Medicare beneficiaries might select to obtain their Medicare advantages by conventional Medicare or a Medicare Benefit plan supplied by a personal medical insurance firm. Over the previous 15 years, the share of Medicare beneficiaries enrolled in Medicare Benefit plans has greater than doubled, approaching half of the full Medicare inhabitants. One motive for the expansion in Medicare Benefit enrollment could also be that nearly all plans provide additional advantages not out there in conventional Medicare, together with protection of imaginative and prescient (eyeglasses and/or eye exams), listening to (exams and/or aids), health, and dental providers.
Companies that sponsor Medicare Benefit plans have the flexibility to find out what, if any, additional advantages to supply, and these choices could also be made with the purpose of attracting and retaining enrollees. Agency participation within the Medicare Benefit market is powerful, with the common Medicare beneficiary ready to select from 43 plans supplied by 9 corporations in 2023 (just like 2022). Regardless of having broad choices, enrollment is extremely concentrated, with UnitedHealthcare and Humana accounting for greater than 40 p.c of all Medicare Benefit enrollees since 2015, and a excessive of 46 p.c in 2022.
This evaluation examines how the share of enrollees in plans that provide additional advantages varies throughout corporations, based mostly on an evaluation of CMS Medicare Benefit plan profit and enrollment recordsdata (for extra info, see Strategies field). We deal with variations throughout corporations based mostly on 2022 enrollment, as a result of plan enrollment for 2023 isn’t but out there. As well as, we offer an summary of how the 2023 plan choices, by agency, differ from choices in 2022. We restricted the evaluation to particular person Medicare Benefit plans which might be typically out there to all beneficiaries for enrollment (which, for instance, excludes plans sponsored by employers/unions and particular wants plans which might be supplied to an outlined group of beneficiaries). We current findings for the seven corporations with the biggest market share in 2022, representing greater than four-fifths (83%) of Medicare Benefit enrollment – UnitedHealthcare (24%), Humana (20%), Blue Cross Blue Defend (15%), CVS Well being (10%), Kaiser Permanente (6%), Centene (5%), and Cigna (2%).
This evaluation seems at what number of enrollees are in plans that provide varied additional advantages however doesn’t look at how the scope of those advantages varies throughout plans or insurers. Prior KFF evaluation documented substantial variation within the scope of dental advantages supplied throughout Medicare Benefit plans, based mostly on an in depth evaluate of every plan’s Proof of Protection, that’s past the scope of this evaluation which depends on public information recordsdata. Moreover, we don’t look at utilization or out-of-pocket spending related to these additional advantages, as a result of plans are usually not required to report these information for supplemental advantages.
Share of Medicare Benefit enrollees in plans with additional advantages, by agency
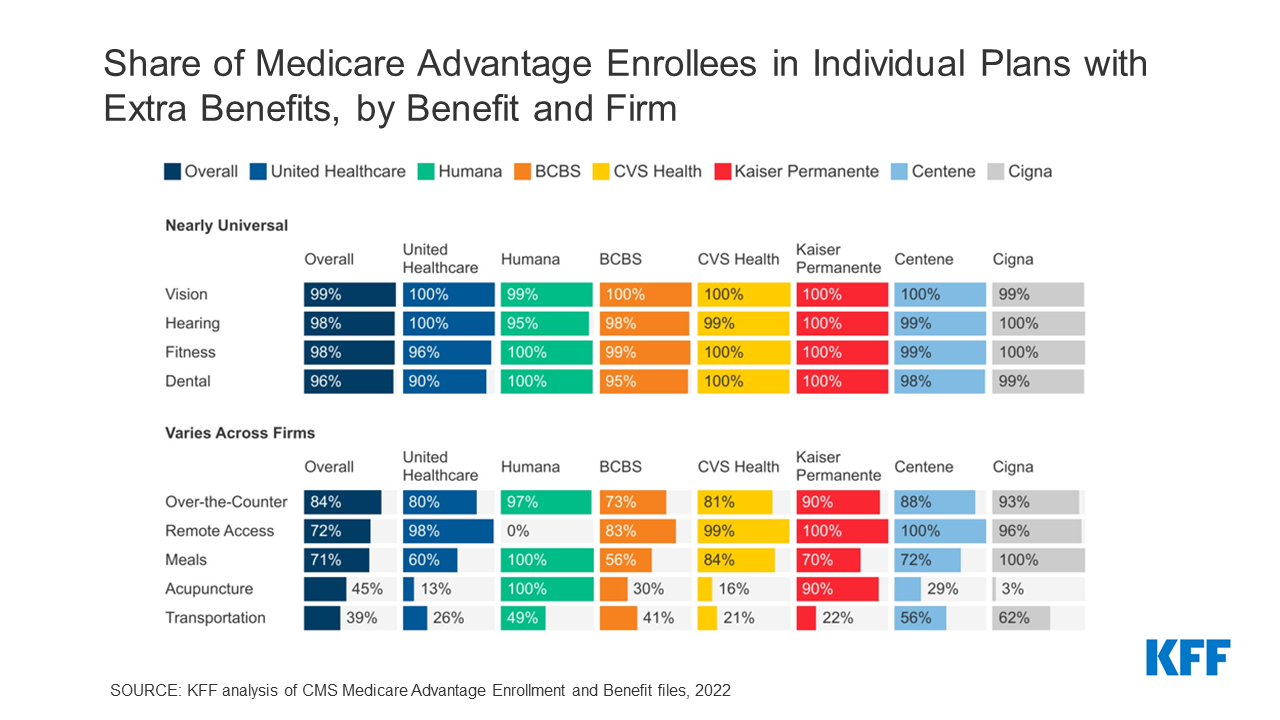
