After a lot anticipation, the Facilities for Medicare & Medicaid Providers (CMS) has introduced that Medicare will cowl the brand new Alzheimer’s drug, Aduhelm, topic to proof growth. This preliminary Nationwide Protection Dedication (NCD) comes after months of handwringing over the potential influence of this new high-priced drug on Medicare spending and a considerable Medicare Half B premium improve that took impact in January 2022. CMS proposes to cowl Aduhelm and comparable FDA-approved antiamyloid monoclonal antibody remedies underneath Protection with Proof Growth (CED) for sufferers collaborating in CMS-approved or NIH-supported randomized scientific trials, which can assist to generate the proof that CMS suggests is at the moment missing relating to whether or not Aduhelm is affordable and essential for the therapy of Alzheimer’s illness.
Whereas this resolution, which will likely be finalized in April 2022, proposes the phrases of Medicare protection of those remedies for Alzheimer’s illness, the Aduhelm story shouldn’t be prone to finish right here. Solely someday earlier than the preliminary NCD was issued, HHS Secretary Becerra directed CMS to reassess the month-to-month Medicare Half B premium for 2022 in gentle of the announcement from Biogen, the drug’s producer, that it was slashing the value of Aduhelm by 50% from $56,000 to $28,200 in response to anemic demand for the brand new drug.
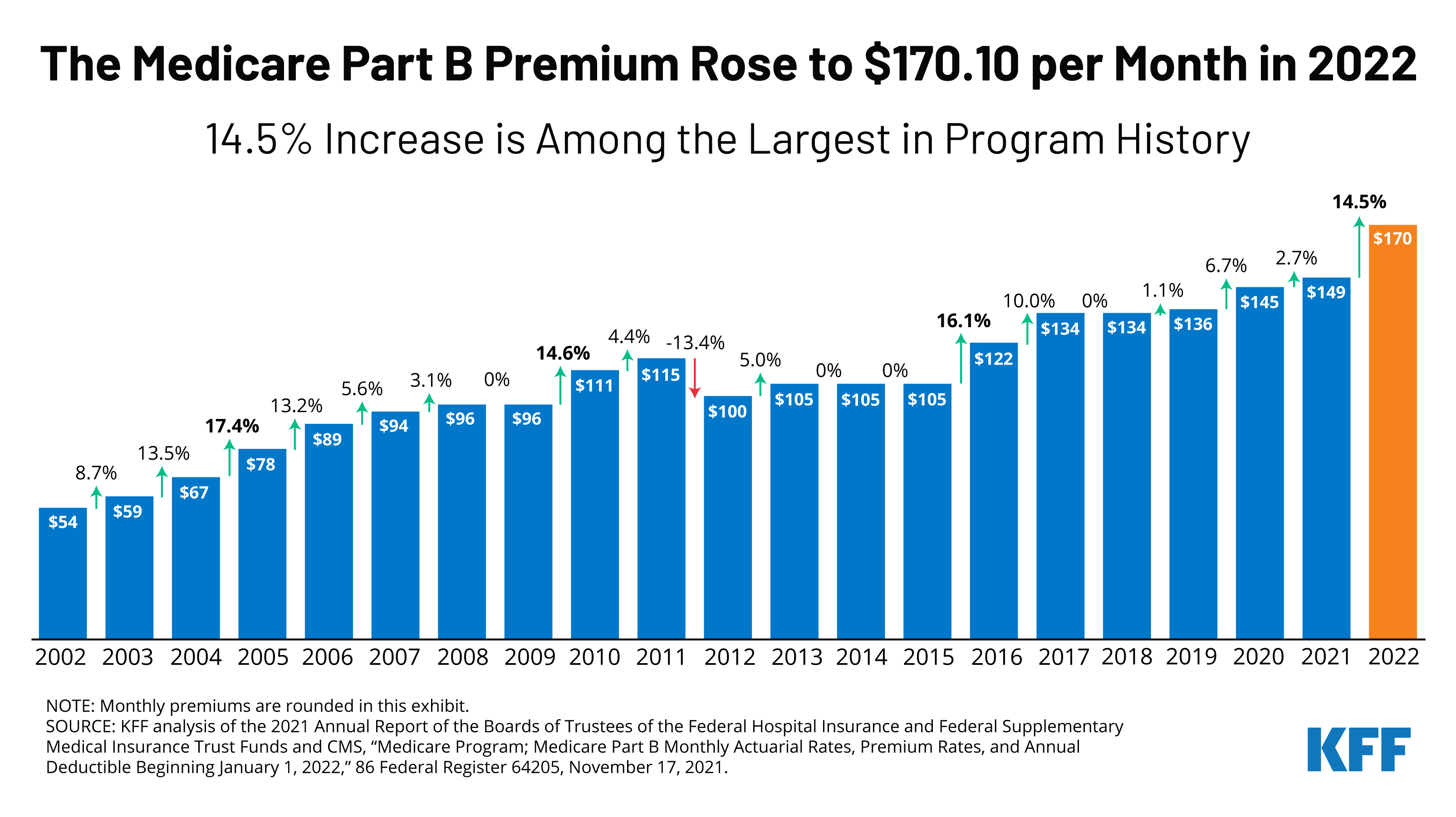
Again in November 2021, previous to the discharge of the preliminary nationwide protection willpower and the drop within the value of Aduhelm, CMS introduced a 14.5% hike within the Medicare Half B premium for 2022. The rise within the premium – from $148.50 in 2021 to $170.10 in 2022 – was based mostly on a “high-cost” situation that took under consideration the potential improve in Medicare Half B spending for Aduhelm, amongst different elements (Determine 1). CMS attributed about half of the premium improve to the necessity to enhance revenues to cowl larger projected Half B spending for this one drug alone.
