Latest coverage actions and proposals in Medicaid have renewed give attention to the issue of churn, or short-term lack of protection by which enrollees disenroll after which re-enroll inside a brief time frame. The Households First Coronavirus Response Act (FFCRA) handed through the coronavirus pandemic requires states to supply steady protection to Medicaid enrollees till the tip of the month by which the general public well being emergency (PHE) ends to obtain enhanced federal funding. Throughout this time, folks didn’t churn on and off Medicaid, however churn might resurface when the continual enrollment requirement ends. The Construct Again Higher reconciliation invoice into consideration in Congress would start to part out the continual enrollment requirement and the improved match starting April 1, 2022. Moreover, the invoice would require states to supply 12-month steady protection for youngsters and for postpartum people in Medicaid and the Kids’s Well being Insurance coverage Program (CHIP), which may cut back churn for these teams. At the moment greater than half of states already present 12-month steady protection for youngsters on an optionally available foundation.
To assist inform the present coverage dialogue, this transient supplies estimates of churn for folks enrolled in Medicaid in 2018. We use 2017 and 2019 as look-back and look-ahead years, respectively, so we are able to study what occurs to folks a full 12 months earlier than and after an enrollment date or disenrollment date in 2018. We additionally present estimates of churn by eligibility group and examine charges in Medicaid enlargement versus non-expansion states. General, we discover that 10% of full-benefit enrollees have a niche in protection of lower than a 12 months, and charges are larger for youngsters and adults in comparison with aged and folks with disabilities. Churn charges additionally fluctuate considerably by state, starting from 5% or much less in some states to fifteen% or extra in others. Churn has implications for entry to care in addition to administrative prices confronted by states. Element on the information and strategies underlying this evaluation are within the Strategies part on the finish of the transient.
Background
The short-term lack of Medicaid protection by which enrollees disenroll after which re-enroll inside a brief time frame, also known as “churn,” happens for a a number of causes. Enrollees might expertise short-term adjustments in revenue or circumstances that make them quickly ineligible. Alternatively, some individuals who stay eligible might face limitations to sustaining protection as a result of renewal processes and periodic eligibility checks. Eligible people are in danger for shedding protection if they don’t obtain or perceive notices or varieties requesting further info to confirm eligibility or don’t reply to requests inside required timeframes.
Some enrollees could also be at larger danger of churn than others. Working people whose month-to-month revenue fluctuates could also be extra more likely to expertise churn in states which have adopted frequent digital knowledge matches through the 12 months. For instance, grownup enrollees with out disabilities, most of whom are working, might have irregular work hours, additional time, or a number of part-time jobs that may result in month-to-month adjustments in revenue. In distinction, aged adults and folks with disabilities, notably those that qualify for Supplemental Safety Earnings (SSI), are much less more likely to expertise month-to-month revenue adjustments or different adjustments in circumstances. Most states conduct knowledge matches on a periodic foundation to determine adjustments in circumstances between annual renewal intervals. If the information checks determine adjustments in revenue or different components that have an effect on eligibility and the person is unable to resolve the discrepancy inside the specified timeframe (typically restricted to inside 10 days from the date of the discover), the particular person may be disenrolled from protection.
Churn can lead to entry limitations in addition to further administrative prices. When people who stay eligible for protection are disenrolled, they might expertise gaps in protection that would restrict entry to care and result in delays in getting wanted care. Analysis signifies that enrollees who expertise fluctuations in protection usually tend to report difficulties getting medical care and usually tend to find yourself within the hospital with a preventable situation. As well as, there are administrative prices related to disenrolling an enrollee after which subsequently processing a brand new software.
What are the charges of churn in Medicaid?
