Concerning the Survey
On March 18, 2020, in response to the outbreak of COVID-19 in america, the Households First Coronavirus Response Act (FFCRA) was signed into regulation. The FFCRA included a provision requiring state Medicaid packages to maintain individuals enrolled, in alternate for extra federal funding. This steady enrollment provision lasted for 3 years, ending on March 31, 2023, and states had been in a position to resume disenrolling individuals from Medicaid who now not met eligibility necessities or who didn’t full the renewal course of starting on April 1, 2023. This strategy of conducting redeterminations for all Medicaid enrollees has been generally known as “Medicaid unwinding.”
For the reason that begin of Medicaid unwinding, KFF state monitoring exhibits that greater than 20 million individuals have been disenrolled from Medicaid, with states reporting renewal outcomes for two-thirds of enrollees thus far. To make clear the experiences of people that tried to resume their protection or discover a completely different supply of well being protection throughout this era, KFF interviewed 1,227 U.S. adults who had Medicaid protection in previous to April 1, 2023 – as states started the method of figuring out who was nonetheless eligible for Medicaid of their state. This report highlights individuals’s experiences with the Medicaid unwinding course of and measures the monetary and well being impacts of being disenrolled from Medicaid and/or having to seek out different types of protection. Whereas the dimensions of the unwinding is unprecedented, the survey findings may also help policymakers perceive how one can enhance the Medicaid renewal course of extra typically going ahead.
Key Takeaways
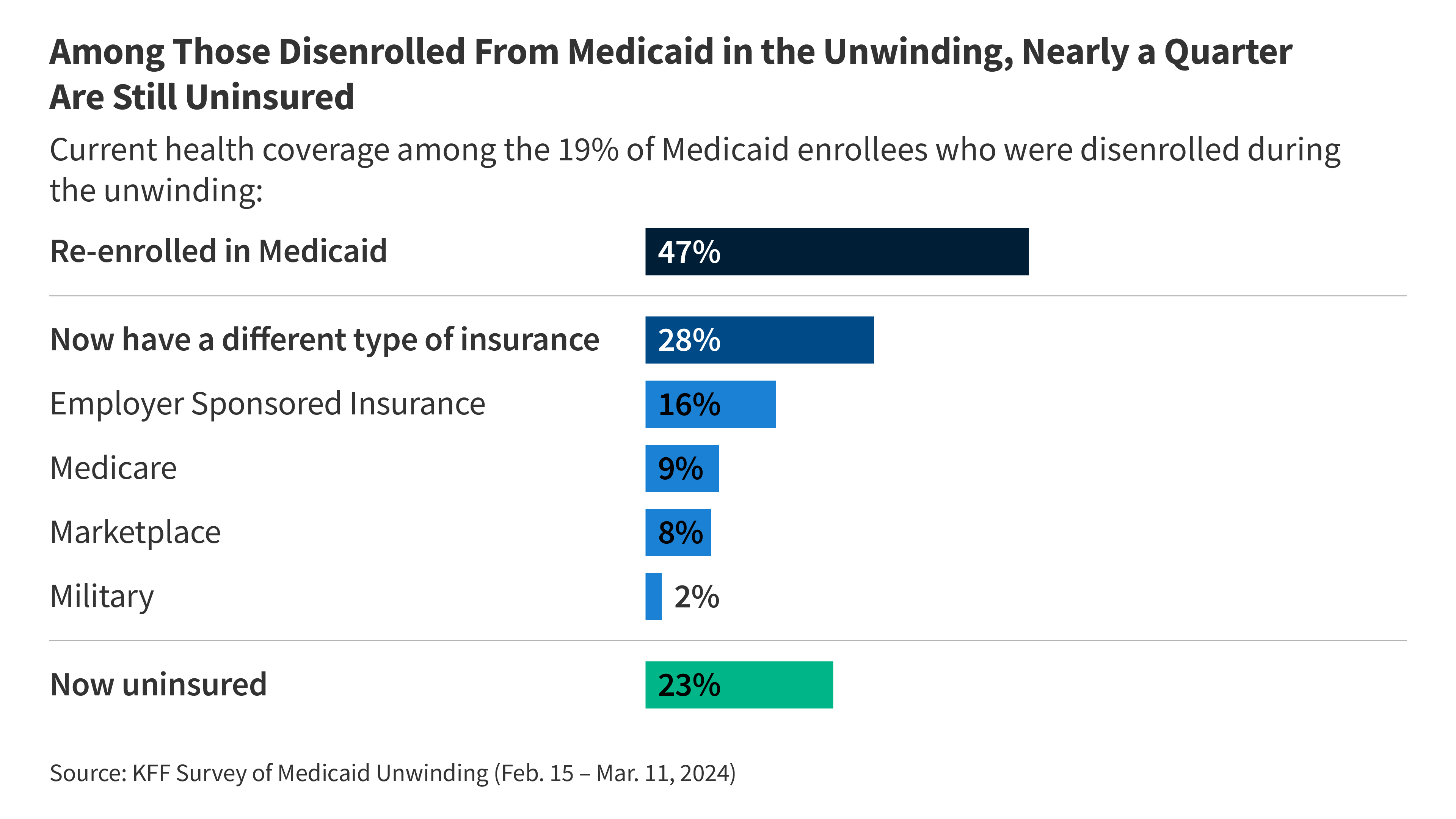
- About one in 5 enrollees say they had been disenrolled from Medicaid protection sooner or later in 2023 and a couple of quarter (23%) of those that had been disenrolled stay uninsured. A few of those that had been disenrolled finally re-enrolled in this system (47%) or discovered different types of well being protection (28%), however the lack of protection led many to fret about each their bodily well being and their psychological well being. Three-fourths of those that had been disenrolled from Medicaid say they had been apprehensive about their bodily well being whereas six in ten say they had been apprehensive about their psychological well being. Moreover, a majority (56%) say they skipped or delayed getting well being care providers or prescriptions whereas trying to resume their protection (13% of whole enrollees).
