About 4 in ten adults (41%) in america—and about six in ten (57%) of these with family incomes beneath $40,000—have some degree of medical debt, owing an estimated $195 billion or extra in complete. Many adults who report medical debt cite prices related to emergency care (50%) and hospitalizations (35%) as sources of unpaid payments. Affording this care could also be particularly difficult for the massive variety of adults who’re uninsured or underinsured. The monetary affect of unpaid payments from hospitals and different suppliers on sufferers and their households may be substantial and lengthy lasting. Latest reporting signifies that hospitals are incomes wholesome margins in some areas the place a big share of residents are burdened with medical debt. In response to issues about medical debt and the affordability of care extra usually, policymakers have explored choices to strengthen the regulation of hospital charity care applications, which give free or discounted companies to eligible sufferers who’re unable to afford their care.
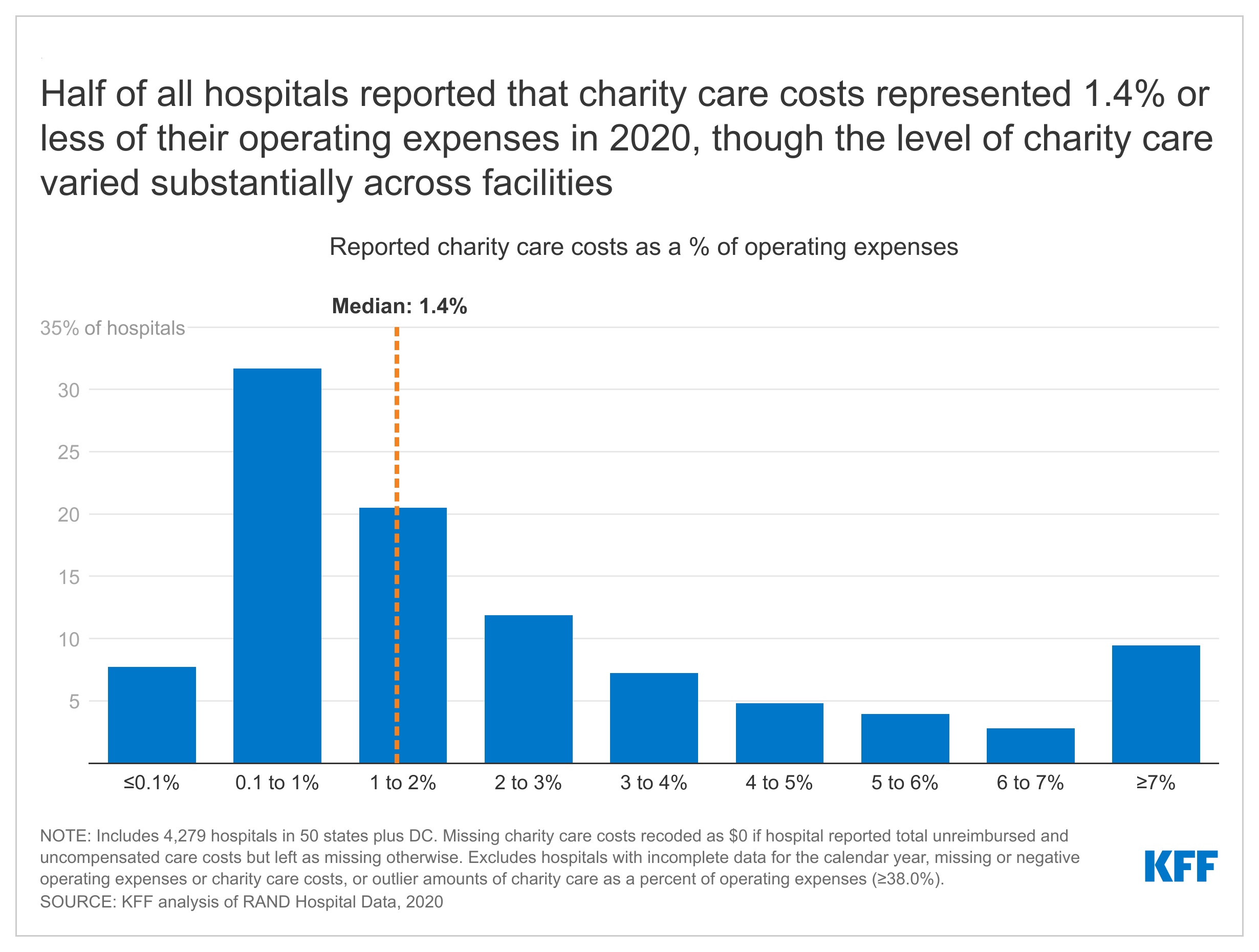
This problem temporary addresses key questions on hospital charity care applications. In keeping with our evaluation of hospital value experiences, charity care prices represented 1.4 % or much less of working bills at half of all hospitals in 2020, although the extent of charity care diversified considerably throughout services (Determine 1) (see Strategies for particulars about our calculations). For instance, whereas charity care prices represented 0.1 % of working bills or much less on the decrease finish of the spectrum (for 8% of hospitals), they represented 7.0 % of working bills or extra amongst an analogous share of hospitals (9%). The variation in charity care prices as a % of working bills possible displays variations in hospitals’ missions and enterprise practices; the necessity for charity care amongst sufferers; and federal, state, and native coverage and regulation. Federal, state, and native governments present funding in quite a lot of methods—together with by tax advantages for nonprofit hospitals—to assist hospital charity care, which can partially encourage efforts to extend the regulation of those applications. Though charity care applications are an essential supply of reduction for uninsured and underinsured sufferers, many People proceed to have issue affording hospital care. In 2022, about one in seven adults (14%) reported delaying hospital companies prior to now yr attributable to value.
