Because the Biden Administration takes workplace, the continued results of the coronavirus pandemic and associated financial downturn are the important thing points that may considerably form Medicaid protection and financing coverage within the 12 months forward. Different points to observe in 2021 embrace efforts to take care of and develop Medicaid protection, potential adjustments in Medicaid demonstration waiver coverage, points round state budgets and Medicaid financing, initiatives to strengthen long-term providers and helps and efforts to handle social determinants of well being.
Medicaid Protection and Enrollment
Enrollment Previous to the Pandemic. Earlier than the pandemic, Medicaid enrollment progress peaked after implementation of the Reasonably priced Care Act (ACA). The ACA Medicaid growth has been adopted by 39 states and covers greater than 15 million adults. Nonetheless, Medicaid enrollment declined from 2017 by means of 2019, which has contributed to will increase within the general quantity and price of uninsured. Enrollment declines may replicate a extra strong economic system throughout these years, however experiences in some states recommend declines could have additionally been because of people experiencing challenges finishing enrollment or renewal processes. As well as, the Trump Administration promoted plenty of insurance policies that prohibit enrollment together with issuance of the general public cost rule that imposed new obstacles to acquiring everlasting immigration standing or immigrating to the U.S. (resulting in declines in participation in Medicaid and different packages broadly throughout immigrant households). The Trump Administration additionally supported proposals to repeal and substitute the ACA in addition to litigation to overturn the regulation that’s pending on the Supreme Court docket.
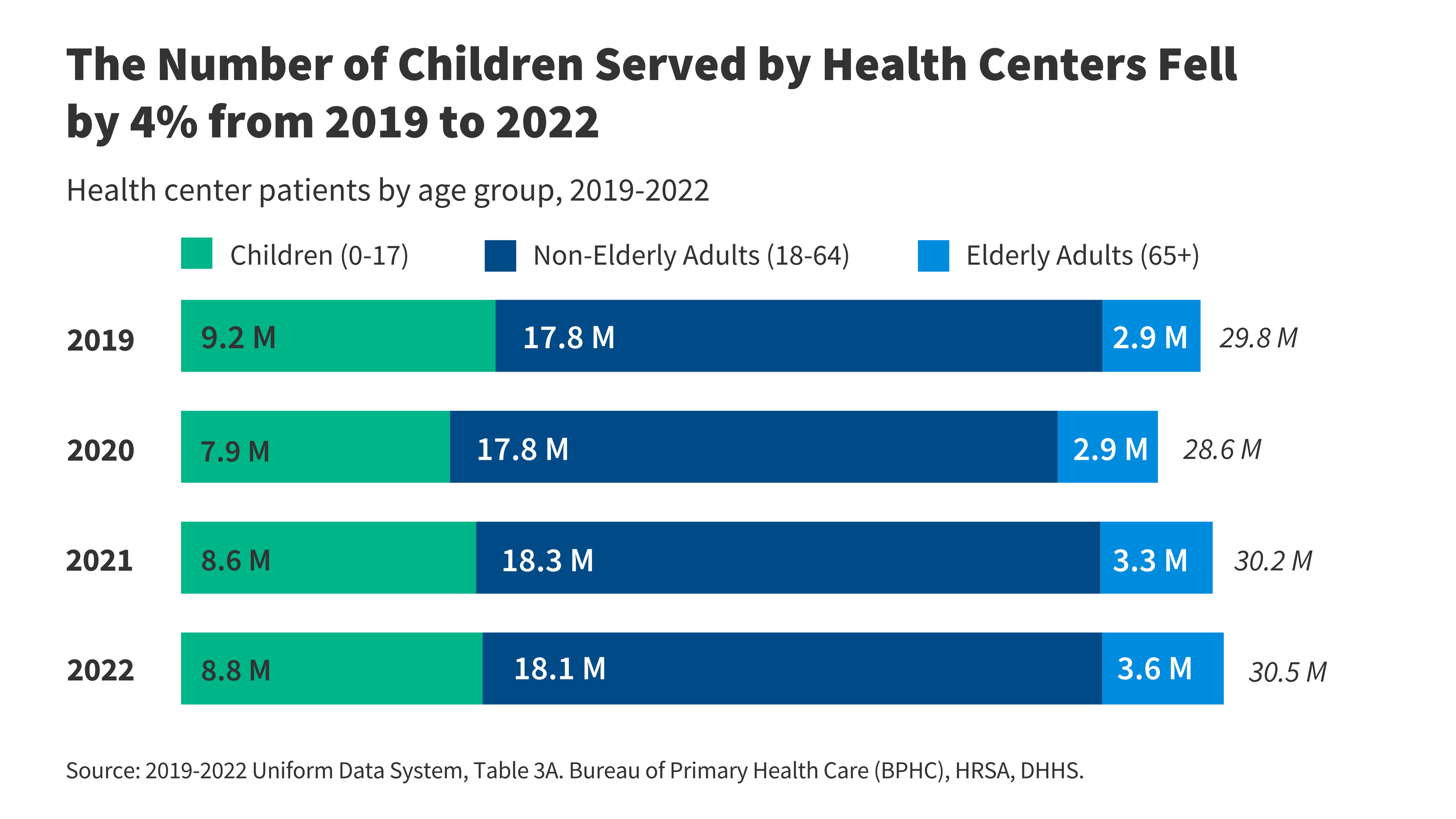
Enrollment and COVID-19. As a counter-cyclical program, Medicaid enrollment grows throughout financial downturns when extra individuals expertise revenue and job loss and qualify for protection. Because the begin of the coronavirus pandemic, enrollment in Medicaid and the Kids’s Well being Insurance coverage Program (CHIP) grew to 76.5 million in August 2020, a rise of 5.3 million from February 2020 (7.4%). This pattern doubtless displays adjustments within the economic system because of the pandemic and provisions within the Households First Coronavirus Response Act (FFCRA) that require states to make sure steady protection for present Medicaid enrollees to entry a brief enhance within the Medicaid match price. These FFCRA provisions are tied to the Public Well being Emergency (PHE) interval, which presently expires in April 2021 however could also be prolonged longer.
