Introduction
Medicaid is the first funding supply for household planning companies for low-income individuals and is collectively financed and administered by the federal and state governments. The federal Medicaid statute establishes minimal federal requirements, and for many years, has labeled household planning as a compulsory profit class that each one state applications should cowl, however doesn’t outline precisely what companies should be included. For probably the most half, these companies are outlined by the states inside broad federal pointers. This report presents findings from a 2021 survey of states on insurance policies associated to protection of household planning companies underneath Medicaid.
The vary of household planning companies that states make obtainable to their beneficiaries is formed by many components, together with longstanding federal insurance policies associated to protection of household planning companies, federal necessities for protection of preventive companies and prescribed drugs, and states’ utility of utilization controls equivalent to sustaining most popular drug lists (PDL), requiring using generics earlier than model names, step remedy protocols, and prior authorization. States have appreciable discretion relating to Medicaid eligibility standards, managed care enrollment, and cost buildings which additionally have an effect on beneficiaries’ protection for and entry to household planning care in addition to the quantity, period and scope of the companies which can be lined.
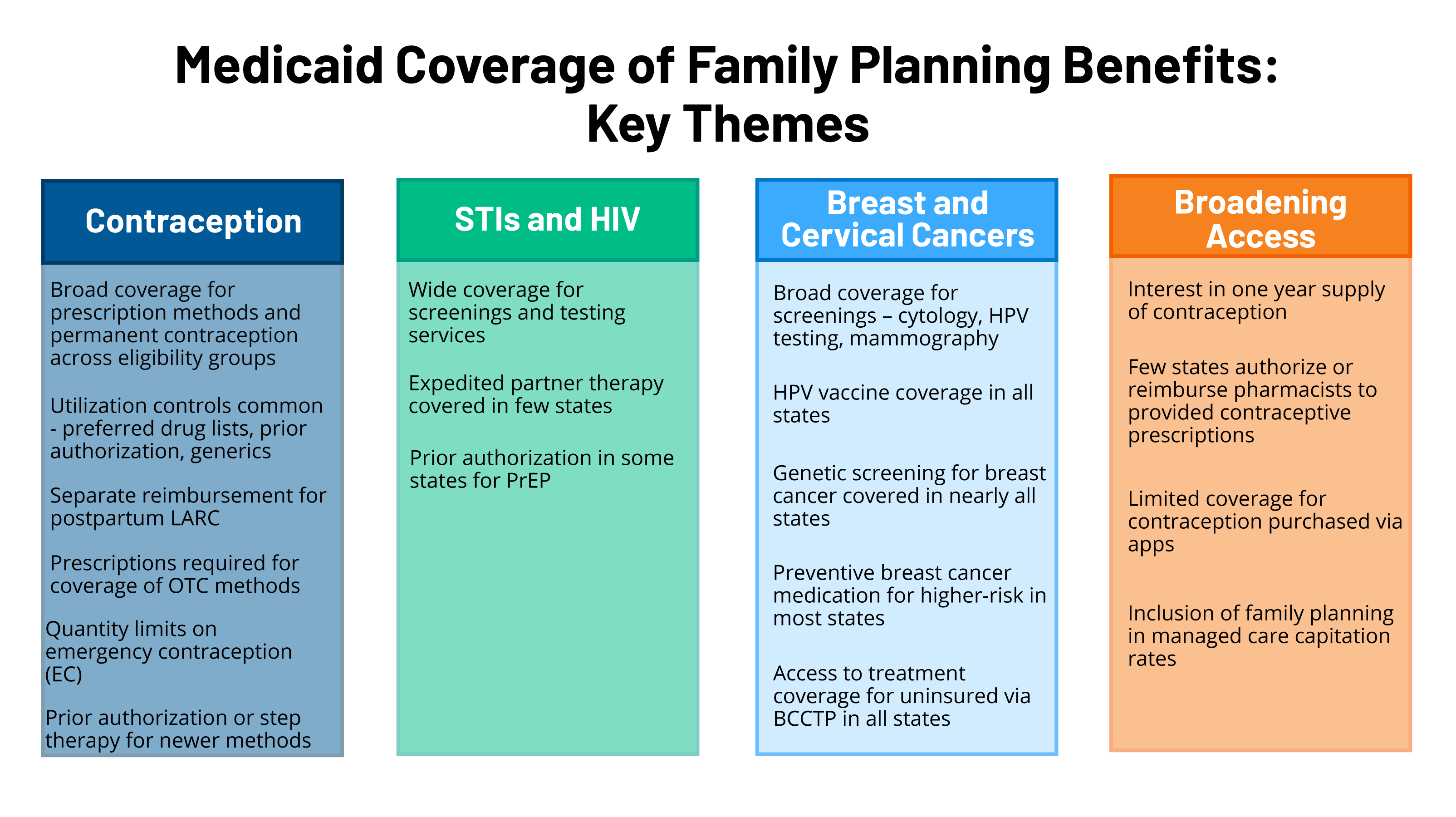
To acquire details about state Medicaid household planning protection insurance policies for adults, KFF and Well being Administration Associates (HMA) performed a survey of state Medicaid businesses relating to protection of sexual and reproductive well being care companies. Federal requirements for various Medicaid eligibility pathways might fluctuate: conventional Medicaid eligibility, which was in place previous to the Inexpensive Care Act (ACA), the Medicaid enlargement pathway in states which have expanded eligibility underneath the ACA, and restricted scope household planning applications for people who don’t qualify via different pathways. The place related, variations in state insurance policies between these pathways are highlighted. This report presents survey findings from the states that responded (41 states and District of Columbia) about protection insurance policies for fee-for-service Medicaid in place as of July 1, 2021, for the next classes of household planning advantages: prescription contraceptives, over-the-counter strategies, STI and HIV companies, properly girl care, breast and cervical most cancers companies, and managed care companies. Determine 1 summarizes key themes from the survey findings.