What’s hospital charity care?
The Inside Income Service (IRS) defines “charity care”, also called “monetary help”, as “free or discounted well being companies supplied to individuals who meet the group’s eligibility standards for monetary help and are unable to pay for all or a portion of the companies.” Relying on their eligibility standards, hospitals might present charity care to each uninsured and insured sufferers. Amongst different authorities rules, federal regulation requires that nonprofit hospitals—which account for almost three-fifths (58%) of neighborhood hospitals—present some degree of charity care as a situation of receiving tax-exempt standing, and lots of state governments require all or a subset of hospitals to increase eligibility for charity care to sure teams of sufferers. Inside the broad parameters set by authorities regulation, hospitals set up their very own charity care insurance policies, which fluctuate when it comes to eligibility standards, utility procedures, and the degrees of charity care supplied. Whereas hospitals bear the direct prices of offering charity care, assist from donors and federal, state, and native governments might cowl some or all of those bills. Estimates from one latest examine recommend that the worth of the tax exemption alone coated about half (50%) of the price of charity care and different neighborhood advantages supplied by nonprofit hospitals from 2011 to 2018.
The sum of charity care and unhealthy debt is typically known as “uncompensated care”. “Dangerous debt” refers to situations the place a hospital payments a affected person however, after pursuing assortment, determines that it’s unlikely to gather cost. This stands in distinction to charity care, for which hospitals don’t search reimbursement. Hospitals accumulate unhealthy debt when sufferers are unable or unwilling to pay for his or her care. A few of these sufferers could also be eligible for charity care below the hospital’s charity care coverage however have no idea to use, have issue doing so, have their utility improperly denied, or select to not apply.
Who’s eligible for hospital charity care?
Hospitals have broad flexibility to determine their very own eligibility standards for charity care, and consequently, eligibility standards fluctuate throughout hospitals. For instance, one evaluation of a big pattern of nonprofit hospitals that used the federal poverty degree (FPL) to find out eligibility without cost care in 2018 discovered that about one in three (32%) of the hospitals required sufferers to have incomes at or beneath 200 % of the FPL ($50,200 for a household of 4 in that yr) or imposed extra restrictive eligibility standards, whereas the remaining hospitals (68%) relied on larger revenue caps. For discounted care, about three-fifths (62%) of nonprofit hospitals within the examine restricted eligibility to sufferers with incomes at or beneath 400 % of the FPL or used decrease revenue ranges, with the remaining nonprofit hospitals (38%) counting on larger revenue caps.
Hospitals might situation free or discounted care on different eligibility standards along with or in lieu of revenue thresholds primarily based on the FPL, equivalent to by requiring that sufferers have restricted property or reside within the hospital service space or by extending eligibility to sufferers who’re unable to afford giant medical payments regardless of exceeding revenue or asset thresholds below commonplace eligibility pathways. For instance, one evaluation of charity care insurance policies at 170 giant nonprofit and authorities hospitals discovered that the majority insurance policies (76%) recognized a streamlined utility course of for some teams which might be possible eligible for charity care, equivalent to sufferers experiencing homelessness.
