On August 31, the Facilities for Medicare & Medicaid Providers (CMS) launched a proposed rule designed to make it simpler for individuals to acquire and preserve protection in Medicaid. Among the many many modifications in that rule are a number of main modifications to the eligibility course of for individuals with Medicare who’re additionally eligible for assist from Medicaid. CMS proposes to higher combine Medicaid purposes with eligibility and enrollment information primarily based on Medicare Half D Low-Earnings Subsidies (LIS) for pharmaceuticals. The proposed rule would additionally routinely enroll some individuals in Medicare Financial savings Applications the place Medicaid pays their Medicare premiums and, in lots of instances, value sharing, for individuals with restricted monetary sources.
On this challenge temporary, we estimate charges of Medicaid protection loss amongst individuals who turned Medicare-Medicaid enrollees (MMEs) throughout 2018 however didn’t have any months of MME protection within the prior 12 months. We examine outcomes for partial-benefit MMEs and full-benefit MMEs. For partial-benefit enrollees, Medicaid pays Medicare premiums and, in lots of instances, additionally pays Medicare’s deductibles and value sharing on behalf of MMEs. Full-benefit MMEs additionally obtain the complete vary of Medicaid advantages that aren’t lined by Medicare, corresponding to long-term providers and helps and non-emergency medical transportation. Amongst full-benefit MMEs, we outlined lack of protection as shedding full Medicaid advantages. In 2018, there have been 12.0 million MMEs within the 50 states and D.C., together with 10.0 million within the 39 states included on this evaluation. Of these 10 million, we included 1.1 million newly-enrolled MMEs (848,000 full-benefit and 294,000 partial-benefit) within the evaluation. See strategies for additional particulars on the examine inhabitants and outcomes of curiosity.
Our evaluation finds that 38% of newly-enrolled full-benefit MMEs in 2018 misplaced protection inside their first 12 months of enrollment and 31% misplaced protection for greater than 3 months, which is in keeping with, however considerably greater than, what an older examine had discovered. Amongst newly-enrolled partial profit MMEs, 33% misplaced protection for a number of months and 24% misplaced protection for greater than 3 months. Such substantive charges of Medicaid protection loss amongst Medicare beneficiaries are notable as a result of many Medicare beneficiaries dwell on mounted incomes and are unlikely to expertise will increase in earnings or belongings that might set off shedding eligibility for Medicaid. As an alternative, the lack of Medicaid seemingly displays administrative burdens related to verifying candidates’ eligibility and renewing their enrollment. The proposed rule goals to scale back Medicaid protection loss by decreasing these burdens.
How Does the Proposed Rule Simplify Eligibility and Enrollment Processes for Medicare-Medicaid Enrollees?
The Medicaid proposed rule addresses a number of elements that contribute to excessive charges of Medicaid protection loss amongst Medicare enrollees. The proposed rule would simplify the eligibility course of for MMEs. These modifications are meant to extend enrollment amongst Medicare beneficiaries who’ve by no means enrolled in Medicaid and to scale back the variety of Medicaid enrollees who lose protection just a few months after enrolling on account of administrative limitations. Particularly, the rule would:
- Encourage states to make use of the LIS definitions of economic sources in order that the monetary useful resource documentation Medicare beneficiaries full for LIS would additionally doc eligibility for Medicaid,
- Require states with definitions of economic sources that differ from LIS to simply accept candidates’ self-reported worth of sources until the state already has info that’s inconsistent with that worth, and
- Require states to help candidates with procuring acceptable documentation validating earnings and belongings when it’s required.
The rule additionally goals to scale back lack of Medicaid on the time of renewal. These modifications are meant to scale back the variety of Medicaid enrollees who’re nonetheless eligible however lose protection in the course of the renewal course of on account of administrative limitations. Particularly, the rule would:
- Require states to resume Medicaid solely as soon as per 12 months,
- Eradicate states’ choice to require an in-person interview as a part of the applying course of,
- Apply different simplified enrollment and renewal necessities that exist already for youngsters and different adults in Medicaid, and
- Institute necessities for the way states should reply when mail to an applicant or enrollee is returned.