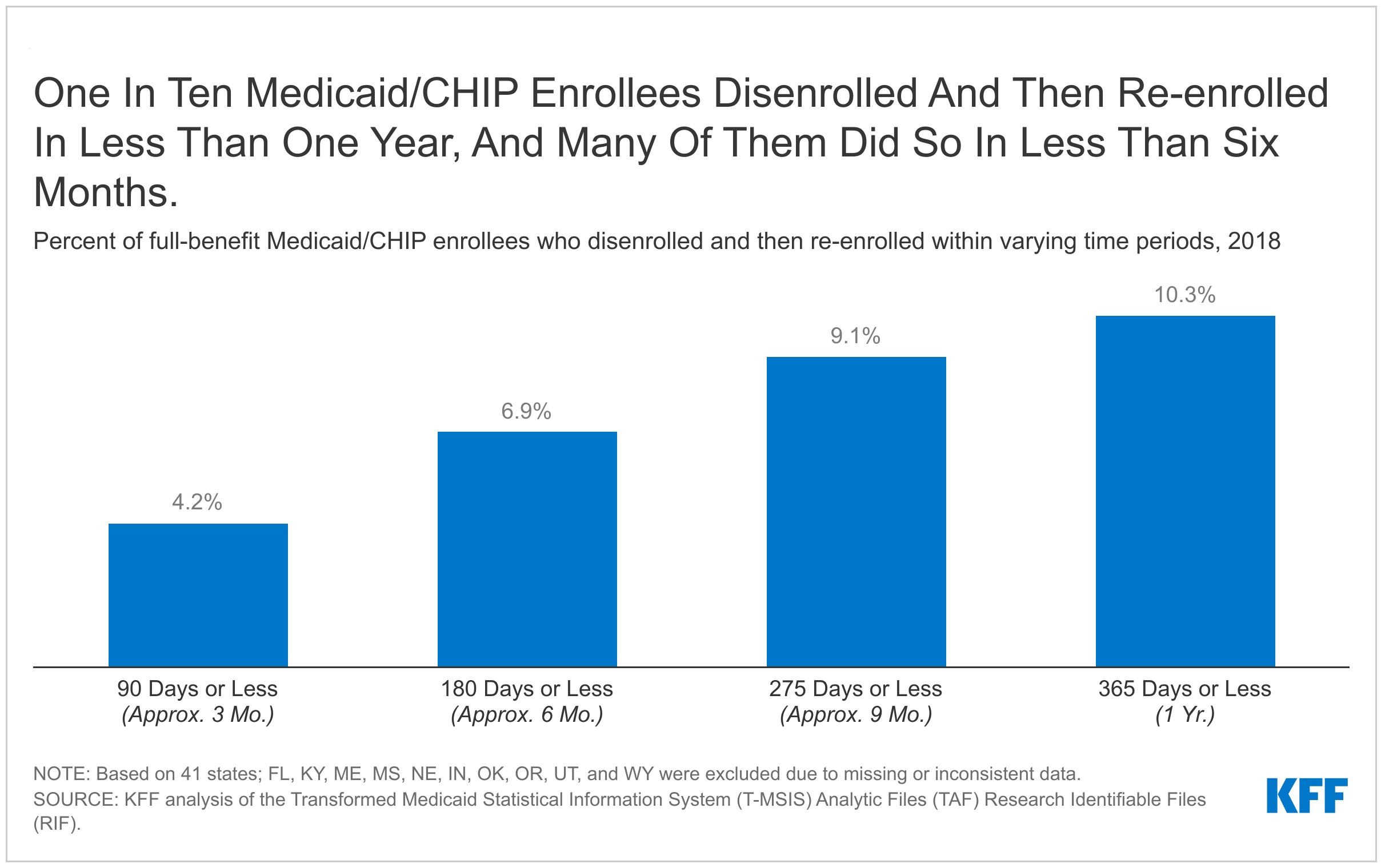
Amongst full-benefit beneficiaries enrolled at any level in 2018, 10.3% had a niche in protection of lower than a 12 months. About 4.2% have been disenrolled after which re-enrolled inside three months and 6.9% inside six months (Determine 1).