- Newly uninsured adults cite prices as the explanation for not getting one other type of well being protection. Most pre-unwinding enrollees say they both retained their protection or had been in a position to re-enroll in Medicaid (83%), however one in twelve (8%) of all enrollees are actually uninsured, leading to tens of millions of newly uninsured people. Greater than a 3rd (36%) of the at present uninsured group say they’re nonetheless making an attempt to get Medicaid protection, and greater than half (54%) cite prices as the explanation why they haven’t gotten protection from elsewhere.
- Medical health insurance prices are additionally a significant concern for many who now have a distinct type of protection. Amongst those that now produce other types of protection (8% of enrollees), half (50%) say they fear about affording their month-to-month premium, and three-quarters (76%) say they’re apprehensive about affording the prices of well being care providers. Most who’ve one other supply of protection say it’s about the identical as or higher than Medicaid when it comes to entry to care.
- Many pre-unwinding enrollees who tried to resume their Medicaid protection encountered some sort of drawback. Two-thirds (64%) of these enrolled in Medicaid earlier than the unwinding course of started say they took motion final 12 months to resume their protection. Amongst those that tried to re-enroll, most discovered it very or considerably straightforward, however 58% (37% of whole enrollees) skilled no less than one drawback in the course of the course of, mostly lengthy name heart wait occasions (44%). Different issues encountered embody not understanding what paperwork had been wanted; making an attempt to submit paperwork and being instructed they had been incomplete, not acquired, or not processed; or having unreliable web entry to finish kinds on-line. Notably, about half (54%) of those that skilled any drawback when making an attempt to resume their protection say they discovered it troublesome to resume their Medicaid protection.
- These dwelling in states that haven’t expanded Medicaid usually tend to say they wanted proof of residency to resume their protection. Enrollees dwelling in non-expansion states had been no less than twenty share factors extra doubtless than these in Medicaid growth states to say they had been requested to submit proof of residency. Whereas states are required to first examine accessible knowledge sources to substantiate ongoing eligibility, they might require enrollees to submit sure paperwork at renewal if the state can not acquire the knowledge electronically.