It’s unclear what share of low-income sufferers are eligible for hospital charity care, not to mention what share of eligible sufferers find yourself benefiting from these applications, or what share of their prices are coated. Eligible sufferers might not obtain charity care as a result of they’re unaware that charity care is offered, have no idea that they’re eligible, have issue finishing an utility, are improperly denied charity care by the hospital, or select to not apply. Some proof means that many eligible sufferers might not be benefiting from charity care. For instance, nonprofit hospitals have estimated that, of the unhealthy debt that they reported in 2019 (reflecting bills in 2017 or an earlier yr), about $2.7 billion got here from sufferers who had been possible eligible for charity care however didn’t obtain it. This quantity is a tough estimate, because it comes from unaudited hospital experiences, is restricted to nonprofit services, and doesn’t account for situations the place eligible sufferers paid payments that may have been lowered below a given hospital’s charity care program.
How a lot charity care do hospitals present?
In keeping with the Medicaid and CHIP Cost and Entry Fee (MACPAC), hospitals reported $28 billion in charity care prices in fiscal yr (FY) 2019, the vast majority of which ($22 billion) was for uninsured people. Primarily based on our evaluation of hospital value experiences, charity care prices represented 1.4 % or much less of working bills at half of all hospitals in 2020, although the extent of charity care diversified considerably throughout services (Determine 1) (see Strategies for particulars about our calculations). For instance, whereas charity care prices represented 0.1 % of working bills or much less on the decrease finish of the spectrum (for 8% of hospitals), they represented 7.0 % of working bills or extra amongst an analogous share of hospitals (9%). Charity care prices as a % of working bills had been 2.6% in 2020 on common, which is bigger than the median given {that a} comparatively small share of hospitals reported comparatively giant quantities of charity care. Variation in charity care ranges throughout hospitals possible displays variations of their missions and enterprise practices; the necessity for charity care amongst sufferers; and federal, state, and native insurance policies and rules. The Medicare Cost Advisory Fee (MedPAC) has famous that the present methodology for calculating charity prices favors hospitals with larger markups, and it has really useful revisions that may put hospitals on extra equal footing and scale back reported charity care prices on common.
Latest analysis has discovered that for-profit hospitals dedicate an analogous share of their working bills to charity care as authorities hospitals on common and a bigger or related share as nonprofit hospitals. This will appear counterintuitive as a result of, in contrast to for-profit hospitals, nonprofit hospitals obtain giant tax-breaks that are, partially, meant to subsidize the charity care that they supply. Amongst potential explanations for this end result, for-profit hospitals might have a better willingness to offer charity care in some situations as a result of they will take a tax deduction for these bills, and it’s doable that some nonprofit hospitals might not anticipate important oversight of their charity care practices from authorities regulators.
What position does charity care play for undocumented and lawfully current immigrants?
Hospital charity care might play an essential position in defending undocumented and lawfully current immigrants from excessive medical prices on condition that they’re extra possible than residents to have low incomes and lack medical insurance. In 2020, about 4 in ten undocumented and lawfully current nonelderly immigrants (44% and 39%, respectively) had incomes beneath 200 % of the FPL in comparison with a few quarter (26%) of nonelderly residents. Moreover, about 4 in ten (42%) nonelderly undocumented immigrants and 1 / 4 (26%) of nonelderly lawfully current immigrants had been uninsured in comparison with lower than one in ten (8%) nonelderly residents. This disparity displays extra restricted entry to non-public protection and eligibility restrictions primarily based on immigration standing in medical insurance applications funded with public {dollars}. Regardless that charity care applications present monetary help for some immigrants, total, analysis means that immigrants use much less well being care, together with hospital care, than U.S.-born residents, and it stays unclear to what extent they profit from charity care applications and the way their use of those applications compares to that of residents.
What charity care guidelines should nonprofit hospitals adjust to in change for receiving federal tax-exempt standing?
Federal rules require that nonprofit hospitals present some degree of charity care and different neighborhood advantages as a situation of receiving tax-exempt standing. The IRS has outlined several types of neighborhood advantages, together with affected person advantages (equivalent to charity care), system advantages (equivalent to unreimbursed medical training), and neighborhood constructing actions (equivalent to addressing environmental hazards). In keeping with one examine, in 2017, unreimbursed Medicaid bills accounted for the plurality (44%) of nonprofit hospitals’ neighborhood profit bills, adopted by charity care (17%), unreimbursed well being professions training (15%), backed well being companies that aren’t mean-tested (10%), neighborhood well being enchancment companies and operations (4%), unfunded analysis (4%), money and in-kind contributions for neighborhood profit (3%), unreimbursed prices for means-tested applications apart from Medicaid (2%) and constructing actions (e.g., associated to housing) (1%). “Unreimbursed bills” for Medicaid—the nation’s public medical insurance program for folks with low incomes—and different means-tested applications refers back to the extent to which prices associated to sufferers enrolled in these applications exceed corresponding revenues for hospitals. Any unreimbursed bills from different payers are usually not counted in hospital neighborhood profit calculations.