CMS estimates that the modifications affecting MMEs would lead to an extra 1.5 million person-years of Medicaid enrollment, almost $7 billion in further Medicaid spending, and almost $3 billion in further Medicare spending within the 12 months 2027. Medicaid spending would improve as a result of Medicaid could be paying for added months of Medicare premiums and in some instances, Medicare value sharing and Medicaid advantages. Medicare spending is predicted to extend as a result of Medicaid protection of value sharing would lead MMEs to make use of extra Medicare-covered providers. As a result of the enrollment course of could be easier and there could be fewer renewals, the proposed rule would lower Medicaid administrative spending. (CMS estimates that administrative spending would lower by over $1 billion in 2027, however that features administrative financial savings from provisions that might have an effect on all Medicaid and CHIP enrollees along with the provisions affecting MMEs.)
What Do the Knowledge Present?
In describing the proposed modifications, CMS cited a examine that confirmed almost 30% of Medicare-Medicaid enrollees (MMEs) misplaced Medicaid for a least one month and over 20% misplaced protection for greater than 3 months within the 12 months after their preliminary enrollment month. That examine used Medicaid claims information from 2006 – 2010 and restricted the evaluation to full-benefit MMEs.
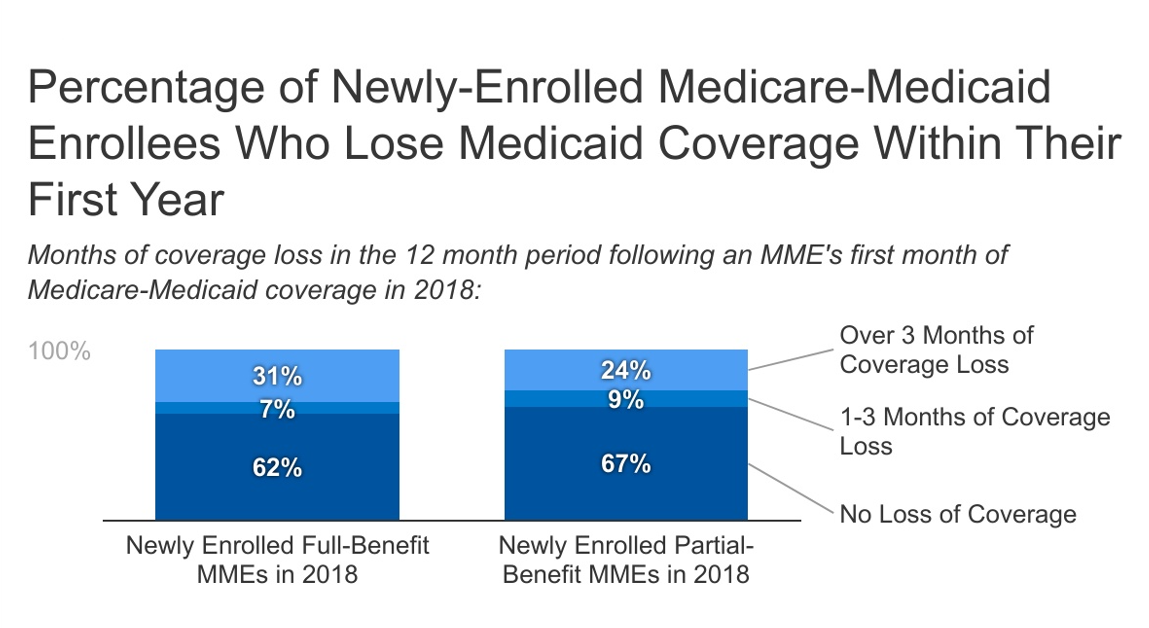
KFF finds that 38% of newly-enrolled full-benefit MMEs in 2018 misplaced no less than one month of protection throughout the 12 months after their first month of enrollment (Determine 1). The evaluation additionally finds that 31% misplaced over three months of protection. New partial-benefit MMEs in 2018 had barely decrease lack of protection than full-benefit MMEs, with 33% shedding no less than one month of protection throughout the 12 months after their first month of enrollment and 24% shedding over 3 months. Amongst these MMEs who misplaced protection throughout the first 12 months put up enrollment, the overwhelming majority misplaced protection for greater than 3 months. Individuals who lose Medicaid protection for greater than 3 months embrace some Medicare beneficiaries who misplaced Medicaid on the time of renewal in states that do multiple renewal interval per 12 months. There are additionally individuals shedding Medicaid earlier than the renewal interval which can counsel that people had been disenrolled because of post-enrollment eligibility verification. Publish-enrollment eligibility verification might require submission of detailed monetary information that enrollees have bother finding and could be prohibited usually underneath the proposed rule.