Medicaid Enlargement States
The Reasonably priced Care Act’s (ACA) Medicaid growth expanded Medicaid protection to almost all adults with incomes as much as 138% of the Federal Poverty Degree ($20,783 for a person in 2024, or $35,632 for a household of three) and gives states with an enhanced federal matching charge (FMAP) of 90% for his or her growth populations. Nevertheless, the growth is successfully non-compulsory for states due to a 2012 Supreme Courtroom ruling. So far, 41 states (together with DC) have adopted the Medicaid growth and 10 states haven’t adopted the growth (Alabama, Florida, Georgia, Kansas, Mississippi, South Carolina, Tennessee, Texas, Wisconsin and Wyoming). In these states, the median earnings restrict for folks is simply 38% FPL, or an annual earnings of $9,812 for a household of three in 2024. In practically all states that haven’t adopted the ACA growth, childless adults stay ineligible no matter their earnings. In Texas, the state with the bottom eligibility threshold, dad and mom in a household of three with incomes above $4,131 yearly, or simply $344 per 30 days, usually are not eligible for Medicaid. Mother and father who certified for Medicaid throughout steady enrollment might fall into the protection hole if their earnings is now too excessive to qualify for Medicaid however too low (under the federal poverty stage, or $25,820 for a household of three) to qualify for sponsored protection within the Market.
Half of Pre-Unwinding Enrollees Say They Heard Little or Nothing Concerning the Medicaid Unwinding Course of
A current KFF Well being Monitoring Ballot discovered that about seven in ten of the general public (69%) say they’ve heard solely “a little bit” or “nothing in any respect” about states eradicating individuals from Medicaid as pandemic insurance policies got here to an finish. The KFF Survey of Medicaid Unwinding finds that amongst adults who had been enrolled in Medicaid previous to the beginning of the unwinding course of, about half (53%) say they heard “a little bit” or “nothing in any respect” about states eradicating individuals from Medicaid as pandemic insurance policies got here to an finish. This contains three in ten (31%) who say they heard “nothing in any respect” about states eradicating individuals from Medicaid final 12 months. One in six (17%) enrollees say they heard “lots” about Medicaid unwinding and three in ten (30%) say they heard “some.”
These with decrease ranges of academic attainment, particularly these with a highschool diploma or much less, had been more likely to say they heard “nothing in any respect” about states eradicating individuals from Medicaid. Moreover, enrollees dwelling in non-expansion states had been extra prone to say they’ve heard “lots” or “some” about Medicaid unwinding (59%), in comparison with 45% of these dwelling in growth states.
For a Sizeable Share of Pre-Unwinding Enrollees, the Medicaid Re-Enrollment Course of Proved Troublesome
After a three-year pause in disenrolling people from the Medicaid program, on April 1, 2023, states resumed disenrolling those that had been now not eligible or who didn’t full the renewal course of. As a part of that course of, states ship notices to enrollees indicating whether or not the enrollee must take motion to resume their Medicaid protection. Amongst adults who had been enrolled in Medicaid previous to the beginning of the unwinding course of, seven in ten (71%) say they bear in mind receiving details about renewing, confirming, or re-enrolling in Medicaid whereas about three in ten (29%) say they don’t bear in mind receiving renewal data.
Much like general consciousness of the Medicaid unwinding course of, these with a highschool diploma or much less (67%) are much less doubtless than enrollees with no less than some faculty schooling (76%) and faculty graduates (80%) to say they bear in mind receiving discover about renewing their Medicaid protection. One-third (33%) of enrollees with a highschool diploma or much less say they don’t bear in mind receiving any details about renewing, confirming, or re-enrolling in Medicaid.
Much like general consciousness, enrollees dwelling in non-expansion states had been typically much less doubtless than these dwelling in growth states to recollect receiving discover about renewing their Medicaid protection (61% vs. 74%).