To retain tax-exempt standing, nonprofit hospitals should:
- Set up a monetary help coverage (FAP). The FAP should describe who’s eligible for charity care, the extent of help supplied, and the way sufferers can apply. A hospital should make its FAP simply accessible to sufferers and be certain that the FAP is translated into the languages generally spoken locally served by the hospital.
- Cap prices to sufferers eligible for charity care primarily based on quantities usually billed to different payers. Federal regulation defines approaches for calculating the quantity usually billed primarily based on fee-for-service Medicare charges, Medicaid charges, and/or industrial plan cost charges.
- Conduct a neighborhood well being wants evaluation (CHNA) each three years and undertake an implementation technique to handle these wants. The CHNA should outline the neighborhood that the hospital serves and consider the well being wants of that neighborhood, integrating enter from native stakeholders. Neighborhood well being wants might embrace, for instance, reducing monetary limitations to well being care or enhancing social determinants of well being.
- Make cheap efforts to find out if a affected person is eligible for charity care earlier than partaking in sure debt assortment practices, together with promoting the affected person’s debt to 3rd events, reporting the debt to credit score companies, and taking authorized motion to manage a affected person’s monetary property. A “cheap effort” might entail, for instance, notifying the affected person of the FAP and giving them a minimum of 4 months to use following their first invoice after being discharged from the hospital.
Nevertheless, gaps in federal regulation and weak oversight and enforcement might permit hospitals to offer low ranges of charity care in some situations. Federal rules don’t at the moment outline or set minimal requirements for hospitals to find out who’s eligible for charity care or the extent of help to be supplied. A 2020 Authorities Accountability Workplace (GAO) report additionally raised questions on whether or not necessities to offer adequate neighborhood advantages, together with charity care, are being adequately enforced. In keeping with the report, the IRS had not revoked a hospital’s nonprofit standing on the idea of offering insufficient neighborhood advantages over the prior ten years.
Do states impose further charity care necessities for hospitals?
Barely over half of all states (26 states and DC) require all or a subset of hospitals to increase eligibility for charity care to sure teams of sufferers, based on a 2021 report from the Nationwide Client Legislation Middle. Amongst people who achieve this, 11 states (CA, CO, CT, IL, MD, ME, NJ, NV, NY, RI, and WA) broadly prolong minimal requirements to for-profit, nonprofit, and authorities hospitals alike. The 16 remaining state legal guidelines prolong to narrower teams of hospitals, together with nonprofit or authorities hospitals (3 states: LA, OR, and TX), hospitals that obtain sure sorts of authorities funding to offset the price of look after low-income sufferers (9 states: GA, KS, KY, MO, NM, OH, OK, PA, and TN), and hospitals in search of approval to increase or construct new well being care services (DC and three states: DE, NC, and VA). These state rules additionally fluctuate when it comes to eligibility standards and the extent of help that should be supplied. For instance, Nevada requires a subset of hospitals to offer free care to uninsured sufferers with particularly low incomes (38% or 39% of the FPL in 2022 relying on family measurement), whereas Maryland requires each acute and power care hospital to offer free care to each insured and uninsured sufferers at or beneath 200% of the FPL and to offer discounted care to sufferers with larger incomes.
Along with setting minimal requirements when it comes to eligibility, a number of states have applied rules meant to extend the uptake of charity care amongst eligible sufferers and to guard doubtlessly eligible sufferers from sure debt assortment practices. For instance, one evaluation discovered that 13 states require hospitals to display sufferers for eligibility, 16 states require hospitals to inform sufferers previous to accumulating cost and/or in each notification about collections, and eight states regulate procedures for sufferers to enchantment denials of charity care.
There’s little details about the effectiveness of those rules or the extent to which they’re enforced. One latest instance of a state enforcement exercise occurred in California, the place the Lawyer Normal despatched letters to hospitals alleging that they weren’t offering descriptions of their charity care insurance policies to sufferers within the sufferers’ spoken languages. One other latest instance occurred in Washington, the place the Lawyer Normal filed a lawsuit towards 14 hospitals for violating state charity care necessities, together with by sending many sufferers’ payments to collections when the hospitals knew the sufferers had been eligible for charity care.
