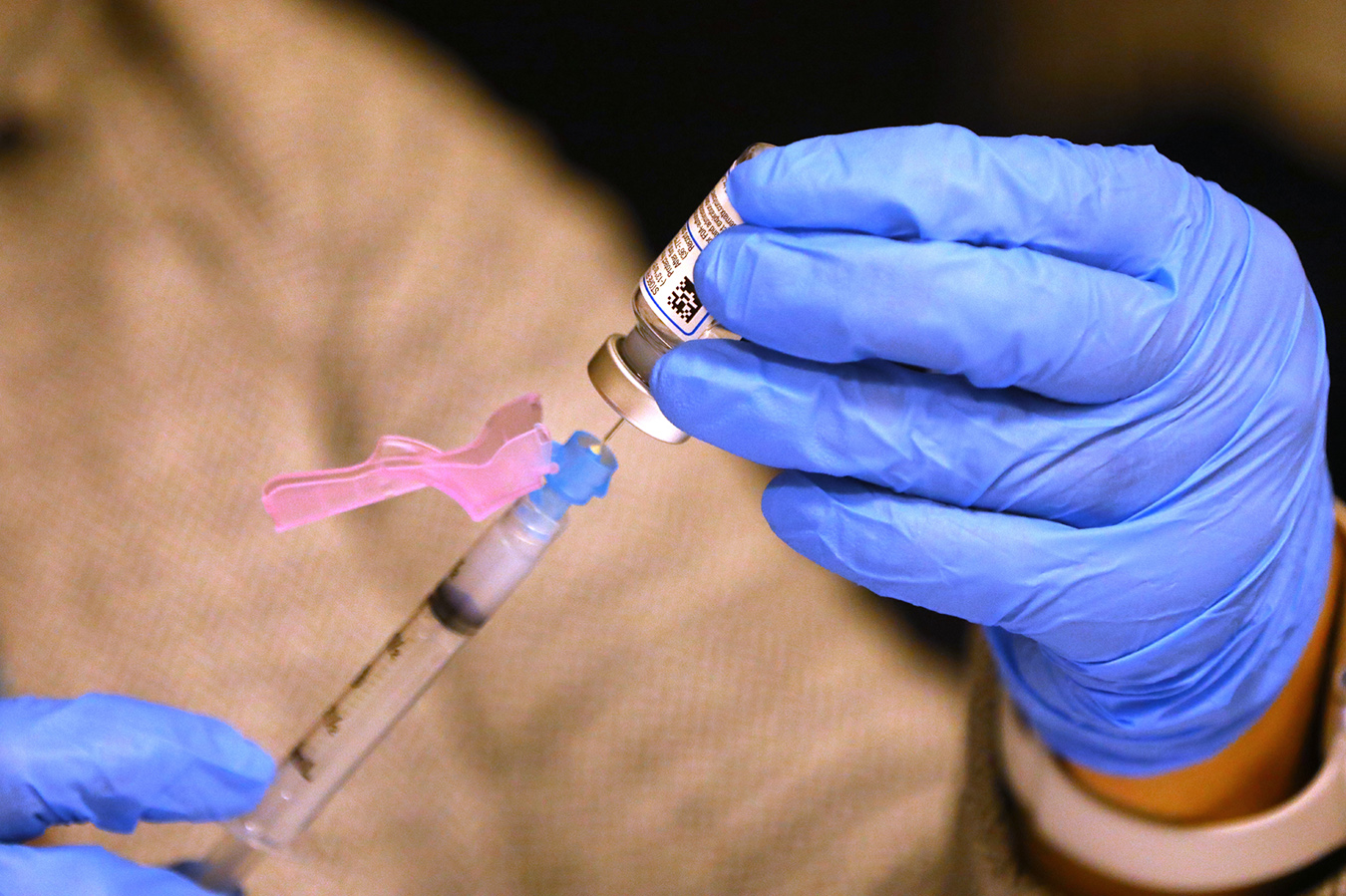
Final week, after ending inoculations of some front-line hospital employees, Jupiter Medical Middle was left with 40 doses of treasured covid vaccine. So, officers provided photographs to the South Florida hospital’s board of administrators and their spouses over age 65.
However that call sparked outrage amongst staff left unvaccinated, together with these at one of many hospital’s pressing care clinics, or who imagine the hospital was currying favor with rich insiders earlier than getting all its staffers protected, in response to a hospital worker who spoke on the situation of not being named.
The transfer additionally prompted dozens of calls from donors trying to get vaccinated.
The hospital obtained 1,000 doses of the Moderna vaccine two days earlier than Christmas, fewer than half of what it requested from the state to cowl its workforce. Officers prioritized delivering the vaccine to front-line medical staff who requested it, performing inoculations on Christmas Eve or the vacation weekends.
Patti Patrick, a hospital vice chairman, stated the hospital acted appropriately in its choices of the vaccine, which has a brief shelf life as soon as vials are opened. Neither she nor different directors who don’t work immediately with sufferers had been included on this first spherical of photographs.
“This was a easy technique to transfer 40 doses in a short time” earlier than it spoiled, she stated.
She added that each one front-line employees from the well being system, together with the clinics, got the chance to get the photographs.