The commonest approach individuals bear in mind receiving data was by means of the U.S. mail. About six in ten (63%) Medicaid enrollees say they acquired discover through mail relating to Medicaid renewal whereas about one in 5 (22%) say they acquired renewal data through e mail. One in ten pre-unwinding enrollees say they acquired discover through a web based Medicaid portal (10%) or through textual content message (10%). Final 12 months’s KFF Survey of Client Experiences with Well being Insurance coverage reported that the mail was the popular methodology of contact for Medicaid enrollees about renewing their protection.
The Medicaid renewal course of varies barely amongst states however step one is for states to try to confirm a person’s eligibility by checking accessible knowledge sources. If the state can affirm eligibility utilizing these knowledge sources, the person’s protection can be renewed, and the person doesn’t must take any motion. Nevertheless, if eligibility can’t be confirmed utilizing knowledge sources, the state should ship a renewal type to the person.
As a result of not everybody must take motion to resume their Medicaid protection, not each Medicaid enrollee may have expertise with making an attempt to resume their protection. The KFF Survey of Medicaid Unwinding contains about two-thirds (64%) of adults who had been enrolled in Medicaid previous to the beginning of the unwinding course of and say they took motion final 12 months to attempt to renew their Medicaid protection.
Notably, those that acquired discover about the necessity to re-enroll seem to have been spurred to motion as greater than three in 4 (78%) of those that bear in mind receiving details about confirming, renewing, or re-enrolling in Medicaid say they took motion to attempt to renew their protection. In distinction, simply three in ten (29%) of those that didn’t recall receiving data say they took motion to resume their Medicaid protection.
Most of those that took some sort of motion to resume their protection discovered the method straightforward. About two-thirds (65%) of enrollees who tried to resume their protection say they discovered the Medicaid renewal course of to be “very straightforward” or “considerably straightforward.” Nonetheless, about one-third (35%) of enrollees who tried to resume their protection discovered the method troublesome. Extra particularly, about three in ten say gathering and submitting the paperwork (29%) and determining what paperwork had been wanted to finish enrollment (28%) had been both “very troublesome” or “considerably troublesome.” Moreover, about one in 4 (23%) enrollees who tried to resume their protection say filling out the mandatory kinds was no less than considerably troublesome.
Enrollees are break up on whether or not they discovered the expertise annoying or not. General, half (48%) of those that took motion to attempt to renew their protection say they discovered the method to be no less than considerably annoying, much like the share (52%) who say it was “not too annoying” or “in no way annoying.”
Those that have beforehand renewed their Medicaid are extra doubtless than these for whom it is a new expertise to say they bear in mind receiving details about re-enrolling in Medicaid (79% vs. 57%) and to say they took motion to resume their Medicaid protection (75% vs 42%). Nevertheless, prior expertise with the renewal course of doesn’t essentially translate to a better or much less annoying expertise making an attempt to resume their protection.
A few third of each teams, those that had beforehand participated in renewal and those that had not, say the renewal course of throughout unwinding was troublesome (35% vs. 33% respectively) and about half of each teams say the method was annoying (48% and 49% respectively).
A Majority of Pre-Unwinding Enrollees Who Tried To Renew Their Medicaid Protection Skilled Issues
About six in ten (58%) adults who had been enrolled in Medicaid previous to unwinding and tried to resume their protection final 12 months say they skilled no less than one drawback when doing so (37% of whole enrollees). Essentially the most generally reported drawback was lengthy wait occasions on the cellphone (44%), adopted by not understanding what paperwork had been wanted to finish re-enrollment (26%), making an attempt to submit kinds however being instructed the paperwork had been incomplete (25%), and submitting renewal supplies or kinds however being instructed that they weren’t acquired or not processed (24%). Moreover, 14% of pre-unwinding enrollees who tried to resume their Medicaid protection stated they didn’t have dependable web entry to finish kinds on-line, rising to 19% amongst these with family incomes below $20,000, to 19% amongst rural residents, and to 23% amongst those that say they’re in truthful or poor bodily well being.