Key Biden Priorities to Increase Protection. Biden has proposed constructing on the ACA by growing Market premium help and making a Medicare-like public choice plan, which might be accessible to anybody and routinely cowl individuals with low incomes in states that haven’t expanded Medicaid. Whereas not as sweeping as proposals like Medicare for All, Biden’s proposals are broad adjustments that may very well be tough to go with a carefully divided Senate even with Democrats within the majority. Extra slim proposals to handle those that fall into the protection hole in states that haven’t adopted the growth embrace laws to reinstate the 100% federal matching price for states that newly undertake the growth for a time period (the present match price for the growth is 90%), or extending ACA market premium assist to individuals under the poverty stage. States which have already expanded Medicaid and are presently paying 10% of the price would possibly search for extra federal assist as nicely. Twelve states haven’t adopted the Medicaid growth, leaving many poor adults in a protection hole, ineligible for Medicaid or Market subsidies.
Different Choices to Increase Protection. There was bi-partisan help for laws that may enable states to increase postpartum Medicaid protection from the present 60 days to 12 months. One other focused bi-partisan legislative proposal is the Medicaid Reentry Act, which might enable states to cowl providers for Medicaid beneficiaries who’re incarcerated in the course of the 30 days previous their launch which may facilitate protection and entry to care post-release. As well as, Congress may contemplate laws to permit states the choices to cowl latest immigrants on Medicaid (eliminating the present 5 12 months protection ban for teams apart from pregnant ladies and kids).
What to Watch:
- How will the well being and financial results of the pandemic have an effect on Medicaid enrollment?
- How lengthy will the PHE and the upkeep of eligibility necessities be in place, and what would be the results on Medicaid protection once they finish?
- What’s going to occur with the ACA litigation pending on the Supreme Court docket?
- What efforts to guard and construct on the ACA and develop Medicaid will the Biden Administration and Congress pursue?
