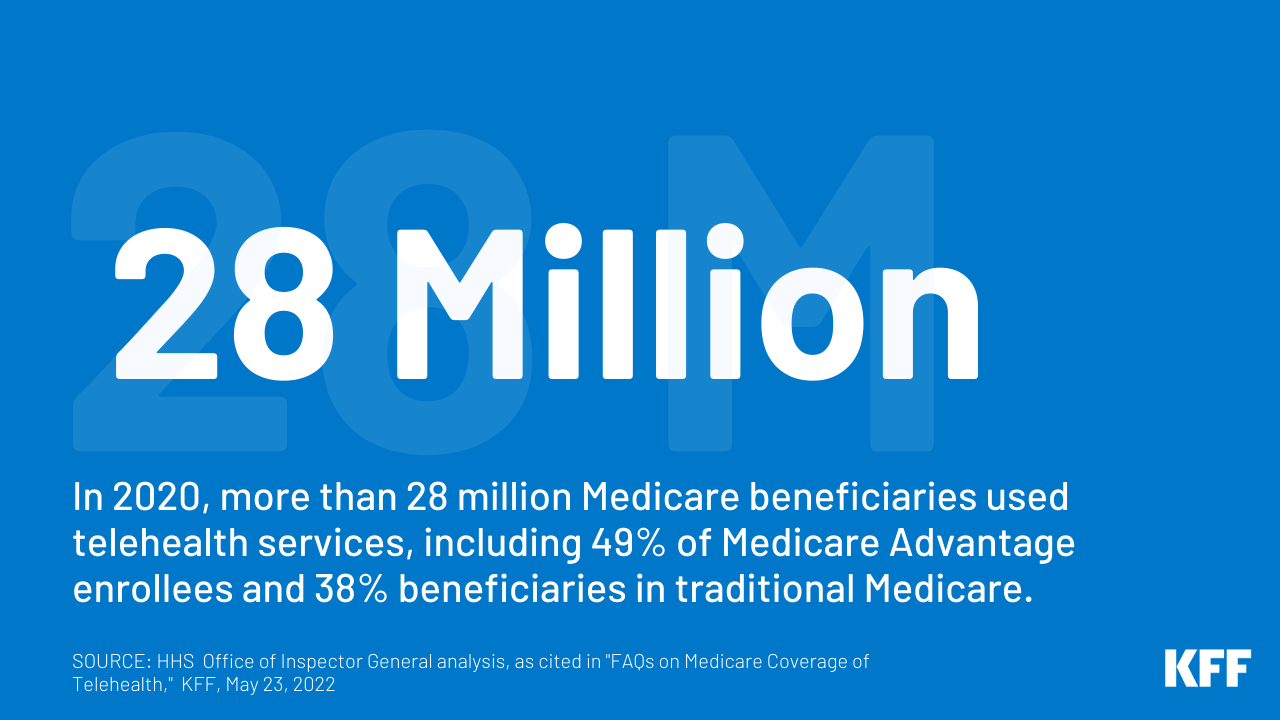
Telehealth, the availability of well being care companies to sufferers from suppliers who will not be on the identical location, has skilled a fast escalation in use throughout the COVID-19 pandemic, amongst each privately-insured sufferers and Medicare beneficiaries. Previous to the pandemic, telehealth utilization amongst conventional Medicare beneficiaries was extraordinarily low, with solely 0.3% of conventional Medicare beneficiaries enrolled in Half B utilizing telehealth companies in 2016. Between 2019 and 2020, the variety of telehealth visits in conventional Medicare elevated 63-fold. Through the first 12 months of the pandemic, greater than 28 million Medicare beneficiaries general used telehealth companies, together with virtually half (49%) of Medicare Benefit enrollees and almost 4 in 10 (38%) beneficiaries in conventional Medicare.
These FAQs present solutions to questions on Medicare’s present protection of telehealth, adjustments made on the outset of the general public well being emergency, extra adjustments adopted by Congress and the Administration, and a few of the coverage concerns that lie forward.
