been making mid-cycle and retrospective fee changes to account for the impression of redeterminations on common member acuity (i.e., well being standing, which might have an effect on use of providers and medicines). Though states might have constructed enrollment and acuity change assumptions into capitation charges (for 2023 and 2024), states and plans confronted appreciable uncertainty firstly of the unwinding–understanding that whereas membership losses would turn out to be instantly obvious, new utilization and acuity tendencies would take longer to discern. Previous to the beginning of unwinding, plans reported anticipating the general danger profile of members to extend, as they anticipated “stayers” can be sicker than “leavers.” No less than one agency famous continued results of danger corridors (the place states and plans conform to share revenue or losses) from earlier contract years, requiring plan payback.
Wanting Forward
As of December 2023 (timeframe for this evaluation), states have been 9 months into the unwinding of the Medicaid steady enrollment provision. It’s extremely unsure what nationwide Medicaid enrollment will likely be on the finish of unwinding. Focus teams with enrollees revealed that whereas many have been in a position to efficiently renew Medicaid protection, many have been disenrolled as a consequence of confusion and obstacles to finishing the renewal course of. Whereas many people who’re disenrolled might “churn” again to Medicaid or transition to different protection, unwinding will possible contribute to will increase within the variety of people who find themselves uninsured. People who find themselves uninsured face extra obstacles to care, go with out wanted care, and should expertise greater out of pocket prices and medical debt. Modifications within the uninsured will rely upon whether or not people who’re not eligible and are disenrolled from Medicaid transition to different protection, together with employer plans and the Market. Medicaid managed care plans have a monetary curiosity in sustaining enrollment in Medicaid and facilitating transitions to the Market (and different merchandise). The 5 publicly traded companies which are the topic of this evaluation account for about half of all Medicaid MCO enrollment nationally. Medicaid managed care plans can proceed to help state Medicaid businesses in speaking with enrollees, conducting outreach and renewal help, and in facilitating transitions to Market protection. Quarterly earnings reviews and calls can present additional perception into the impression of the unwinding on Medicaid enrollees, together with disenrollments, gaps in protection and transitions to the Market.