Medicaid Demonstration Waivers
Part 1115 waivers usually replicate priorities recognized by the states and the federal Facilities for Medicare and Medicaid Companies (CMS), in addition to altering priorities from one presidential administration to a different. Previous administrations have used waivers to develop protection, modify supply techniques, and restructure financing and different program components. Though every administration has some discretion over which waivers to approve and encourage, that discretion just isn’t limitless. Part 1115 waivers are ruled by statutory necessities in addition to longstanding govt department coverage that waivers be finances impartial to the federal authorities. The Trump administration’s Part 1115 waiver coverage has emphasised work necessities and different eligibility restrictions, cost for institutional behavioral well being providers, and capped financing.
The Biden Administration can revise present demonstration waiver coverage to give attention to increasing protection and rescind or reverse waivers or steerage that would restrict protection (together with work necessities) or cap federal financing. The Supreme Court docket is listening to instances involving the Arkansas and New Hampshire work requirement waivers this time period. The Biden Administration can also encourage waivers that develop protection to focused teams or assist make Market protection extra inexpensive. This might embrace steerage to states about utilizing Medicaid Part 1115 waivers together with Part 1332 waivers to advance public choice proposals or different methods to enhance affordability for shoppers and develop protection. As well as, whereas addressing behavioral well being and substance use dysfunction by means of waivers is prone to stay a excessive precedence, the Biden Administration could emphasize the necessity to present providers throughout a full care continuum, together with institutional group primarily based care. Waivers may be used to handle social determinants of well being.
What to Watch:
- How will the Biden Administration use Part 1115 waivers?
- Will the Biden Administration rescind sure waivers which have already been authorized?
- Will the Biden Administration difficulty steerage for states to make use of mixture Part 1115 and 1332 waivers?
- What’s going to the Supreme Court docket determine in pending litigation about work necessities?
Medicaid Financing
Medicaid’s present financing construction supplies some protections for states going through larger prices throughout financial downturns, as federal matching funds (FMAP) routinely enhance as enrollment grows. As well as, non permanent will increase within the federal share of Medicaid funds can present fiscal reduction to states, offsetting some state funds. The FFCRA supplied an FMAP enhance of 6.2 share factors by means of the tip of the quarter by which the PHE ends so supplied states meet sure necessities to take care of protection and supply entry to COVID-19-related providers. With the latest extension of the PHE, the FMAP will likely be in place by means of June 2021. Nonetheless, there’s uncertainty about how lengthy the fiscal reduction will likely be in place, and lots of states are seeing 12 months over 12 months declines in revenues. States must go balanced budgets and should face powerful decisions to chop spending (together with for Medicaid) within the upcoming fiscal 12 months. Typically throughout financial downturns, states implement supplier price cuts or profit restrictions; nevertheless, these insurance policies may very well be tough given pandemic’s well being results, as states try to help well being care suppliers and keep Medicaid supplier networks. Adjustments to the FMAP require laws and can’t be made by means of Administrative motion alone.
President-elect Biden has indicated help for additional growing the FMAP and should attempt to work with Congress to enact laws. Republican leaders have usually opposed substantial will increase in state and native help in the course of the pandemic and financial disaster, although a rise in federal Medicaid funds may very well be included in a finances reconciliation invoice that requires only a easy majority to go the Senate. The Medicaid and CHIP Fee and Entry Fee (MACPAC) in December 2020 introduced shifting towards a advice calling for an automated Medicaid countercyclical financing mannequin primarily based on earlier suggestions from the Common Accountability Workplace. The HEROES Act handed by the Home in Could after which up to date and handed once more in October would have elevated the improved FMAP to 14 share factors by means of September 2021, offering states with an estimated $55.5 billion in federal help in keeping with the Congressional Price range Workplace. Congress may additionally contemplate various choices to focus on the reduction to states experiencing larger enrollment will increase. Nonetheless, it stays unclear if Congress will present extra reduction by means of the FMAP or if they’ll revisit the upkeep of effort necessities as a part of one other coronavirus reduction bundle.