Whereas solely a small fraction of Medicare beneficiaries are doubtless to make use of the drug, all however the very lowest earnings Medicare beneficiaries can pay the upper Medicare Half B premium this yr. For a lot of beneficiaries, the Half B premium shouldn’t be a trivial share of earnings. For instance, a senior dwelling on an earnings at 175% of the federal poverty degree (~$23,000 for a person) will spend practically 9% of her earnings this yr on the Half B premium alone, earlier than factoring in different bills, like Half D drug plan premiums or value sharing for Medicare lined providers. And for low-income Medicare beneficiaries who’ve protection from each Medicare and Medicaid, the Half B premium improve could have implications for Medicaid spending as a result of Medicaid pays their Medicare premiums.
CMS is now contemplating a potential adjustment within the 2022 Medicare Half B premium, a change which might be unprecedented – with the Half B premium already decided for the yr and being deducted from Social Safety funds – however maybe not unwarranted on this case. But even when CMS rolls again a portion of the Half B premium for 2022, Medicare beneficiaries who use Aduhelm may nonetheless be on the hook for the Half B coinsurance, which is 20% of the drug’s whole value, or greater than $5,000. Whereas most beneficiaries have supplemental protection to assist them pay their Medicare cost-sharing necessities, many don’t. This group consists of practically 6 million beneficiaries with no supplemental protection and a lot of the 26 million enrollees in Medicare Benefit plans, which generally cost the identical 20% coinsurance price that beneficiaries in conventional Medicare face for Half B medication (although out-of-pocket prices for Medicare Benefit enrollees can be restricted to their plan’s out-of-pocket most, which averaged $5,091 for in-network providers and $9,208 for each in-network and out-of-network providers (in PPOs) in 2021).
When it comes to Medicare spending, it seems that Medicare won’t expertise as massive a rise in Half B spending related to Aduhelm as was initially forecast and that CMS projected when setting the Half B premium for 2022, based mostly on the drug’s preliminary excessive value and comparatively excessive anticipated utilization. For instance, in the summertime of 2021, simply after the FDA authorised aducanumab, we estimated that the drug’s preliminary price ticket of $56,000 may enhance annual Medicare spending by roughly $30 billion if utilized by 500,000 Medicare beneficiaries. Contemplating the discount within the value of Aduhelm and the chance of decrease utilization based mostly on the preliminary NCD, it’s doubtless that Medicare spending on this drug will likely be considerably decrease, no less than within the close to time period.
Along with Medicare, the Aduhelm protection resolution may have implications for Medicaid. Whereas Medicaid should cowl FDA-approved medication underneath the Medicaid Rebate program, states could possibly impose medical necessity standards in addition to strict prior authorization necessities based mostly on the Medicare protection willpower limiting utilization. The magnitude of the monetary implications for Medicaid may hinge on additional protection steering from CMS.
It’s not arduous to think about a future situation the place a mix of a high-priced drug and excessive utilization really do generate billions of {dollars} in extra Medicare spending yearly and contribute to sizable will increase in Medicare premiums. On condition that Medicare has no authority underneath present regulation to decrease drug costs or restrict drug value development, this raises the stakes for ongoing coverage discussions round prescription drug value proposals within the Construct Again Higher Act. These proposals embrace permitting the federal authorities to barter the value of sure high-cost medication, requiring drug firms to pay rebates if drug costs rise quicker than the speed of inflation, and capping out-of-pocket prices underneath Medicare Half D. Whereas these proposals may end in a really modest discount within the variety of new medication coming to market within the U.S. over the subsequent few a long time, in keeping with CBO, and wouldn’t have an effect on spending related to Aduhelm, they may present significant financial savings on different high-cost medication down the highway.