Jupiter shouldn’t be the one hospital within the nation going through questions on its dealing with of the vaccines. The preliminary rollout — aimed toward well being care staff and nursing residence residents — has been uneven at greatest due to a scarcity of a federal technique on the way it ought to work, with states, hospitals, nursing properties and pharmacies typically making selections on their very own about who will get vaccinated and when.
In some hospitals, directors and different personnel who don’t have any contact with sufferers or face no threat at work from the virus are getting photographs, whereas sufferers — and even front-line employees — who’re at heightened threat for covid problems are being handed by. Some directors who’ve been working remotely all through the pandemic have been vaccinated, particularly at hospitals that determined to allocate doses by age group quite than publicity threat.
Though states and federal well being teams laid out broad tips on tips on how to prioritize who will get the vaccine, in apply what’s mattered most was who managed the vaccine and the place the vaccine distribution was dealt with.
Stanford Well being Care in California was pressured to transform its precedence listing after protests from front-line medical doctors in coaching who stated that they had been unfairly neglected whereas the vaccine was given to college who don’t recurrently see sufferers. (Age was the necessary issue within the college’s algorithm.)
Members of Congress have known as for an investigation following media studies that MorseLife Well being System, a nonprofit that operates a nursing residence and assisted residing facility in West Palm Seaside, Florida, vaccinated donors and members of a rustic membership who donated hundreds of {dollars} to the well being firm.
At the least three different South Florida hospital methods — Jackson Well being, Mount Sinai Medical Middle and Baptist Well being — have provided vaccines to donors upfront of most people, whereas administering the photographs to front-line staff, The Miami Herald reported.
Like Jupiter Medical, the hospitals insist that these provided photographs had been 65 and older, as prioritized by state officers.
Staffing Issues at Hospitals
An advisory board to the Facilities for Illness Management and Prevention designated hospitals and nursing properties to get covid vaccines first as a result of their staff and residents had been thought-about at highest threat, and most states have adopted that advice. However in lots of instances, the well being establishments have discovered demand from staffers, a few of whom are leery of the voluntary shot, is lower than anticipated.
As well as, the arrival of promised shipments has been unpredictable. Whereas the federal authorities authorized the primary covid vaccine on Dec. 14, some hospitals didn’t obtain allotments till after Christmas.
That was the case at Hendry Regional Medical Middle in Clewiston, Florida, which obtained 300 doses from the state. The hospital vaccinated 30 of its 285 staff between Dec. 28 and Jan. 5, stated R.D. Williams, its chief government officer. Some staff most well-liked to attend till after New 12 months’s weekend out of concern about unintended effects, he stated.
The vaccine has been reported to generally trigger ache on the injection website and typically produce fever, lethargy or headache. The reactions usually final no various days.
“I’m pleased with the way it’s going to this point,” Williams stated. “I do know lots of our staff need to be vaccinated, however I don’t see it as a panacea that they need to have it as we speak,” he stated, noting that staffers have already got masks and gloves to guard themselves from the virus.
The hospital can also be attempting to coordinate vaccination schedules so 10 individuals at a time get the shot to make sure not one of the treatment is wasted after the multidose vials are thawed. As soon as vaccine is thawed, it have to be used inside hours to retain its effectiveness.
As of Jan. 6, Howard College Hospital in Washington, D.C., had vaccinated barely greater than 900 well being staff since its first doses arrived Dec. 14. It has obtained 3,000 doses.
Success has been restricted by reluctance amongst staff to get a vaccine and a scarcity of personnel educated to manage it, CEO Anita Jenkins stated.
“We nonetheless have a hospital to run and have sufferers within the hospital with coronary heart assaults and different situations, and we don’t have extra employees to run the vaccine clinics,” she stated.
Whereas some hospitals provide the vaccine solely to front-line staff who work together with sufferers, Howard makes it accessible to everybody, together with public relations employees, cafeteria staff and directors. Jenkins defended the transfer as a result of, she stated, it’s one of the best ways to guard the whole hospital.
She famous such staff as info expertise personnel who don’t see sufferers could also be round medical doctors and nurses who do. “Working in a hospital, virtually everybody runs into sufferers simply strolling down the hallway,” she stated.
At Eisenhower Well being, a nonprofit hospital primarily based in Rancho Mirage, California, 2,300 of the 5,000 staff have been vaccinated.
“Our best problem has been managing the present affected person surge and staffing calls for in our acute and demanding care areas whereas additionally attempting to make sure we have now ample staffing assets to function the vaccine clinics,” stated spokesperson Lee Rice.
A Non-System of Inequitable Distribution
Arthur Caplan, a bioethicist at NYU Langone Medical Middle in New York Metropolis, stated hospitals shouldn’t be inoculating board members forward of hospital staff except these individuals have an important position in operating the hospital.
“That appears, to me, jostling to the pinnacle of the road and attempting to reward those that could also be potential donors,” he stated. However he acknowledged that the hospitals’ vaccination methods should not at all times rational or equitable.
Covid vaccines must get out as rapidly as doable, he added, however hospitals can provide them solely to individuals they’re linked with.
Caplan famous he was vaccinated at an NYU outpatient website final week, regardless that his main care physician hadn’t but gotten the vaccine as a result of his clinic had not obtained any doses.