Enrollment in Medicaid has grown considerably throughout the coronavirus pandemic. Provisions within the Households First Coronavirus Response Act (FFCRA) require states to supply steady protection for Medicaid enrollees till the tip of the month by which the general public well being emergency (PHE) ends with a purpose to obtain enhanced federal funding. Steady enrollment has helped to protect protection and halted Medicaid churn. Nonetheless, when the PHE ends, states will start processing redeterminations and tens of millions of individuals may lose protection if they’re not eligible or face administrative limitations regardless of remaining eligible. Current state enrollment and renewal procedures, in addition to their approaches to the unwinding of the continual enrollment requirement, may have main implications for Medicaid enrollment and broader protection.
The twentieth annual survey of state Medicaid and Youngsters’s Well being Insurance coverage Program (CHIP) officers performed by KFF and the Georgetown College Heart for Youngsters and Households in January 2022 presents a snapshot of actions states are taking to arrange for the lifting of the continual enrollment requirement, in addition to key state Medicaid enrollment and renewal procedures in place throughout the PHE. The Facilities for Medicare and Medicaid Companies (CMS) launched new steerage on March 3, 2022, which emphasizes selling continuity of protection and avoiding inappropriate protection terminations when the continual enrollment requirement ends. Whereas this latest steerage was launched after the survey was fielded, state responses reported right here illustrate how states anticipate to method the unwinding of steady enrollment and what the results of the brand new steerage could also be.
Plans for the Finish of the PHE
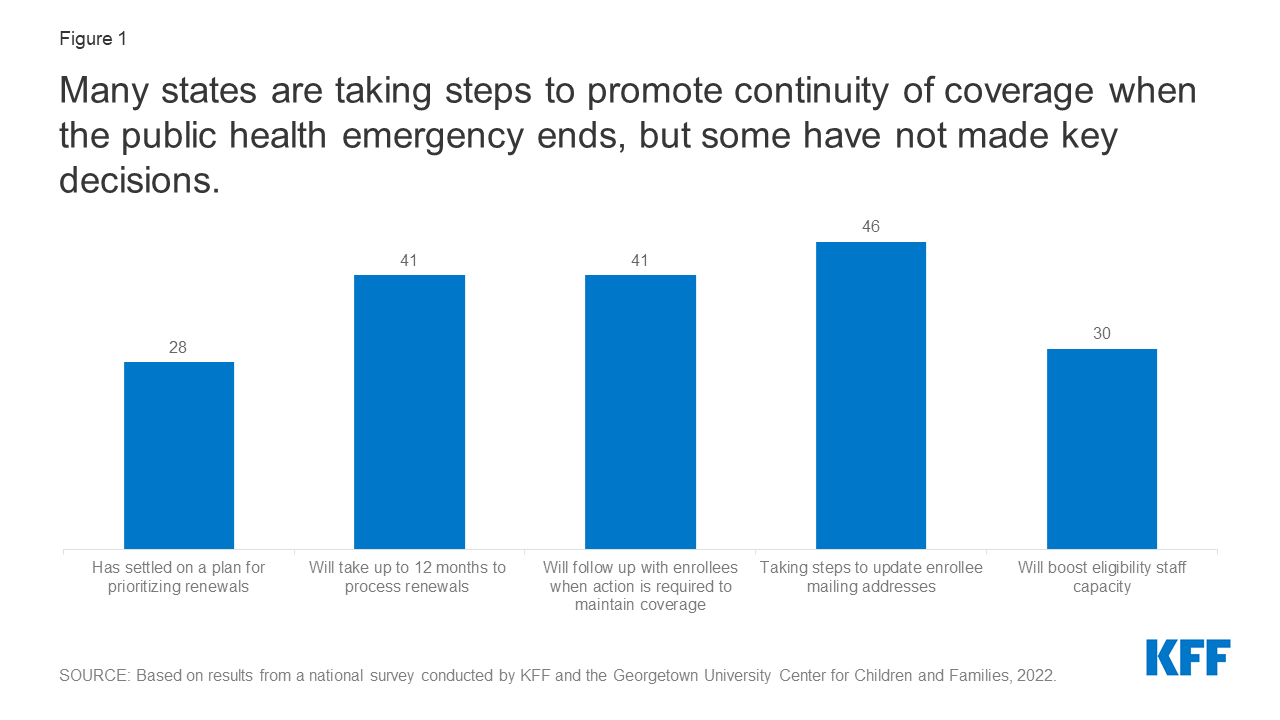
States are required to develop plans for the way they’ll prioritize excellent eligibility and renewal actions when the continual protection requirement is lifted; simply over half of states (27) have decided their method. On the time of the survey, given uncertainty across the timing of the tip of the PHE, timing of extra steerage from the CMS, and the way forward for the Construct Again Higher Act, it’s maybe not shocking that many states have but to finalize their plans. Nonetheless, having plans in place early will permit for higher preparation and can allow states to speak their plans to enrollees and different stakeholders within the state. Among the many states with plans, eleven states point out they’ll goal people who look like not eligible first, whereas eight states plan to conduct contemporary renewals primarily based on the person’s renewal month, and eight have adopted a mix or hybrid method. Whereas most states plan to attend till the continual enrollment requirement is lifted to renew disenrollments, three states haven’t but determined whether or not they’ll forgo enhanced federal funding and start disenrollments earlier than the tip of the PHE. Nonetheless, even when states start disenrollments previous to the tip of the PHE, they have to nonetheless comply with the unwinding steerage CMS has issued.