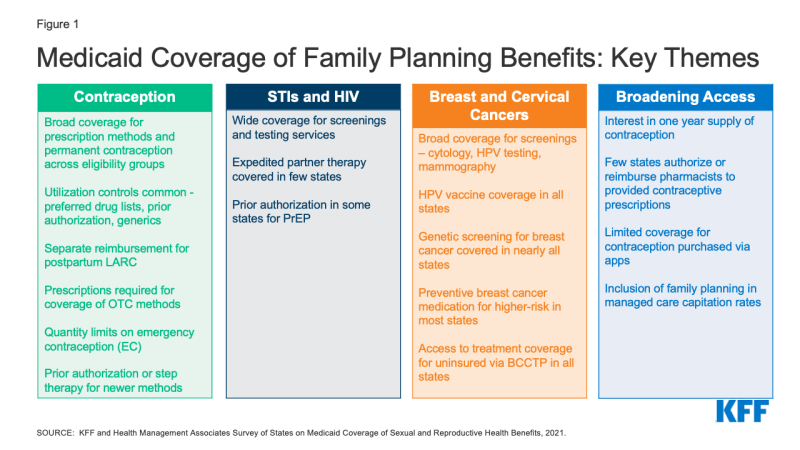
Determine 1: Medicaid Protection of Household Planning Advantages: Key Themes
Key Takeaways
Contraception
Whereas all responding states (41 states and DC) cowl prescription contraceptive strategies authorised by the Meals and Drug Administration (FDA), many apply utilization controls equivalent to amount limits, age restrictions, generic necessities, and Most popular Drug Lists (PDLs). Federal guidelines require state Medicaid applications to cowl all prescribed drugs from producers which have entered right into a federal rebate settlement. Because of this, all state Medicaid applications have open formularies that embody protection for all prescription contraceptives. Nonetheless, to manage prices and promote high quality, states might make use of utilization controls that may limit entry to particular medication. Frequent controls embody limiting the remedy amount that may be prescribed at one time, requiring use and trial of generics earlier than a model identify product, implementing a most popular drug record, and requiring prior authorization earlier than a sure product may be reimbursed. Some states, for instance, use utilization controls to restrict entry to newer contraceptive merchandise just like the Annovera Ring and Phexxi.
Few states reported imposing utilization controls on protection of intrauterine gadgets (IUDs) and implants. Most states additionally reported separate reimbursement for postpartum IUDs and implants moderately than inclusion in a worldwide cost for pregnancy-related companies. IUDs and implants, the 2 types of long-acting reversible contraceptives (LARCs), are among the many handiest strategies to stop being pregnant and likewise the most costly. Lately, there have been appreciable state and federal efforts to facilitate entry to LARCs by enhancing reimbursement, notably within the postpartum interval, an necessary time for start spacing and prevention of undesirable or mistimed pregnancies. Only a few states reported imposing limitations on entry to those strategies, and many of the responding states reported reimbursing postpartum LARCs individually from a maternity world price to clinicians and hospitals, averting what would in any other case end in a monetary disincentive for postpartum LARC placement.