Enrollees who say they skilled an issue when making an attempt to resume their protection usually tend to say the renewal course of was troublesome with a slight majority saying the method was “very” (11%) or “considerably” (42%) troublesome. Moreover, two-thirds (66%) of those that skilled an issue when making an attempt to resume their protection discovered the method to be no less than considerably annoying.
Amongst enrollees who tried to resume their protection, 28% say they received assist with the Medicaid renewal course of, together with a couple of third of enrollees who’re in truthful or poor well being (34%). The commonest supply of assist was from a Medicaid case employee or Navigator (19%), whereas fewer say they acquired assist from a pal or member of the family (7%), from a Medicaid well being plan (5%), or from a health care provider or well being care supplier (3%).
Moreover, about one in six (17%) of those that didn’t get assist say they wished help (8% of whole enrollees). This was mostly reported by pre-unwinding enrollees who skilled issues when making an attempt to resume their protection. About three in ten (29%) pre-unwinding enrollees who skilled issues when making an attempt to resume their protection say they wished however didn’t get assist with the method.
These in Non-Enlargement States Are Extra Doubtless To Report Being Requested To Submit Proof of State Residency When Trying To Renew Medicaid Protection
As a part of the method to redetermine Medicaid eligibility, states might require individuals to submit varied varieties of data. General, about three in 4 (77%) enrollees who tried to resume their Medicaid protection say they had been requested to submit proof of earnings or monetary property as a part of the renewal course of and about half (54%) say they had been requested to submit proof of residency of their state.
Pre-unwinding enrollees in non-expansion states are more likely than these in growth states to say they had been requested to submit proof of residency of their state (73% vs. 51%). States are required to first examine accessible knowledge sources to substantiate ongoing eligibility. Nevertheless, if they’re unable to acquire data through digital sources, they might require enrollees to submit documentation confirming earnings or residency. States may settle for self-attestation of sure data.
General, Black and Hispanic adults are more likely than White adults to say they had been requested to submit proof of residency of their state as a part of the Medicaid renewal course of. Majorities of Black (71%) and Hispanic (60%) enrollees say they had been requested to submit proof of state residency, in comparison with fewer White enrollees (42%) who say the identical.
One in 5 Pre-Unwinding Enrollees Say They Had been Disenrolled from Medicaid at Some Level For the reason that Starting of the Unwinding Course of
One in 5 (19%) pre-unwinding enrollees say they misplaced their Medicaid protection sooner or later since April 1, 2023 – at the same time as some have efficiently re-enrolled in this system. Being disenrolled was extra widespread amongst youthful enrollees (below the age of fifty), and never surprisingly, amongst those that skilled issues in the course of the renewal course of. In Medicaid growth states, 13% enrollees with a family earnings below $20,000 – most of whom are doubtless nonetheless eligible for Medicaid protection – say they had been disenrolled sooner or later for the reason that begin of unwinding.
Notably, three in ten (30%) pre-unwinding enrollees say they discovered they had been disenrolled once they had been knowledgeable by a health care provider, medical supplier, or pharmacist.
Data of Re-enrollment
Not like most employer-sponsored insurance policy and self-purchased ACA Market plans which have particular open enrollment intervals for customers to sign-up for protection, Medicaid permits enrollment all year long. Whereas a majority of pre-unwinding enrollees are conscious that in the event that they lose Medicaid protection they will re-enroll at any time of the 12 months (63%), a 3rd incorrectly suppose they will solely re-enroll throughout particular time intervals (35%). Amongst those that had been disenrolled in the course of the unwinding course of, six in ten (58%) are conscious that they will re-enroll at any time in the course of the 12 months whereas 4 in ten (40%) suppose you possibly can solely re-enroll throughout particular time intervals.
Disenrollment Led to Elevated Well being Worries, Skipped Care
Whether or not or not they had been in a position to re-enroll in Medicaid, disenrollment from Medicaid had a disruptive impact on those that skilled it. Seven in ten (70%) adults who had been disenrolled from Medicaid in the course of the unwinding course of say that they turned uninsured once they misplaced their Medicaid protection, whereas three in ten say they already had one other type of well being protection in place.
