As of February 2021, 12 states haven’t adopted the Inexpensive Care Act (ACA) provision to develop Medicaid to adults with incomes via 138% of poverty. Thousands and thousands of individuals in these states stay with out an inexpensive protection possibility. At present, the federal authorities covers 90% of the price of Medicaid protection for adults coated via the ACA enlargement, the next share than it does for different Medicaid enrollees. The Home Vitality and Commerce Committee reconciliation proposal as a part of the COVID reduction package deal goals to encourage non-expansion states to take up the enlargement by offering a further momentary fiscal incentive for states to newly implement the ACA Medicaid enlargement. This temporary gives illustrative estimates of the web fiscal profit to states from these incentives relative to state prices beneath the enlargement. We evaluation the strategies underlying these estimates within the Strategies part on the finish of the temporary.
How Does the Fiscal Incentive Work?
Below the proposal, states would obtain the 90% ACA match for the enlargement inhabitants. Below the ACA, states presently obtain a 90% federal matching price (FMAP) for adults coated via the ACA enlargement (this quantity was 100% in 2014 and phased all the way down to 90% over time). In states that haven’t expanded to this point, adults who could possibly be coated beneath enlargement embrace about 4 million uninsured folks (2.2 million with incomes beneath poverty within the “protection hole” and 1.8 million presently eligible for market protection as a result of their incomes are between 100% and 138% of poverty stage). As well as, people with incomes 100-138% of the federal poverty stage (FPL) who’re presently enrolled in market protection would change into eligible for Medicaid.
Below the proposal, states that shouldn’t have enlargement in place when the invoice is enacted can be eligible for a 5 share level enhance within the state’s common, or conventional, match price (FMAP) for 2 years in the event that they implement the enlargement. The normal FMAP applies to most providers for non-expansion teams, together with kids, non-expansion adults, seniors, and other people with disabilities. Even in states which have already adopted the enlargement, the standard Medicaid program is way bigger – representing 79% of Medicaid spending general in these states – and per enrollee prices are comparatively increased than the enlargement group. So, beneath this new incentive, states may draw down further funds for a big share of their Medicaid inhabitants and spending in the event that they newly develop. Along with the 12 states that haven’t adopted the enlargement, the rise within the match price may additionally apply to Missouri and Oklahoma if the invoice is enacted earlier than they implement the enlargement (these states are anticipated to implement in July 2021). Additional, if states newly undertake the enlargement within the close to time period, the brand new 5 share level enhance can be along with the present 6.2 share level enhance within the match price supplied beneath the Households First Coronavirus Response Act (FFCRA) that’s tied to the Public Well being Emergency (PHE). Based mostly on a January 2021 letter from the Biden Administration to Governors, the 6.2 share level enhance within the match can be in place a minimum of via March 2022, midway via federal FY 2023. Whereas the improved match can be in place for 2 years after a state implements the Medicaid enlargement, states can benefit from this new possibility any time within the subsequent ten years.
What Is the Estimated Impact on State Spending?
We estimate that the rise within the conventional match price would greater than offset the elevated state prices of the enlargement in each state. Nationally, the rise in federal help from the 5 share level enhance within the conventional match price to the 12 non-expansion states may whole $16.4 billion over two years if all states applied the enlargement beginning in FY 2022. These new federal funds to states can be offset by new state prices tied to the ten% share of enlargement. We estimate that new state prices for enlargement could possibly be $6.8 billion over two years throughout present non-expansion states, assuming all eligible folks enroll. The outcome can be an estimated fiscal profit to states of $9.6 billion over the 2 yr interval (Determine 1). Put one other approach, new federal funds beneath the 5 share level bump are greater than two instances bigger than new state enlargement prices; this ratio varies barely throughout states, from a couple of a half instances bigger in Texas to over 4 instances bigger in South Carolina (Desk 1).