Throughout the seven largest corporations within the Medicare Benefit market that collectively account for 83% of all enrollees, there’s close to common enrollment in plans that provide imaginative and prescient, listening to, health, and dental advantages. There’s extra variation throughout corporations for over-the-counter, distant entry applied sciences, meals, acupuncture and transportation advantages. It’s unusual for plans to supply different advantages, with a comparatively small share of enrollees throughout all corporations in plans that provide in-home assist providers, lavatory security, Medicare Half B premium rebates, telemonitoring or caregiver assist advantages. Determine 1 reveals the share of enrollees in plans that provide every of 14 completely different additional advantages that we examined, by agency, in 2022.
Almost all enrollees are in Medicare Benefit plans that provide imaginative and prescient, listening to, health and dental advantages.
General, nearly all Medicare Benefit enrollees are in plans that provide protection of some imaginative and prescient (99%), listening to (98%), health (98%), and/or dental (96%) providers. Whereas protection is almost common, there are some small variations throughout corporations.
A minimum of 95 p.c of enrollees in plans sponsored by the corporations we examined are supplied imaginative and prescient, listening to and/or health advantages. Throughout all corporations, there’s little distinction within the share of enrollees in who’re supplied no less than some imaginative and prescient providers, resembling eye exams and/or eyeglasses, with no less than 99 p.c of enrollees in a plan that gives this profit. Listening to and health advantages are additionally practically universally supplied, although a barely smaller share of Humana enrollees (95%) are in a plan that covers listening to advantages and barely smaller share of UnitedHealthcare enrollees (96%) are supplied health advantages, in comparison with the nationwide common.
The share of enrollees in a plan that gives dental advantages ranges from 90 p.c amongst UnitedHealthcare enrollees to 100% for Humana, CVS Well being, and Kaiser Permanente enrollees. Protection of dental providers can be practically universally supplied to enrollees in Centene (98%) and Cigna (99%) plans. As famous earlier, prior KFF evaluation has documented broad variation within the scope of dental advantages supplied by plans, starting from preventive providers completely to extra complete protection.
The share of Medicare Benefit enrollees in plans that provide over-the-counter, distant entry applied sciences, meal, acupuncture, and transportation advantages varies extra throughout corporations.
General, a majority of Medicare Benefit enrollees are in a plan that gives over-the-counter (84%), distant entry applied sciences (72%), or meal (71%) advantages, whereas a considerably smaller share are enrolled in plan with acupuncture (45%) or transportation (39%) advantages. Throughout corporations, nevertheless, there are notable variations.
Among the many two corporations with the biggest enrollment, a smaller share of UnitedHealthcare than Humana enrollees are in plans that provide over-the-counter, meal, acupuncture and transportation advantages. Whereas UnitedHealthcare has the biggest market share (each traditionally and at present), a smaller share of enrollees in plans sponsored by UnitedHealthcare than Humana (the insurer with the second highest enrollment) are supplied over-the-counter (80% vs 97%), meals (60% vs 100%), acupuncture (13% vs 100%), and transportation (26% vs 49%) advantages. The one exception amongst advantages that modify throughout corporations is distant entry applied sciences, the place practically all enrollees (98%) in a UnitedHealthcare plan are supplied expanded telehealth advantages that embody distant entry applied sciences, whereas no Humana enrollees are in a plan that gives this profit.