Charges of churn have been larger for youngsters and adults in comparison with aged adults and folks with disabilities (Determine 2). We estimate that 11.2% of full-benefit youngsters and 12.1% of adults have been disenrolled after which subsequently re-enrolled inside one 12 months. Evaluation additionally exhibits that charges of churn are larger for enrollees with partial profit packages, however there are comparable churn charges throughout enlargement and non-expansion states (Appendix Desk 1). Nevertheless, there may be appreciable variation in churn charges throughout states, with 4 states (HI, AZ, DC, and NC) having 5% of enrollees or fewer disenrolling after which re-enrolling inside a 12 months, and 4 states (TX, WI, NH, and PA) having 15% of enrollees or extra disenrolling and re-enrolling inside a 12 months.
What are present coverage points associated to churn?
The continual enrollment requirement associated to the coronavirus pandemic has all however halted Medicaid churn for the previous 12 months and a half, however disenrollments are anticipated resume as soon as the requirement ends. Partially as a result of steady enrollment requirement, Medicaid/CHIP enrollment has elevated from February 2020 to Might 2021 by 11.5 million (or 16.2%) to 82.8 million people. Nevertheless, when the continual enrollment requirement ends, states will start processing renewals and people might lose protection if they’re now not eligible or face limitations through the redetermination course of, reminiscent of offering required documentation.
The Construct Again Higher Act (BBBA) that’s at present being debated in Congress would part out the continual enrollment requirement starting April 1, 2022. To proceed receiving a phased-down enhanced federal match fee, states can be required to comply with guidelines about disenrolling folks that would assist to scale back charges of churn. For instance, states may solely disenroll people who’ve been enrolled a minimum of 12 consecutive months and should restrict eligibility redeterminations to a set proportion of enrollees every month by way of September 2022. States couldn’t disenroll people based mostly on returned mail until there have been a minimum of two failed makes an attempt to contact the person by way of a minimum of two modalities (e.g., mail and textual content messages). States would additionally need to report month-to-month knowledge on name heart statistics (common quantity, wait instances, and abandonment charges) in addition to charges of eligibility renewals, redeterminations, and protection terminations as a result of adjustments in circumstances (e.g., elevated revenue) or as a result of administrative causes (e.g., failing to supply required documentation).
Previous to the pandemic, some states had adopted insurance policies and processes to scale back churn and promote steady protection. For instance, as of January 2020, 35 states account for anticipated revenue adjustments, reminiscent of recurring seasonable employment or a job change, when figuring out eligibility at renewal. Some states additionally use projected annual revenue for the rest of the calendar 12 months when figuring out ongoing eligibility at renewal or when a person has a possible change in circumstances between renewal intervals. States may also implement processes that enhance communications with enrollees to assist forestall them from shedding protection as a result of they don’t obtain or reply to notices from the state. Such actions embody conducting common knowledge matches with the U.S. Postal Service Nationwide Change of Tackle Database, working with managed care plans and suppliers to replace enrollees’ handle info, and calling enrollees or sending e-mail or textual content notifications when returned mail from a discover despatched to an enrollee is acquired.
The BBBA would require states to implement 12-month steady protection for youngsters and postpartum people. States have the choice to supply 12 months of steady protection for youngsters. Underneath this selection, states enable a baby to stay enrolled for a full 12 months until the kid ages out of protection, strikes out of state, voluntarily withdraws, or doesn’t make premium funds. As such, 12-month steady eligibility eliminates protection gaps as a result of fluctuations in revenue over the course of the 12 months. A latest MACPAC evaluation discovered that states with 12-month steady protection for youngsters had decrease charges of churn amongst youngsters enrolled in Medicaid and CHIP in comparison with states with out this coverage. At the moment, 34 states present 12-month steady eligibility to a minimum of some youngsters in both Medicaid or CHIP. The Construct Again Higher Act would require states to increase 12-month steady protection for youngsters in Medicaid and CHIP and would additionally require 12-month steady protection for postpartum people, a change from the present requirement of 60-day postpartum protection.