One other Medicaid financing difficulty may very well be to re-examine the financing for Puerto Rico and the remainder of the territories. Federal funding for Medicaid within the territories is topic to a statutory cap and a hard and fast federal matching price, not like within the states, the place federal Medicaid funding just isn’t capped, and the federal share varies primarily based on states’ per capita revenue. Because of the capped financing, the efficient FMAP is usually decrease than the statutory ranges. Hurricanes and different emergencies exacerbated long-standing fiscal points within the territories. Further funding help (by means of each elevated quantities and will increase within the FMAP) have been supplied by means of the ACA after which in response to different emergencies. For Puerto Rico, help is predicted to run out on the finish of FY 2021. Congress may prolong reduction or make extra everlasting funding adjustments for Puerto Rico and different territories.
What to Watch:
- To what extent will the pandemic proceed to have an effect on state budgets and skill to finance Medicaid? Will states suggest Medicaid cuts within the upcoming state fiscal 12 months?
- How lengthy will the PHE and the non permanent enhance within the FMAP stay in place?
- Will Congress contemplate proposals to undertake extra fiscal reduction or a everlasting counter-cyclical adjustment or tackle Medicaid financing within the territories?
Lengthy-Time period Companies and Helps
Medicaid is a big supply of protection for seniors and other people with disabilities, together with those that want long-term providers and helps (LTSS). Most eligibility pathways primarily based on previous age or incapacity, and practically all house and community-based providers (HCBS), are optionally available for states, creating state variation. The COVID-19 public well being disaster has highlighted the importance of Medicaid protection for individuals with disabilities by means of the ACA growth in addition to optionally available eligibility pathways primarily based on previous age or incapacity and optionally available HCBS profit packages, as these populations have been hit notably exhausting by the pandemic. Many seniors and other people with disabilities depend on Medicaid LTSS to fulfill day by day self-care and unbiased dwelling wants, which has taken on even larger consequence in the course of the pandemic. On the similar time, state finances shortfalls may make it difficult for states to take care of optionally available LTSS.
President-elect Biden helps legislative adjustments to extend federal Medicaid funding for and develop entry to HCBS. Extra broadly, Congress may contemplate proposals to get rid of Medicaid’s historic institutional bias by making HCBS a compulsory profit. Federal and state policymakers are also anticipated to proceed specializing in nursing house oversight, together with compliance with federal Medicaid and Medicare an infection management and different care high quality measures because the pandemic continues. As states rollout their vaccine precedence plans, extra consideration will give attention to reaching LTSS customers and workers past nursing amenities, together with individuals receiving and delivering HCBS.
What to Watch
- What actions will states proceed to take to handle the pandemic’s disproportionate influence on seniors and other people with disabilities, and can any of those coverage adjustments proceed after the PHE ends?
- Will Congress contemplate laws to develop protection and financing for Medicaid community-based LTSS?
Social Determinants of Well being
Social determinants of well being (SDOH) are the circumstances by which persons are born, develop, stay, work, and age that form well being. Addressing SDOH is essential for bettering well being and decreasing longstanding disparities in well being and well being care. SDOH embrace however are usually not restricted to housing, meals, training, employment, wholesome behaviors, transportation, and private security. Throughout the well being care system, there are multi-payer federal and state initiatives in addition to Medicaid-specific initiatives targeted on addressing social wants. Though federal Medicaid guidelines prohibit expenditures for many non-medical providers, states have been growing methods to determine and tackle enrollee social wants each inside and out of doors of managed care. Medicaid managed care plans could use administrative financial savings or state funds to supply a few of these providers. CMS launched extra steerage for states about alternatives to make use of Medicaid and CHIP to handle SDOH on January 7. The pandemic has exacerbated the challenges for state Medicaid packages associated to well being care entry and different SDOH and has shined a lightweight on persistent well being inequities because of the disparate influence of COVID-19 on individuals of coloration. Entry to meals and housing are areas of rising want as many individuals have misplaced jobs and revenue.
What to Watch:
- How can Medicaid be leveraged to assist tackle SDOH in the course of the pandemic and past?
- How will efforts be applied (e.g. by means of managed care, waivers, and so forth.)?
- How will efforts have an effect on well being and well being disparities?