The 2 corporations with the smallest Medicare Benefit market share, Centene and Cigna, provide transportation advantages to the biggest share of enrollees. Transportation advantages are supplied to 56 p.c of Centene enrollees and 62 p.c of Cigna enrollees. No different agency affords this profit to a majority of enrollees, with 49 p.c of Humana enrollees, 41 p.c of Blue Cross Blue Defend enrollees, 26 p.c of UnitedHealthcare enrollees, and simply over one fifth of CVS Well being (21%) and Kaiser Permanente (22%) enrollees in a plan that gives a transportation profit.
It’s unusual for Medicare Benefit enrollees to be in plans that provide in-home assist providers, lavatory security, Half B rebates, telemonitoring, or caregiver assist.
A comparatively small share of Medicare Benefit enrollees are in a plan that gives in-home assist providers (12%), lavatory security gadgets (9%), a rebate towards the Half B premium (7%), telemonitoring (4%), or assist for caregivers (4%).
Enrollees in Blue Cross Blue Defend plans are enrolled considerably extra typically in a plan that gives in-home assist providers, lavatory security, telemonitoring, or caregiver assist advantages than enrollees in plans sponsored by different corporations. Amongst enrollees in Blue Cross Blue Defend plans, 29 p.c are in a plan that gives in-home assist providers, in comparison with 23 p.c in Centene plans, 12 p.c in Cigna plans, 10 p.c in Humana plans, 7 p.c in Kaiser Permanente plans, and no enrollees in UnitedHealthcare or CVS Well being plans. Equally, 36 p.c of Blue Cross Blue Defend enrollees are in a plan that covers lavatory security gadgets, whereas simply 7 p.c of Cigna enrollees and fewer than 2 p.c of enrollees in plans sponsored by different corporations are supplied this profit. Telemonitoring and caregiver assist advantages are supplied completely by Blue Cross Blue Defend among the many corporations examined. Amongst Blue Cross Blue Defend enrollees, 15 p.c are in a plan that gives telemonitoring providers and 11 p.c are in a plan with caregiver assist advantages, whereas no enrollees in plans sponsored by different corporations are supplied these advantages.
Throughout Medicare Benefit corporations, a comparatively small share of enrollees are in a plan that gives a rebate towards the month-to-month Medicare Half B premium. Medicare beneficiaries in each conventional Medicare and Medicare Benefit plans are answerable for paying a month-to-month Medicare Half B premium. Some plans present a rebate that reduces the premium as an additional profit. Apart from Kaiser Permanente, all corporations have no less than some enrollees in a plan that gives a rebate in direction of the Medicare Half B premium. Centene has a bigger share than different corporations, with 26 p.c of enrollees in a plan with this profit, adopted by Humana (11%), Cigna (9%), CVS Well being (6%), UnitedHealthcare (4%) and Blue Cross Blue Defend (4%).
Outlook for 2023
The primary launch of Medicare Benefit plan profit bundle information for 2023 present only a few modifications in what’s being supplied with respect to the additional advantages that we examined on the agency stage. For instance, UnitedHealthcare is providing meal advantages in 83 p.c of its plans in 2023, in comparison with simply over half in 2022. Each Humana and Blue Cross Blue Defend have elevated the share of plans providing in-home assist providers (from 4% of plans in 2022 to 11% of plans in 2023 for Humana; from 20% of plans in 2022 to 27% of plans in 2023 for Blue Cross Blue Defend). Cigna is providing caregiver assist providers in 17 p.c of plans after not providing this profit in any particular person plans open for basic enrollment in 2022. Lastly, Half B premium rebates are included in a considerably bigger share of plans sponsored by Cigna (30% in 2023 in comparison with 18% in 2022), Humana (22% in 2023 in comparison with 14% in 2022) and Blue Cross Blue Defend (14% in 2023 in comparison with 8% in 2022). Collectively, these modifications imply that the share of Medicare Benefit enrollees in plans that provide additional advantages by agency might differ barely in 2023, however there are unlikely to be massive, broad modifications.
Dialogue
Almost all enrollees in Medicare Benefit plans sponsored by the seven largest corporations out there are in a plan that gives some imaginative and prescient, listening to, health, and/or dental advantages, however different advantages differ broadly throughout corporations or are comparatively unusual. This differentiation might symbolize firm-level methods to draw and retain enrollees and develop their share of the Medicare Benefit market. Companies could also be trying to entice enrollees from their rivals by providing additional advantages which might be thought of precious (partially, as a result of they doubtlessly enhance well being or decrease prices), and tailoring these advantages to explicit subgroups of beneficiaries.