Fifteen states point out they’ll conduct digital knowledge matches to establish and goal enrollees for precedence motion who might not be eligible after the continual enrollment requirement is lifted. States should not required to conduct knowledge matches in between renewal intervals. Whereas knowledge matches can establish individuals who skilled a change in earnings or circumstance that makes them not eligible, broad knowledge searches may additionally establish inconsistent or inaccurate info that doesn’t impression eligibility and will result in eligible people shedding protection if they don’t comply with up.
Nearly all of states (41) plan to take as much as a full yr to course of redeterminations and return to routine operations; nevertheless, seven states plan to renew regular operations extra rapidly. When states resume redeterminations on the finish of the PHE, they might want to conduct a contemporary evaluation of eligibility primarily based on present circumstances earlier than disenrolling anybody from Medicaid. Present CMS steerage offers states as much as 12 months to provoke and 14 months to finish all redeterminations and 41 states point out they’ll take no less than 9 months and as much as the total yr. The elimination of the improved federal Medicaid matching charge (on the finish of the quarter by which the PHE ends) may put fiscal or political stress on states to maneuver extra rapidly. The chance of shifting rapidly is that there shall be much less time to conduct outreach to enrollees and develop employees capability to course of renewals. CMS encourages states to provoke redetermination on not more than 1/9th of their whole caseload every month to attenuate this danger.
When the continual enrollment requirement is lifted, a majority of states (41) plan to follow-up with enrollees when motion should be taken to keep away from a lack of protection attributable to lacking info. States should not required to comply with up with enrollees who don’t reply to a renewal request and should merely ship a termination discover if no response is acquired inside 30 days. Nonetheless, sending reminder notices through mail – and in addition by means of different communication modes, equivalent to cellphone, textual content, and/or electronic mail – can enhance the response charge to renewal requests and scale back the quantity of people that stay eligible however are disenrolled on the finish of the PHE as a result of they didn’t reply to a request for info.
In preparation for the tip of the PHE, states are taking steps to replace enrollee mailing addresses. The 2-year COVID-19 emergency has probably exacerbated longstanding difficulties in reaching enrollees by mail. In response, the overwhelming majority of states (46) are planning actions to replace mailing addresses earlier than the tip of the PHE, together with conducting knowledge matches with the USA Postal Service (USPS) Nationwide Change of Handle database; working with managed care organizations (MCOs); and conducting outreach campaigns. As well as, 35 states will follow-up on returned mail to try to find an enrollee earlier than terminating protection.
Anticipating the necessity for added employees assets on the finish of the PHE, 30 states plan to take steps to spice up employees capability. Most states are taking a number of actions that embrace approving time beyond regulation, hiring new eligibility staff or contractors, or borrowing employees from different items or companies.