What’s the present scope of Medicare telehealth protection and the way did it change at first of the COVID-19 pandemic?
Underneath present legislation and laws, Medicare covers a broad scope of companies through telehealth with out restrictions that had been in place previous to the COVID-19 pandemic, however, for essentially the most half, this broader protection is obtainable solely briefly. Folks with Medicare can now entry telehealth companies, whether or not in city or rural areas, at dwelling or in different settings, utilizing audio-visual or audio-only applied sciences, and from a variety of well being care suppliers. This is because of a broad however time-limited growth of telehealth protection in Medicare throughout the COVID public well being emergency. To make it simpler and safer for beneficiaries to hunt medical care throughout the pandemic, in March 2020, the Secretary of the Division of well being and Human Providers (HHS) waived sure restrictions on Medicare protection of telehealth companies for Medicare beneficiaries throughout the COVID-19 public well being emergency, primarily based on waiver authority included within the Coronavirus Preparedness and Response Supplemental Appropriations Act (and as amended by the CARES Act) (Determine 1). The general public well being emergency was most just lately renewed in April 2022, and the Biden Administration has stated that it’ll present a 60-day discover earlier than permitting the general public well being emergency to run out. As a result of the Biden Administration has not but supplied a 60-day discover that the general public well being emergency will finish, it’s probably the PHE will lengthen past July.
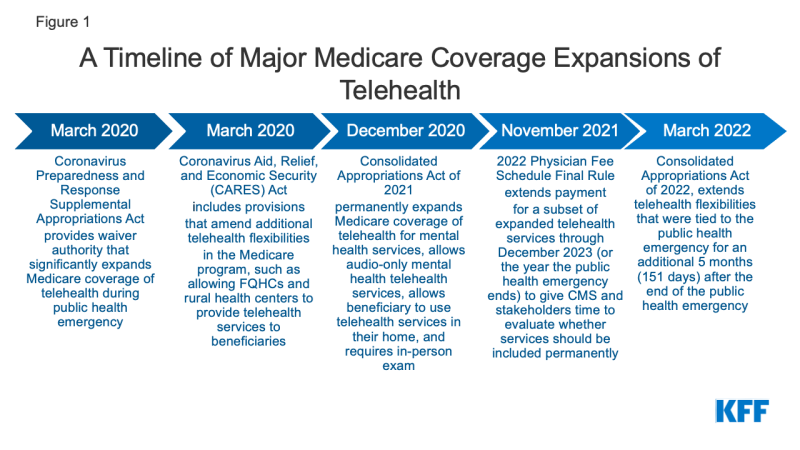
Determine 1: A Timeline of Main Medicare Protection Expansions of Telehealth
The Consolidated Appropriations Act of 2022 (CAA of 2022) prolonged lots of the latest expansions of Medicare’s telehealth protection for roughly 5 months (151 days) after the tip of the COVID-19 public well being emergency. This implies, for instance, if the general public well being emergency ends in October 2022, Medicare protection of telehealth would revert to extra restricted protection in March 2023, and most beneficiaries in conventional Medicare would lose entry to telehealth protection for many companies, aside from psychological well being companies (see beneath for extra data). It’s because earlier than the pandemic, protection of telehealth companies beneath Medicare was restricted to rural beneficiaries utilizing telehealth at an “originating website,” comparable to a clinic or physician’s workplace, quite than from their very own houses. There have been additionally restrictions on which suppliers may very well be paid to ship telehealth companies (i.e., “distant website” suppliers). There was additionally a comparatively restricted set of companies that may very well be coated by telehealth. (Medicare Benefit plans have flexibility to supply extra telehealth advantages past these which are coated by conventional Medicare outdoors of the general public well being emergency, as described beneath).
What companies can Medicare beneficiaries obtain via telehealth?