Shedding Medicaid protection led to worries about their very own well being. Three in 4 (75%) of those that turned uninsured say that they had been no less than considerably apprehensive about their bodily well being and 6 in ten (60%) say they had been apprehensive about their psychological well being once they misplaced their Medicaid protection. This contains about 4 in ten who say they had been “very apprehensive” about their bodily well being (43%) or their psychological well being (37%).
As well as, about one in 5 (21%) enrollees who took motion to resume their Medicaid protection (13% of whole enrollees) say they skipped or delayed getting wanted well being care providers or prescription drugs when trying to resume their protection. The share who say they skipped or delayed wanted well being care when trying to resume their protection will increase to greater than half (56%) of those that say they misplaced their Medicaid protection sooner or later for the reason that begin of unwinding.
A Quarter of These Who Had been Disenrolled Are Now Uninsured, Prices High Issues of These Who No Longer Have Medicaid Protection
Because the Medicaid unwinding course of continues, about half (47%) of those that had been disenrolled from Medicaid final 12 months are actually at present enrolled in Medicaid protection. Previous to the pandemic, about 41% of Medicaid enrollees who had been disenrolled finally re-enrolled in protection. Greater than 1 / 4 of those that had been disenrolled are actually insured with a distinct type of protection together with 16% who’ve employer-sponsored insurance coverage, 9% who’ve Medicare, and eight% who’ve bought their very own insurance coverage by means of the ACA market. One in 4 (23%) of those that had been disenrolled are at present uninsured.
General, a big majority (83%) of enrollees say they at present have Medicaid protection whereas 8% say they’re now uninsured, and eight% say they now not have Medicaid protection, however have another sort of medical health insurance, together with 4% who say they’re now lined by employer-sponsored insurance coverage, 2% who say they’re now lined by Medicare, and a couple of% who are actually lined by a self-purchased Market plan.
About one in eight Hispanic adults (13%), and one in ten ladies (10%) and enrollees between the ages of 18 and 49 (10%) say they’re now uninsured. The share of pre-unwinding enrollees who are actually uninsured will increase to 17% amongst these dwelling in non-expansion states. In growth states, 6% of pre-unwinding enrollees with family incomes of lower than $20,000 – a gaggle that ought to largely nonetheless be eligible for Medicaid – say they’re at present uninsured.
These With Different Types of Protection Charge Their Present Protection Worse Than Medicaid on Out-of-Pocket Prices, Although Many Say New Protection Is the Similar or Higher When It Involves Entry
Most enrollees who now have one other type of well being protection say their present insurance coverage is “about the identical” or in some instances, “higher” than Medicaid in relation to well being care entry. For instance, most charge their present protection about the identical (58%) as Medicaid in relation to the flexibility see a health care provider or well being care supplier when they should, whereas one in 5 (20%) say their present protection is healthier. Equally, a plurality (39%) say their present protection is about the identical in relation to the providers lined whereas about one in 4 (26%) say their present protection is healthier. But, some say their entry to lined providers (34%) and skill to see well being suppliers when wanted (22%) are worse with their present protection than they had been with Medicaid.
Not unexpectedly, in relation to evaluating the price of protection, majorities of pre-unwinding enrollees who now have one other type of insurance coverage are extra essential concerning the prices related to their present protection. Two-thirds (67%) of those adults say the out-of-pocket prices of their present protection are worse in comparison with Medicaid. Equally, two in three (65%) say the month-to-month premiums they pay for his or her new protection are worse when in comparison with Medicaid. The prices related to Medicaid, together with co-pays and premiums, are typically nominal, and related to a recipient’s earnings.
Over half of earlier Medicaid enrollees who’ve one other type of protection report problem affording month-to-month premiums and out-of-pocket prices. About six in ten (59%) say it’s no less than “considerably troublesome” for them to afford the out-of-pocket prices related to their present protection – which embody co-pays and deductibles. A slight majority (54%) report problem affording their month-to-month premiums.