Most states are capable of report key metrics wanted to observe the unwinding course of. Virtually all states (50) report they’re able to monitoring name middle statistics and a majority (41) are capable of report the share of disenrollments that had been decided ineligible versus disenrollments attributable to procedural causes. Having well timed and dependable knowledge from states shall be wanted to observe the unwinding course of and assess whether or not extra steps ought to be taken to keep away from protection losses amongst those that stay eligible. In latest steerage, CMS has indicated it is going to require states to report month-to-month knowledge to observe their progress on unwinding and compliance with present guidelines, though there isn’t any indication the information shall be launched publicly.
In 20 states capable of report, it’s estimated that about 13% of Medicaid enrollees shall be disenrolled when the continual enrollment requirement ends. Nonetheless, the estimates vary extensively throughout reporting states from about 8% to over 30% of whole enrollees. Based mostly on obtainable knowledge, most states report that a rise in earnings would be the main motive for the disenrollment though a number of states additionally anticipate incomplete renewals or lacking documentation shall be a main motive for disenrollment. If these estimates maintain true, tens of millions of individuals will lose Medicaid protection within the months following the tip of the PHE; nevertheless, many kids will probably be eligible for CHIP and lots of adults will probably be eligible for Inexpensive Care Act (ACA) Market or different protection. Efficiently transitioning these people into these different protection choices may keep away from gaps in protection and scale back the quantity who lose protection altogether and grow to be uninsured.
Enrollment and Renewal Insurance policies Through the PHE
Even throughout the PHE, states proceed to streamline software processes and combine non-MAGI and non-health packages into the system that determines MAGI Medicaid eligibility. In virtually all states, functions will be submitted on-line, by phone, in particular person, or by mail. Moreover, almost all states (48) now supply on-line accounts for Medicaid and CHIP enrollees that make it simpler for people to submit and entry details about their protection. States have taken steps to enhance the cell friendliness of their functions and on-line accounts. All states use digital knowledge matches from a wide range of knowledge sources to confirm earnings eligibility and, in consequence, most states (43) can present eligibility determinations in actual time (inside 24 hours).
Whereas states can’t disenroll individuals, as of January 2022, most states (42) report processing ex parte renewals and sending renewal varieties (30 states) to cut back backlogs in renewals on the finish of the PHE. By persevering with ex parte renewals throughout the PHE, states have been capable of renew protection for 12 months for individuals who stay eligible. Of the 42 states actively processing ex parte renewals, almost two-thirds (30 states) are sending renewal varieties or requests for documentation when they’re unable to substantiate ongoing eligibility by means of digital knowledge sources, though they could not disenroll anybody throughout the PHE. By processing ex parte renewals and sending out renewal varieties, states may have a smaller backlog of delayed renewals or pending actions when the PHE ends.