What position do Medicaid, Medicare, and different authorities applications play in serving to hospitals afford charity care bills?
Medicaid offers well being protection for low-income sufferers and subsequently performs a major position in decreasing uncompensated care, together with by reducing the demand for hospital charity care. This was particularly evident in 2014, when many states adopted the Medicaid growth below the Reasonably priced Care Act (ACA) (and when enrollment within the ACA Marketplaces additionally started in all states). Amongst hospitals in states that expanded Medicaid, complete uncompensated care prices decreased from $16.7 billion in 2013 to $11.0 billion in 2014 (a 34% lower); in distinction, uncompensated care prices decreased by a a lot smaller quantity (from $18.1 billion in 2013 to $17.9 billion in 2014, a 1% lower) amongst hospitals in states that did increase Medicaid.
Medicaid and Medicare each present supplemental funds to hospitals which might be meant, a minimum of partially, to offset the prices of charity care and different uncompensated care:
- Medicare disproportionate share hospital (DSH) funds. Medicare offers further funds to hospitals that look after a disproportionate share of low-income sufferers, that are often known as “DSH hospitals”. The magnitude of Medicare DSH funds is predicated on hospitals’ Medicaid and Supplemental Safety Revenue (SSI) populations and the quantity of uncompensated care that they supply, amongst different elements. The Facilities for Medicare and Medicaid Providers (CMS) estimates that further Medicare funds to DSH hospitals will complete $14.0 billion in FY 2023.
- Medicaid DSH funds. State Medicaid applications additionally present further funds to DSH hospitals. Federal rules present states with a considerable degree of discretion when it comes to which services to designate as DSH hospitals and find out how to distribute funding. Medicaid DSH funds totaled $19.5 billion in FY 2020.
- Medicaid uncompensated care pool funds. In FY 2020, eight state Medicaid applications paid hospitals a complete of $8.2 billion to assist offset the prices of uncompensated care.
Different state and federal applications might present further assist to hospitals, which in flip can scale back the quantity of charity care hospitals have to soak up. For example, some state and native governments function applications past Medicaid that present protection to low-income sufferers or that offset uncompensated care prices. As one other instance, the 340B Drug Pricing Program offers substantial monetary assist primarily to hospitals that serve a lot of low-income sufferers. Beneath this program, the federal authorities requires drug producers to supply reductions on outpatient medicine to sure hospitals as a situation of getting their medicine coated by Medicaid. Gross sales of 340B medicine totaled an estimated $44 billion in 2021 and DSH hospitals account for the massive majority (78%) of gross sales. These further revenues assist services cowl their working bills, together with prices associated to the availability of charity care.
How has the availability of charity care modified in the course of the pandemic?
Though the COVID-19 pandemic has led to important and ongoing disruptions in hospital operations, hospital admissions bounced again after sharp preliminary declines, and huge quantities of presidency reduction have helped stabilized hospital funds and charity care spending. Most prominently, the federal Supplier Aid Fund (PRF) program has distributed $134 billion to hospitals and different suppliers as of early October 2022 to cowl well being care bills or misplaced revenues as a result of pandemic. Though the PRF program initially distributed funds on the idea of complete affected person income, which favored hospitals that obtained a big share of their revenues from personal insurance coverage, it later included $16 billion that was earmarked for safety-net hospitals. Amongst different reduction applications, the federal government additionally reimbursed suppliers, together with hospitals, for treating uninsured sufferers for COVID-19, with funds totaling $5.8 billion by the point this system stopped reimbursing claims in March 2022 attributable to lack of funding.
One examine discovered that common hospital working margins decreased from -1.0% in 2019 to -7.4% in 2020 when excluding COVID-19 reduction funds, however that complete margins—which take reduction funds into consideration—had been comparatively fixed over time and had been 6.7% in 2020. Equally, common charity care prices as a % of working bills remained comparatively fixed at 2.7% in 2019 and a pair of.6% in 2020 primarily based on our evaluation of hospital value experiences (see Strategies for particulars about our calculations). One evaluation of 151 giant nonprofit and authorities hospitals discovered that about three in ten (31%) expanded their charity care insurance policies from 2019 to 2021, whereas lower than one in ten (8%) moved in the direction of extra restrictive insurance policies; the remaining hospitals made minimal, indeterminate, or no change to their charity care insurance policies.