Prices Are a Barrier to Acquiring Well being Insurance coverage for Some Who Misplaced Medicaid
Amongst pre-unwinding Medicaid enrollees who are actually uninsured (8%), greater than half (54%) say that they haven’t gotten one other type of medical health insurance due to the associated fee. Moreover, about one-third (36%) say they’re nonetheless making an attempt to get Medicaid protection. About one in 4 (27%) usually are not conscious of different insurance coverage choices, which can point out an data hole on various protection choices throughout their transition from Medicaid. Moreover, about one in 5 of these at present uninsured say they’ve been too busy to seek out alternate well being protection (22%). Most of the uninsured could also be unaware that the ACA market gives income-based premium subsidies for these with out entry to reasonably priced employer protection.
Many Enrollees With Different Types of Protection or Who Are Now Uninsured Cite Issues Over Paying for Well being Care
Enrollees who now produce other non-Medicaid protection are much less doubtless than those that retained their Medicaid protection to specific fear about affording some primary bills, nevertheless they’re extra doubtless to say they fear about well being care prices and payments. For instance, no less than three-quarters of those that now have non-Medicaid insurance coverage (76%) or who are actually uninsured (78%) say they’re apprehensive about affording the price of well being care providers, whereas fewer than half (47%) of those that nonetheless have Medicaid categorical this concern. Giant majorities of those that produce other protection (75%) or who’re uninsured (79%) are apprehensive about sudden medical payments, in comparison with six in ten of those that stay on Medicaid (60%). Those that now produce other types of protection are about twice as doubtless as those that nonetheless have Medicaid to say they’re apprehensive about affording their month-to-month medical health insurance premium (50% vs. 26%). (Some enrollees who nonetheless have Medicaid even have further protection by means of employers or Medicare, which can have extra pricey month-to-month premiums). Moreover, enrollees who are actually uninsured (70%) or who produce other protection (50%) are more likely than those that stay on Medicaid (33%) to say they’re apprehensive about affording prescribed drugs.
These Who Had been or Nonetheless Are on Medicaid Charge It Positively
General, a majority of enrollees charge Medicaid positively. About three-quarters (77%) of adults who had been enrolled previous to the beginning of unwinding charge their expertise with Medicaid as “wonderful” (34%) or “good” (43%). About one in 4 give Medicaid a detrimental ranking of both “truthful” (19%) or “poor” (4%).
Majorities throughout racial and ethnic teams, together with no less than three in 4 Black enrollees (77%), Hispanic enrollees (79%), and White enrollees (79%) charge Medicaid positively. Moreover, scores are persistently optimistic throughout each Medicaid growth states (79%) and in non-expansion states (71%).
Shedding Medicaid appears to be driving some perceptions of this system with greater than a 3rd of those that are actually uninsured giving Medicaid a detrimental ranking, doubtless reflecting some frustration with having misplaced their protection.
Previous KFF analysis has proven that Medicaid enrollees usually have worse self-reported well being standing and due to this fact usually tend to be increased customers of well being care providers. It is usually well-documented that top well being care customers are sometimes extra essential of their insurance coverage protection. However general, Medicaid enrollees give Medicaid optimistic scores on most value and entry measures. No less than six in ten pre-unwinding enrollees charge their Medicaid insurance coverage as “wonderful” or “good” in relation to the standard of medical suppliers accessible to them (70%), the quantity they should pay out-of-pocket to see a health care provider (68%), the quantity they should pay to fill a prescription (68%), and the supply of suppliers lined by Medicaid (62%). Over half (56%) of pre-unwinding enrollees say Medicaid insurance coverage is “wonderful” or “good” in relation to the specialists which might be lined. About half (46%) say the identical about psychological well being suppliers and providers which might be lined, although a couple of quarter (26%) say the psychological well being facet doesn’t apply to them since they don’t use these providers. Throughout a few of the measures requested about, a notable share say the query didn’t apply to them principally on account of them not accessing such a service.