Medicaid and CHIP Eligibility
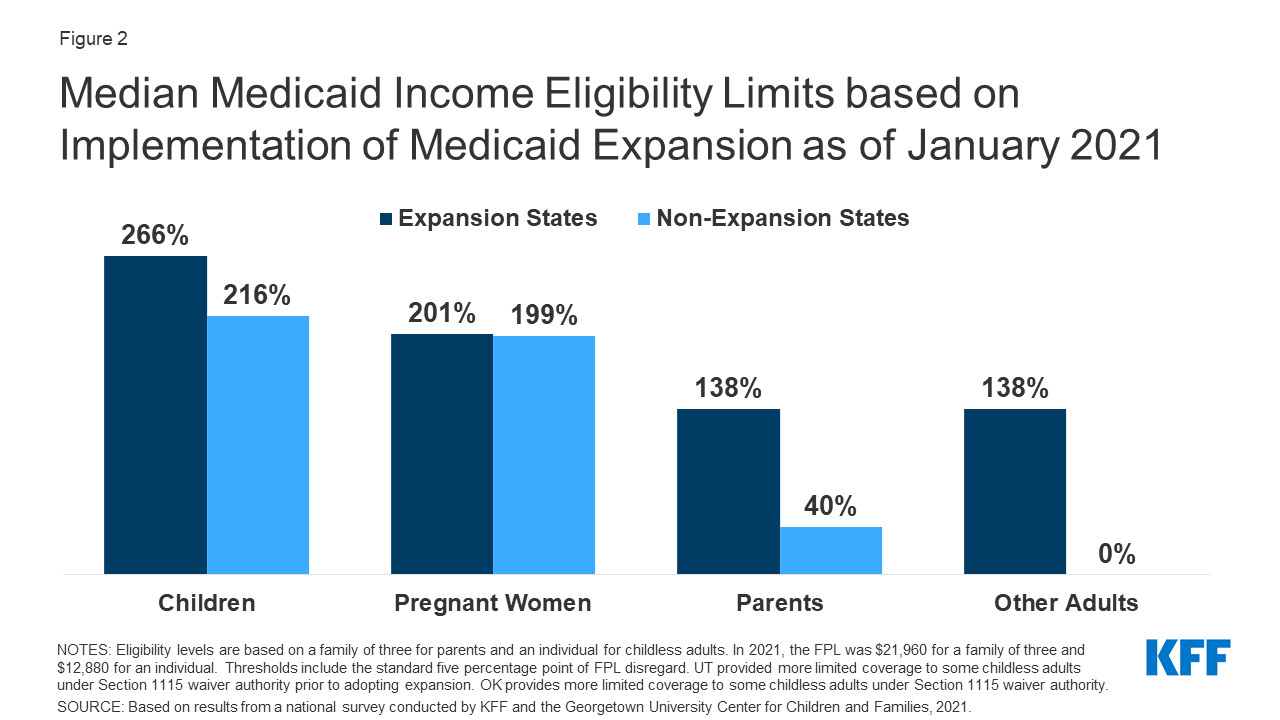
As of January 2022, Medicaid and CHIP eligibility was steady because the PHE protections remained in impact for the whole lot of 2021. Oklahoma and Missouri applied the ACA Medicaid grownup enlargement in 2021, leaving solely 12 states that haven’t crammed the protection hole for low-income adults. Within the 12 states that haven’t applied the Medicaid enlargement, eligibility for folks stays extraordinarily low (starting from 16% to 100% of the poverty stage) and solely Wisconsin covers adults with out dependent kids (by means of a waiver of normal Medicaid eligibility guidelines). Eligibility ranges for youngsters and pregnant girls held fixed with median eligibility at 255% of the federal poverty stage (FPL) and 205% FPL respectively.
Trying Forward
Current CMS steerage offers guardrails and flexibilities for states to advertise continuity of protection throughout the unwinding interval; nevertheless, state choices and actions may have implications for Medicaid enrollment. Just lately launched steerage emphasizes methods to advertise continuity of protection. The steerage reiterates present choices for states, equivalent to adopting 12-month steady eligibility for youngsters and lengthening postpartum protection for 12 months, and offers extra flexibilities, together with utilizing Supplemental Vitamin Help Program (SNAP) eligibility to resume Medicaid protection. How states method the unwinding of the continual enrollment requirement will have an effect on the extent to which eligible people retain protection and people who are not eligible are capable of transition to different protection. Outcomes will differ throughout states as they make totally different decisions and cautious monitoring of state progress all through the unwinding interval can present info to evaluate fiscal results and state efforts to advertise continuity of protection.
The destiny of the Construct Again Higher Act (BBBA) may have implications for total protection. The BBBA contains provisions to shut the Medicaid protection hole in states that haven’t adopted the ACA Medicaid enlargement and to increase the improved Market premium subsidies initially made obtainable by the American Rescue Plan Act (ARPA), which have made protection extra inexpensive for tens of millions of individuals. Whereas the variety of people who find themselves uninsured has not elevated throughout the PHE as many had predicted, tens of millions of individuals may lose protection if those that proceed to be eligible for Medicaid should not capable of retain protection, and if the provisions within the BBBA that shut the protection hole and make Market protection extra inexpensive should not enacted.