Earlier than the general public well being emergency, Medicare coated about 100 companies that may very well be administered via telehealth, together with workplace visits, psychotherapy, and preventive well being screenings, amongst different companies. Through the public well being emergency, the listing of allowable telehealth companies coated beneath Medicare has expanded to incorporate emergency division visits, bodily and occupational remedy, and sure different companies. Some analysis and administration, behavioral well being, and affected person training companies will be supplied to sufferers through audio-only phone.
Within the 2022 doctor charge schedule ultimate rule, the Facilities for Medicare & Medicaid Providers (CMS) briefly prolonged protection for a subset of the expanded telehealth companies via December 31, 2023 (or via the tip of the 12 months wherein the general public well being emergency ends, whichever is later) to present each CMS and stakeholders time to guage whether or not they need to be completely included as Medicare-covered telehealth companies. These companies embody bodily and occupational remedy, end-stage renal illness (ESRD) visits, emergency division visits, essential care companies, and others.
What psychological well being telehealth companies can be found for Medicare beneficiaries?
Telehealth has performed an vital function throughout the COVID-19 pandemic in offering entry to psychological well being companies for older adults, one in 4 of whom reported nervousness or melancholy in August 2020. Through the first 12 months of the pandemic, a big share of Medicare beneficiaries’ behavioral well being companies had been performed through telehealth, and a bigger share of behavioral well being companies had been delivered through telehealth for beneficiaries in conventional Medicare (16%) than enrollees in Medicare Benefit (9%).
Based mostly on provisions within the Consolidated Appropriations Act of 2021, policymakers have completely expanded protection for telehealth companies for the aim of analysis, analysis, or remedy of psychological well being issues after the tip of the COVID-19 public well being emergency. Medicare beneficiaries can use telehealth for psychological well being companies of their houses, and beneficiaries who can’t use real-time two-way audio and video for telehealth psychological well being companies are permitted to make use of audio-only gadgets to entry these companies. Beneficiaries are required to have an in-person, non-telehealth service inside six months of their first telehealth psychological well being service (though the CAA of 2022 delayed this requirement for 151 days after the tip of the general public well being emergency).
What do Medicare beneficiaries pay for telehealth companies?
Beneficiary price sharing for telehealth companies has not modified throughout the public well being emergency. Medicare covers telehealth companies beneath Half B, so beneficiaries in conventional Medicare who use these advantages are topic to the Half B deductible of $233 in 2022 and 20% coinsurance. Nonetheless, the HHS Workplace of Inspector Common has supplied flexibility for suppliers to scale back or waive price sharing for telehealth visits throughout the COVID-19 public well being emergency, though there aren’t any publicly-available information to point the extent to which suppliers might have finished so. Most beneficiaries in conventional Medicare have supplemental insurance coverage which will pay some or the entire price sharing for coated telehealth companies. Medicare Benefit plans have flexibility to change cost-sharing necessities supplied they meet requirements of actuarial equivalence and different CMS necessities.
What applied sciences can be utilized for telehealth companies?
Through the COVID-19 public well being emergency, telehealth companies coated by Medicare will be performed through an interactive audio-video system, in addition to utilizing smartphones with real-time audio/video interactive capabilities with out different tools. Moreover, a restricted variety of telehealth companies will be supplied to sufferers through audio-only phone or a smartphone with out video (comparable to phone analysis and administration companies and behavioral well being counseling).
When the 151-day interval after the general public well being emergency ends, a telehealth go to have to be performed with two-way audio/video communications; using audio-only telephones won’t be permitted, aside from psychological well being companies (as described above).
What sort of suppliers can get reimbursed by Medicare for telehealth companies?
Through the public well being emergency, any well being care skilled who’s eligible to invoice Medicare for skilled companies can present and invoice for telehealth companies and doesn’t must have beforehand handled the beneficiary. Additionally, federally certified well being facilities and rural well being clinics are eligible for reimbursement for telehealth companies supplied to Medicare beneficiaries throughout the COVID-19 public well being emergency; these settings weren’t licensed as suppliers of telehealth companies for Medicare beneficiaries previous to statutory and regulatory adjustments made initially of the pandemic.