All responding states cowl at the least one type of emergency contraception (EC) capsule underneath their conventional Medicaid program, however some states impose amount limits and lots of require prescriptions for Plan B, though it’s authorised for over-the-counter availability for EC capsules. Emergency contraceptive capsules forestall being pregnant if taken inside the first few days after unprotected intercourse. They aren’t abortifacients as they can not disrupt a longtime being pregnant. All however one state report protection of prescription emergency contraceptive capsules (ella or ulipristal acetate) throughout eligibility teams, and all however two cowl over-the-counter (OTC) Plan B (levonorgestrel) underneath their conventional Medicaid applications. Far fewer states, nonetheless, reported masking Plan B and not using a prescription (7 states). Offering protection and not using a prescription can expedite entry, particularly for a contraceptive with a brief window of effectiveness equivalent to emergency contraceptive capsules.
Most states shouldn’t have a course of for masking over-the-counter (OTC) strategies equivalent to condoms or sponges and not using a prescription. Thirty-eight states reported requiring a prescription from a supplier to cowl OTC strategies, in step with federal steerage {that a} prescription is required to acquire federal Medicaid matching funds. Ten states, nonetheless, reported masking some or all OTC contraceptives by increasing pharmacists’ scope of apply to prescribe and dispense particular contraceptives, both independently, underneath the supervision of a licensed supplier with prescribing authority via a collaborative apply settlement (CPA), or via protocols equivalent to a statewide “standing order.”
STIs and HIV
Practically all reporting states cowl testing and therapy for sexually transmitted infections (STIs) and routine HIV screening underneath their conventional Medicaid program, and virtually all states align non-contraceptive household planning advantages throughout eligibility pathways inside their state. Take care of STIs is often thought-about a part of medical household planning companies. Underneath Medicaid, nonetheless, STI therapy is assessed as a “household planning associated” service. All responding states reported masking STI testing, therapy, and counseling underneath their conventional Medicaid program, and virtually all align protection throughout eligibility teams. Moreover, virtually all of the responding states additionally reported masking routine HIV screening of their conventional Medicaid applications.
Few states, nonetheless, reported masking Expedited Associate Remedy (EPT) which is endorsed by the CDC as an efficient technique to manage the transmission of STIs. Expedited accomplice remedy (EPT) permits the therapy of the sexual companions of a affected person recognized with an STI with out examination and is beneficial by the CDC for therapy of STIs. Nonetheless, simply 9 of the responding states reported EPT protection.
Some states require prior authorization for the supply of Pre-Publicity Prophylaxis (PrEP), a medicine taken to stop HIV acquisition, and a few states don’t cowl it as a profit underneath restricted scope household planning applications. PrEP drugs can forestall people from buying HIV, and are beneficial for people at greater danger of HIV an infection. Like different prescribed drugs, Medicaid applications are required to cowl PrEP, however 12 of the responding states reported having a previous authorization requirement. Seven states reported that they don’t cowl PrEP as a part of their restricted scope household planning applications, the place protection is non-obligatory as a result of states can outline the household planning and associated companies that they embody for beneficiaries in these applications.
Cervical and Breast Cancers
All of the responding states cowl companies to stop, detect, and diagnose cervical and breast most cancers, however there’s variation within the forms of companies which can be included and whether or not they’re lined underneath restricted scope household planning applications. Screening for cervical and breast cancers is taken into account acceptable for provision throughout a household planning go to. Each responding state reported protection of their conventional Medicaid program for HPV vaccines, cervical most cancers screenings utilizing cervical cytology and HPV checks, and colposcopy and LEEP or chilly knife conization, that are beneficial companies following an irregular screening. Nonetheless, protection for these companies isn’t common in restricted scope household planning-specific applications.