Some experiences recommend that the monetary outlook for hospitals has deteriorated in latest months, which can make it tougher for hospitals to take care of present ranges of charity care. Additional monitoring is required to evaluate the extent to which hospitals are experiencing monetary stress in response to ongoing results of the pandemic equivalent to labor shortages, decreases in authorities reduction, rising drug prices, and broader financial tendencies which have led to rising costs and funding losses.
Trying forward
Within the context of ongoing issues in regards to the affordability of hospital care and the rising burden of medical debt, a number of coverage concepts have been floated on the federal and state degree to strengthen hospital charity care applications. These embrace adjustments that may strengthen the necessities for nonprofit hospitals to qualify for tax-exempt standing, in addition to broader reforms that may apply to all hospitals. Particular proposals embrace creating or increasing necessities that hospitals present charity care to sufferers beneath a specified revenue threshold, mandating that nonprofit hospitals present a minimal quantity of neighborhood advantages, establishing a floor-and-trade system the place hospitals could be required to both present a minimal quantity of charity care or subsidize different hospitals that achieve this, introducing insurance policies to extend the uptake of charity care, increasing oversight and enforcement of neighborhood profit necessities, and restructuring the tax exemption for nonprofit hospitals to extra carefully tie authorities subsidies to the worth of charity care and different neighborhood advantages supplied by a given facility. A associated set of proposals are meant to higher align neighborhood advantages with native or regional wants and will subsequently additionally have an effect on the availability of charity care.
Latest coverage adjustments have been concentrated on the state degree. For instance, since 2021, California and Washington state have expanded their charity care mandates to cowl extra sufferers by larger revenue eligibility thresholds. Colorado has launched a non-public proper of motion to implement hospital compliance with charity care necessities, and Illinois has applied new reporting necessities for charity care applications. State and federal policymakers have additionally thought of a number of different choices to scale back medical debt or enhance affordability extra usually, equivalent to by increasing Medicaid in states that haven’t already finished so, decreasing well being care costs by direct regulation or different means, and growing shopper protections towards medical debt.
Efforts to increase hospital charity care will inevitably contain tradeoffs, together with the potential value to hospitals from defending sufferers who can not afford their hospital payments.
| Our evaluation of reported charity care prices as a % of working bills is predicated on 2019-2020 RAND Hospital Knowledge, which is a cleaned and processed model of annual value report information submitted by hospitals to the Healthcare Price Report Info System (HCRIS). Each Medicare-certified hospital should submit a value report, which means that HCRIS information embody all US hospitals besides federal hospitals and a few youngsters’s hospitals. HCRIS directions point out that hospitals ought to report quantities associated to each their charity care and uninsured reductions as a part of their charity care prices. The Medicare Cost Advisory Fee (MedPAC) has famous that present HCRIS calculations favor hospitals with larger markups, and it has really useful revisions that may put hospitals on extra equal footing and scale back reported charity care prices on common.
Our evaluation relied on a calendar yr model of the RAND Hospital Knowledge, which apportions information from completely different value experiences for hospitals that don’t use a calendar yr reporting interval. We targeted on short-term normal hospitals in all 50 states plus DC. We recoded lacking charity care prices as $0 if the hospital reported complete unreimbursed and uncompensated care prices (affecting about 3% of hospitals) however left as lacking in any other case. There have been no different situations of $0 charity care prices in our pattern. We excluded hospitals with incomplete information for the calendar yr, lacking or damaging working bills or charity care prices, or outlier quantities of charity care as a % of working bills (better than or equal to 38.0%, i.e., the highest 0.1% of hospitals). Our closing pattern for 2020 included 4,279 of the 4,546 short-term normal hospitals within the 2020 RAND Hospital Knowledge. When evaluating charity care prices in 2019 and 2020, we restricted the pattern to the 4,236 hospitals that had been in pattern in each years. We evaluated two changes to our evaluation and located that neither considerably affected our major findings. First, we discovered that dropping all hospitals with lacking charity care prices, slightly than recoding a subset as $0, would lead to an analogous median worth for charity care prices as a % of working bills (1.5% versus 1.4%) and the identical imply worth (2.6%), with considerably much less variation throughout hospitals than in our evaluation. For instance, below this different method, charity care prices would symbolize 0.2 % of working bills or much less amongst eleven % of hospitals and seven.0 % of working prices or extra amongst 9 % of hospitals. Second, as with our evaluation evaluating 2019 and 2020, when additional limiting the pattern to the 1,628 hospitals that used a calendar yr reporting interval in each years, common charity care prices as a % of working bills remained comparatively fixed over time (at 2.3% in 2019 and a pair of.2% in 2020). |