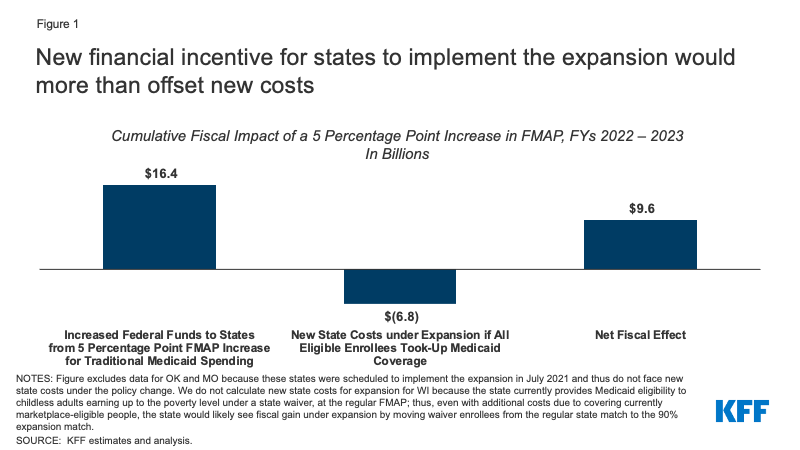
Determine 1: New Monetary Incentive for States To Implement the Enlargement Would Extra Than Offset New Prices
After the 2 years, states would proceed to obtain the 90% match for the enlargement group and the standard match with out the 5 share level enhance for the standard inhabitants. These estimates don’t embrace further federal funds that states would draw down via the 90% federal match on enlargement spending, which might proceed so long as the enlargement is in place. States would proceed to fund the ten% share of enlargement and would lose the added fiscal incentive after two years. Analysis reveals there are sometimes financial savings in different state packages associated to increasing Medicaid in addition to income will increase because of the infusion of federal funds related to the 90% match on enlargement spending. As well as, states may fund these ongoing prices with funds from the momentary enhanced FMAP that exceeded the price of enlargement; nonetheless, as states usually steadiness their budgets yearly and will use the extra funds for different functions, making use of these funds to a later yr could also be tough in observe.
These are illustrative estimates and topic to uncertainty. For instance, the estimate of elevated federal help from the improved match price could possibly be low if conventional Medicaid enrollment grows quicker than our estimates assume, which can be doable given the pandemic and financial results. As well as, the estimates of prices for brand spanking new protection could possibly be excessive as we don’t mannequin take up however relatively estimate prices for all eligible folks; alternatively, the estimate for enlargement could possibly be low as it’s primarily based on nationwide survey knowledge that usually undercounts decrease earnings folks. Even with some uncertainty within the estimates, the magnitude clearly reveals that the federal help would considerably outweigh the brand new prices of enlargement whereas the momentary enlargement incentive is in place. These estimates usually are not corresponding to estimates from the Congressional Funds Workplace (CBO) which might be capturing modifications in federal spending over the subsequent 10 years and incorporating behavioral responses that assume not all states would undertake the brand new possibility. The CBO estimates account for elevated federal spending and lowered prices for federal subsidies within the Market for states that undertake the enlargement. CBO assumes that the choice may enhance federal spending by a web of $15.5 billion over the 2021-2030 interval.
Medicaid enlargement within the remaining 12 non-expansion states has the potential to succeed in tens of millions of individuals. A complete literature evaluation of Medicaid enlargement research reveals that enlargement helps to develop protection and scale back the uninsured, enhance entry to and utilization of care, scale back uncompensated care prices, enhance affordability of care and scale back racial and ethnic disparities in protection. The proposed provisions would additionally present substantial fiscal incentives for states to develop, which could possibly be engaging given latest state income declines. Nonetheless, provided that the enlargement incentive can be momentary, its impact could also be restricted.
| Elevated Federal Funds from FMAP Improve on Conventional Populations | New State Value Because of ACA Medicaid Enlargement | Internet Impact for State Spending | |
| Whole* | $16,410 | -$6,830 | $9,590 |
| Alabama | 740 | -200 | 540 |
| Florida | 3,080 | -1,260 | 1,810 |
| Georgia | 1,360 | -640 | 710 |
| Kansas | 450 | -210 | 250 |
| Mississippi | 690 | -290 | 400 |
| North Carolina | 1,700 | -490 | 1,210 |
| South Carolina | 790 | -190 | 600 |
| South Dakota | 110 | -50 | 60 |
| Tennessee | 1,260 | -360 | 900 |
| Texas | 5,020 | -3,090 | 1,930 |
| Wisconsin** | 1,140 | ** | 1,140 |
| Wyoming | 70 | -40 | 30 |
| Adopted Enlargement however Not Carried out | |||
| Missouri* | 1,150 | * | 1,150 |
| Oklahoma* | 520 | * | 520 |
| NOTES: Figures might not sum to whole attributable to rounding. *Whole excludes OK and MO as a result of these states had been scheduled to implement the enlargement in July 2021 and thus don’t face new state prices beneath the coverage change. **We don’t calculate new state prices for enlargement for WI as a result of the state presently gives Medicaid eligibility to childless adults incomes as much as the poverty stage beneath a state waiver, on the common FMAP; thus, even with further prices attributable to protecting presently marketplace-eligible folks, the state would probably see fiscal achieve beneath enlargement by shifting waiver enrollees from the common state match to the 90% enlargement match. SOURCE: KFF estimates and evaluation. |
|||