If no different statutory adjustments are made, as soon as the 151-day interval after the general public well being emergency ends, Medicare reimbursement for telehealth will revert to guidelines in place earlier than the general public well being emergency. Underneath these guidelines, solely physicians and sure different practitioners (comparable to doctor assistants, scientific social staff, and scientific psychologists) shall be eligible to obtain Medicare fee for telehealth companies supplied to eligible beneficiaries in conventional Medicare, and so they will need to have handled the beneficiary receiving the companies within the final three years.
How does Medicare pay suppliers for telehealth companies?
Through the public well being emergency, Medicare pays for telehealth companies, together with these delivered through audio-only phone, as in the event that they had been administered in particular person, with the fee fee various primarily based on the situation of the supplier, which signifies that Medicare pays extra for a telehealth service supplied by a health care provider in a non-facility setting, comparable to a clinician’s workplace, than by a health care provider in a facility setting, comparable to a hospital outpatient division. This additionally signifies that throughout the public well being emergency, medical doctors in non-facility settings are receiving a better fee for companies supplied by telehealth than they did earlier than the general public well being emergency.
Assuming no adjustments to present legislation, Medicare’s fee for a telehealth service after the 151-day interval after the general public well being emergency ends would be the identical no matter whether or not it was supplied in a non-facility setting or a facility setting, and the fee fee shall be primarily based on the decrease quantity paid to facility-based suppliers for a service delivered in particular person. (Underneath Medicare’s doctor charge schedule, the fee to facility-based-providers for in-person companies is decrease than the fee to non-facility suppliers as a result of Medicare makes a separate fee to services to cowl follow bills, comparable to bodily area, medical provides, medical tools, and scientific employees time.) The rationale for utilizing the decrease facility fee quantity for telehealth companies is that follow bills for the supply of telehealth companies needs to be decrease than these for an in-person go to.
How do Medicare Benefit plans cowl telehealth?
Medicare Benefit plans are required to cowl all Half A and Half B advantages coated beneath conventional Medicare. Moreover, since 2020, Medicare Benefit plans have been in a position to supply telehealth advantages not routinely coated by conventional Medicare (that’s, not throughout the COVID-19 public well being emergency), together with telehealth companies supplied to enrollees in their very own houses and companies supplied outdoors of rural areas. In 2022, nearly all Medicare Benefit plans (98%) supply a telehealth profit. Through the first 12 months of the COVID-19 pandemic, 49% of Medicare Benefit enrollees used telehealth companies.
Medicare Benefit plans are paid a capitated quantity by Medicare to offer fundamental Medicare advantages coated beneath Elements A and B, together with telehealth companies. Plans are actually permitted to incorporate prices related to extra telehealth advantages (past what conventional Medicare covers) of their bids for fundamental advantages.
Medicare Benefit plans have flexibility to waive sure necessities with regard to protection and value sharing in circumstances of catastrophe or emergency, such because the COVID-19 pandemic. CMS has suggested plans that they might waive or scale back price sharing for telehealth companies, so long as plans do that uniformly for all similarly-situated enrollees. Many Medicare Benefit plans have waived or decreased price sharing for enrollees for some or all companies administered through telehealth throughout the public well being emergency.
How is telehealth coated beneath Medicare for beneficiaries and suppliers taking part in different fee fashions?
Like all different conventional Medicare beneficiaries, beneficiaries who obtain care via an alternate fee mannequin can entry expanded telehealth advantages throughout the public well being emergency. Separate from the time-limited expanded availability of telehealth companies, CMS has granted suppliers taking part in some different funds fashions, together with Medicare Shared Financial savings Program ACOs, higher flexibility to offer care via telehealth, together with billing for telehealth companies supplied to each city and rural beneficiaries and to beneficiaries when they’re at dwelling.