The entire responding states cowl screening mammograms for individuals eligible via the normal Medicaid pathway, and most cowl genetic screening (BRCA) and counseling in addition to remedy to stop or scale back danger of breast most cancers for ladies at greater danger. As with cervical most cancers screenings, each taking part state covers mammograms underneath conventional Medicaid, however not all cowl them for enrollees within the restricted scope household planning applications.
Along with routine mammography, screening for genetic mutations and preventive drugs are beneficial for some ladies at greater danger for breast most cancers. Whereas these preventive companies are thought-about non-obligatory underneath conventional Medicaid, 40 states cowl genetic screening and counseling for BRCA mutations and 36 cowl preventive remedy for high-risk ladies of their conventional Medicaid program.
Broadening Entry
Whereas almost half of responding states cowl a one-year provide of contraceptives at a time, few states enable pharmacists to prescribe and be reimbursed for contraceptive companies offered to Medicaid beneficiaries. Prolonged provide and pharmacist prescribing of contraceptives are two avenues for enhancing entry to household planning companies. Various states report that they permit Medicaid protection for a one-year provide of sure hormonal strategies, together with 18 states that allow a one-year provide of oral contraceptives. Nonetheless, fewer than a dozen of the responding states reimburse for pharmacist provision of contraceptives.
The provision of contraceptives through on-line apps is proliferating, however few states present Medicaid protection of contraceptives obtained via these platforms. Lately, plenty of corporations have been offering principally hormonal contraceptive strategies via on-line platforms for purchasers to acquire contraceptives usually prescribed utilizing an asynchronous telehealth protocol. Whereas a few of these corporations don’t settle for any third-party funds, eight states reported that Medicaid covers contraceptive purchases secured via these apps. That is an evolving space, however total Medicaid protection for these merchandise is proscribed right now.
***
Medicaid represents a big supply of protection of the complete vary of contraceptive strategies and associated household planning companies for low-income individuals. Lately, Medicaid enrollment, notably of reproductive age adults, has grown because of state choices to broaden Medicaid underneath the ACA and to ascertain restricted scope household planning applications. This survey finds sturdy protection of many contraceptive companies and provides, however variation within the utility of utilization controls. Whereas there’s broad protection for prescription contraceptives (as a consequence of necessities and the drug rebate program) entry to newer and OTC strategies in addition to adoption of insurance policies which have been demonstrated to facilitate entry, equivalent to 12-month allotting or permitting pharmacists to prescribe and be reimbursed, are much less frequent. Moreover, some states haven’t adopted protocols that facilitate the prevention of STIs and HIV equivalent to expedited accomplice remedy or protection for PrEP with out prior authorization, necessary public well being advances which have the potential to enhance the sexual well being of high-risk populations. Within the coming years, notably if entry to abortion companies turns into more and more restricted, the alternatives that states make relating to Medicaid eligibility and protection for household planning companies will make a important distinction within the reproductive well being and well-being of thousands and thousands of individuals throughout the nation.
Background
Medicaid, the nation’s well being protection program for low-income individuals, performs a main position in financing and offering entry to sexual and reproductive well being companies for thousands and thousands of low-income people. This system covers greater than 20 million adults ages 18 to 49 and is the most important supply of public funding for household planning companies. This system is operated collectively by the federal and state governments, who share duty for cost of companies, whereas states set eligibility ranges and decide the quantity, period, and scope of lined advantages inside broad federal parameters.
Financing and protection of household planning companies is exclusive inside the Medicaid program. Federal Medicaid regulation classifies household planning companies and provides as a “obligatory” profit class that states should cowl, however it doesn’t formally outline the precise companies that should be included, giving states discretion as to which companies they embody on this class. As well as, federal regulation:
- Prohibits suppliers from charging copayments to beneficiaries or another type of affected person price sharing for household planning companies
- Establishes a 90% federal matching charge (FMAP) for the prices of companies categorized as household planning, the next proportion than for different companies. States pay the remaining 10% of prices
- Entitles beneficiaries to acquire household planning companies from any supplier that participates within the Medicaid program, referred to as free selection of supplier, together with for beneficiaries with obligatory enrollment in managed care organizations (MCOs)
Protection for prescribed drugs is one other necessary ingredient in Medicaid protection of household planning companies. All states have chosen to cowl prescribed drugs, though it’s an non-obligatory advantages class underneath federal regulation. Moreover, all state Medicaid applications should keep an “open formulary,” that means that Medicaid covers almost all FDA-approved medication from producers that agree to supply rebates for a portion of drug funds. States, nonetheless, can impose utilization management insurance policies to restrict spending and promote high quality, which may limit entry to some medication, together with sure contraceptives.