Plans are capable of provide further advantages, partially as a result of Medicare spends extra per enrollee in Medicare Benefit than it spends per individual in conventional Medicare. Particularly, rebates paid by Medicare to plans (based mostly on the distinction between the bid and the benchmark), that are used to fund additional advantages, have elevated quickly in recent times, rising to just about $2,000 per enrollee on common in 2022. Of that quantity, plans are estimated to spend a median of $480 per enrollee on additional advantages general, together with Half B premium rebates. We should not have the info to know the way that quantity varies throughout corporations, and so we can’t assess particularly whether or not corporations with bigger rebates provide extra or completely different additional advantages. It’s doable that sure plans preserve extra of their rebate {dollars} for revenue (topic to assembly medical loss ratio necessities) or allocate extra of their rebate {dollars} in direction of a decrease out-of-pocket cap or lowered value sharing for Medicare-covered providers.
The Facilities for Medicare and Medicaid Providers (CMS) has mentioned that “Medicare Benefit is a essential a part of CMS’ imaginative and prescient to advancing well being fairness.” The variation in additional advantages throughout Medicare Benefit plans might have implications for the way efficient personal plans are on this position. Broad variations in advantages may very well be in line with the purpose if corporations are tailoring and offering advantages, resembling transportation, to these with the best social or medical wants. These variations may additionally exacerbate disparities if the additional advantages are usually not sufficiently centered on high-need populations. Plans are usually not at present required to report info on utilization or prices related to additional advantages, nor details about the community of suppliers for additional advantages, generally, or for particular subgroups. Beginning with plan 12 months 2023, some value info shall be required as a part of the medical loss ratio reviews. Nonetheless, there’ll proceed to be no details about how utilization of additional advantages, and related spending, varies by race/ethnicity, revenue, or well being standing, so it’ll stay unattainable to evaluate whether or not, and the extent to which, additional advantages are having an impression on well being outcomes for these with the best wants.
Medicare Benefit is projected to quickly turn into the primary type of Medicare protection. Understanding the advantages supplied to Medicare Benefit enrollees, how they differ throughout corporations, and the way they differ from these out there to conventional Medicare beneficiaries is vital for understanding how rising enrollment in Medicare Benefit plans is redefining what it means to have Medicare protection, in addition to the consequences on well being fairness. As extra beneficiaries obtain their protection by a personal plan, the variation in additional advantages supplied, in addition to the scope and generosity of these advantages, implies that Medicare protection may look meaningfully completely different for various folks.
This work was supported partially by Arnold Ventures. KFF maintains full editorial management over all of its coverage evaluation, polling, and journalism actions.
| Supplemental advantages in Medicare Benefit plans had been recognized utilizing the 2022 and 2023 Quarter 1 Facilities for Medicare & Medicaid Providers (CMS) Plan Profit Bundle information. Enrollment information are from the March 2022 Month-to-month Enrollment by Contract/Plan/State/County printed by CMS within the Medicare Benefit (MA)/Half D Contract and Enrollment Knowledge part. Enrollment information is simply supplied for plan-county mixtures which have no less than 11 beneficiaries; thus, we exclude any plans that don’t meet this enrollment threshold. We additionally excluded all employer plans, value plans, Well being Care Prepayment Plans (HCPP), Program of All-Inclusive Take care of the Aged (PACE) plans, and Medicare-Medicaid plans (MMP). Employer plans are usually not required to submit all information vital for the evaluation. The opposite plans eliminated have completely different enrollment necessities, and in some instances are paid otherwise, than conventional Medicare Benefit plans.
We don’t look at all the additional advantages that Medicare Benefit plans provide. For instance, we don’t look at particular supplemental advantages for the chronically unwell. Moreover, we don’t embody primary telehealth providers as an additional profit on this evaluation. Whereas these telehealth providers are usually not routinely coated by conventional Medicare (outdoors the COVID-19 public well being emergency), since 2019 Medicare Benefit plans are permitted to incorporate telehealth related prices of their bids, slightly than paying for them as a supplemental profit utilizing rebates. The overwhelming majority of Medicare Benefit enrollees (98%) are in a plan that gives primary telehealth providers. We outline a plan as providing a profit whether it is out there to enrollees as both a compulsory or non-obligatory supplemental profit. Non-obligatory supplemental advantages require a further premium, which we don’t look at on this evaluation. |