Will Medicare’s protection of “digital test ins” expire on the finish of the general public well being emergency?
Separate from Medicare’s protection of telehealth companies, Medicare covers temporary, “digital check-ins” (additionally known as “temporary communication technology-based companies”) through phone or captured video picture, and E-visits for all beneficiaries, no matter whether or not they reside in a rural space. Each digital check-ins and E-visits, which had been obtainable to all beneficiaries previous to the general public well being emergency and can proceed to be obtainable to all beneficiaries after the general public well being emergency, are extra restricted in scope than a full telehealth go to. For instance, digital check-ins can solely be reported by suppliers with a longtime relationship to the affected person, can’t be associated to a latest medical go to (throughout the previous 7 days), and can’t result in a medical go to within the subsequent 24 hours (or the soonest obtainable appointment), and fee is meant to cowl solely 5-10 minutes of medical dialogue.
What are present legislative proposals to increase Medicare protection of telehealth?
Policymakers are contemplating quite a lot of proposals to increase some or the entire present flexibilities surrounding telehealth companies beneath Medicare past the general public well being emergency, and plenty of have expressed assist for doing so. Among the many telehealth-related payments which have been launched within the 117th Congress are proposals to increase sure Medicare telehealth companies and to completely carry geographic and site-based restrictions for Medicare protection of telehealth. Different laws would completely cowl a few of the telehealth expansions supplied throughout the public well being emergency and increase the scope of suppliers eligible for fee for telehealth companies coated by Medicare. Different payments are aimed toward assessing the impression of expanded telehealth companies in Medicare and Medicaid on utilization of telehealth visits, together with by demographics.
What coverage points are into account relating to the way forward for telehealth protection beneath Medicare?
Expanded protection of telehealth past the COVID-19 public well being emergency may have an effect on the standard of affected person care in addition to program and beneficiary spending. Broadening telehealth protection has the potential to enhance entry to wanted care, however the implications of telehealth for communities of shade will not be but clear, with analysis exhibiting each increased use in deprived neighborhoods and decrease use amongst black and rural Medicare beneficiaries than white beneficiaries. Furthermore, increasing telehealth protection would probably result in an general improve in Medicare program spending: CBO scored 5 months of expanded telehealth protection included within the CAA 2022 as costing $663 million. Nonetheless, some telehealth companies could also be substitutes for in-person care, comparable to a behavioral well being care go to, although simpler entry to telehealth may result in an general improve in visits and prices. Different telehealth companies might not absolutely exchange the necessity for (or prevalence of) an in-person go to, comparable to when lab work is set to be wanted.
Moreover, state licensing necessities may have an effect on entry to telehealth companies. Through the public well being emergency, states used emergency authority to waive elements of state licensing necessities for medical suppliers to make it simpler for folks to entry well being care through telehealth, and plenty of of those waivers are ending. Greater than half of states have signed the Interstate Medical Licensure Compact, which creates an expedited pathway for state licensure for medical suppliers, though it doesn’t present reciprocity for suppliers who’ve a state license in a single state and wish to follow in one other.
The potential growth of telehealth protection brings with it issues in regards to the potential for fraudulent exercise. There have been a number of giant fraud circumstances involving telehealth firms in recent times, most of which concerned the submission of fraudulent claims for objects, companies, and checks to Medicare and different insurers that had been by no means given or administered to sufferers. HHS’ Workplace of the Inspector Common (OIG) is conducting a number of research to evaluate the appropriateness of use of telehealth throughout the public well being emergency, together with an evaluation of supplier billing patterns to be able to establish suppliers that would pose a threat for program integrity and an audit of telehealth companies beneath Half B to guarantee that companies are assembly Medicare necessities. The Medicare Fee Advisory Fee (MedPAC) has advisable that Medicare apply extra scrutiny to outlier clinicians who ship extra telehealth companies than others, in addition to requiring in-person visits earlier than clinicians can order high-cost tools or companies for beneficiaries.