Enrollees who qualify for Medicaid via conventional pathways, these in place previous to the Inexpensive Care Act (ACA) are entitled to protection for household planning companies. A number of states have established particular restricted scope “household planning applications” that reach Medicaid protection for household planning companies solely to people who aren’t eligible for conventional Medicaid (normally as a result of their incomes exceed the state earnings eligibility thresholds or don’t in any other case qualify for Medicaid). States can set up household planning-only applications both via federal Part 1115 analysis and demonstration waivers or State Plan Amendments (SPAs) that should be authorised by the Facilities for Medicare and Medicaid Companies (CMS), the federal company that oversees the Medicaid program. States can resolve which companies they cowl in these restricted scope household planning applications, and pharmacy protection underneath restricted scope household planning applications is restricted to household planning and associated companies.
Moreover, states which have opted to broaden Medicaid eligibility underneath the ACA are required to cowl “important well being advantages,” together with preventive companies beneficial by the U.S. Preventive Companies Activity Power (USPSTF), preventive companies for ladies recognized by the federal Well being Companies and Sources Administration (HRSA) based mostly on the suggestions of the Ladies’s Preventive Companies Initiative (WPSI), and vaccines beneficial by the Advisory Committee on Immunization Practices (ACIP). The slate of preventive companies beneficial by these committees embody a number of household planning and associated companies, particularly FDA-approved, approved and cleared contraceptives with a prescription, screenings for STIs and HIV, screening for cervical and breast cancers, the HPV vaccine, properly girl visits, and screening for intimate accomplice violence. These companies should be lined underneath ACA Medicaid enlargement, however that requirement doesn’t apply to conventional Medicaid or restricted scope household planning applications, which implies that the advantages package deal may fluctuate inside a state for various Medicaid populations (Desk 1). Nonetheless, a 2015 KFF/HMA survey discovered that the majority states have aligned protection of household planning advantages for all pathways, regardless of the differing necessities. States do fluctuate, nonetheless, within the utilization controls that they select to use.
To know the scope of protection for sexual and reproductive well being companies, the utilization controls that states undertake, variations between and inside states, and associated state Medicaid insurance policies throughout the nation, KFF (Kaiser Household Basis) and Well being Administration Associates (HMA) performed a nationwide survey of states about insurance policies in place as of July 1, 2021. States have been requested primarily about protection of companies underneath conventional Medicaid and whether or not they align protection insurance policies in restricted scope household planning applications and underneath their Medicaid expansions, the place relevant.
The survey was performed between June 2021 and October 2021. Forty-one states and the District of Columbia responded to the survey (Determine 2). As of July 1, 2021, 31 of those taking part states had carried out the ACA Medicaid enlargement, and 11 had not carried out the enlargement. Since July 1st, one of many 11 non-expansion states (Missouri) has carried out Medicaid enlargement. Of the responding states, 24 states additionally supply restricted scope household planning applications financed by Medicaid to people who don’t qualify via different Medicaid pathways. Two further states (Iowa and Missouri) function restricted scope household planning applications which can be solely state-funded as a result of they exclude suppliers that supply each household planning and abortion companies, disqualifying these applications from federal Medicaid funds. These state restrictions violate Medicaid’s freedom of selection requirement and Medicaid’s requirement to incorporate all keen suppliers, which give Medicaid beneficiaries the fitting to hunt companies from any certified supplier that participates in a state’s Medicaid program. States that didn’t reply to the survey are: Arkansas, Georgia, Kentucky, Minnesota, Nebraska, New Hampshire, New Mexico, Ohio, and South Dakota.
Introduced under are detailed survey findings from 41 states and DC regarding protection and utilization limits for reversible contraceptives and everlasting contraception, properly girl care, STI and HIV companies, companies for breast and cervical cancers, and necessities for managed care plans relating to protection of household planning companies. A majority of the states responding to the survey contract with managed care organizations (MCOs) underneath a capitated construction to ship Medicaid companies, together with household planning. Whereas the survey’s questions centered on state Medicaid insurance policies and protection underneath fee-for-service, these insurance policies kind the premise of protection for MCOs.