Protection loss within the 12 months after preliminary enrollment was extra frequent amongst newly-enrolled full-benefit MMEs underneath the age of 65 than amongst newly-enrolled full-benefit MME ages 65 and older: 46% misplaced protection for a number of months within the 12 months following their preliminary enrollment (Determine 2). In distinction, protection loss was decrease amongst full-benefit MMEs 65 and older: 32% misplaced protection for a number of months. Protection loss was decrease amongst all partial-benefit MMEs of all ages – 36% of these underneath 65 and 32% of these ages 65 and older misplaced protection for no less than one month.
Among the many 38% of newly enrolled full-benefit MMEs who misplaced Medicaid, 79% misplaced all Medicaid protection for no less than one month throughout their 12-month follow-up interval, together with protection of Medicare premiums and cost-sharing, and different Medicaid advantages (Determine 3). These Medicare beneficiaries would have needed to begin paying Medicare premiums and if relevant, cost-sharing. The remaining 21% misplaced eligibility for full Medicaid however retained Medicaid protection of Medicare premiums and value sharing (if relevant). All MMEs who lose protection now not have protection of Medicaid advantages, which embrace long-term helps and providers and nonemergency medical transportation amongst different providers and could also be significantly necessary for people who find themselves aged or with disabilities. In some states, Medicaid advantages embrace dental, imaginative and prescient, and listening to – providers that are necessary to Medicare beneficiaries however not lined by Medicare.
Trying Forward
Our evaluation reveals that roughly one-third of MMEs lose Medicaid within the 12 months following their first month of enrollment, which is surprising given most MMEs live on mounted incomes and unlikely to expertise modifications in eligibility. These findings spotlight the challenges individuals face when attempting to entry Medicaid and the way the brand new proposed rule may assist individuals extra simply navigate the applying and eligibility renewal processes. Additionally they construct on the findings of older analysis that CMS cited as a foundation for the proposed modifications. This evaluation doesn’t discover how many individuals shedding protection re-enroll in Medicaid, whether or not charges of Medicaid protection loss differ for MMEs who usually are not new to this system, and the way the proposed rule would affect Medicare beneficiaries who’re eligible for Medicaid however not enrolled. Understanding these points shall be useful to higher perceive the potential results of the proposed rule. Lastly, it’s unclear if modifications within the proposed rule will intersect with the unwinding of the Public Well being Emergency (PHE) as a result of the timing of each are unsure. When the PHE ends, states might want to conduct redeterminations and renewals for all enrollees for the primary time in over two years, which can lead to important disenrollment and churn.
| Knowledge: We used month-to-month enrollment and eligibility info from the 2017-2019 Reworked Medicaid Statistical Info System (T-MSIS) Analytic Information (TAF) Analysis Identifiable Information (RIF) DE Base information, linking the years with the beneficiary ID.
Figuring out Newly Enrolled Full-Profit and Partial Profit MMEs: We recognized MMEs utilizing the month-to-month twin eligibility code however used the month-to-month restricted advantages code to find out which MMEs had been eligible for full advantages (codes 1,A,D,4,5,7) or had been solely eligible for partial advantages (2,3,C,6,E,F). The twin eligibility code signifies full and partial profit standing for some varieties of MMEs, however for different varieties (corresponding to Certified People) it doesn’t. We outlined newly enrolled full-benefit MMEs as individuals who had been full-benefit MMEs for no less than one month in 2018 and weren’t full MMEs for the 12-month interval prior. We outlined newly enrolled partial-benefit MMEs as individuals who had been partial-benefit MMEs for no less than one month throughout 2018 and weren’t MMEs for the 12-month interval prior. Enrollee and State Exclusion Standards: We calculated the nationwide distinction between our charges and the ASPE charges of protection loss for full-benefit enrollees (10 share factors) and doubled that distinction to create a variety of “anticipated distinction” on the state-level. We excluded states that that had been both greater than 30 share factors away from ASPE’s charges or greater than 10 share factors decrease. We eradicated 9 states primarily based on these standards (DE, GA, IN, KS, ME, MI, MN, OH, and RI). We additionally excluded one state that reported no duals in 2017-2018 (AR), two states that reported solely partial duals in 2017-2018 (MS, ND). Defining Protection Loss: We estimated enrollment outcomes for 12 months after the unique enrollment month, for a complete of 13 months follow-up. In every month, we assigned MME’s profit standing as “full,” “partial,” or “none” after which summed the variety of months by profit standing. For partial-benefit MMEs, higher than zero months of no advantages indicated protection loss. For full-benefit MMEs, higher than zero months of no advantages or partial advantages indicated protection loss. We additionally break up protection loss amongst full-MMEs into protection loss with no Medicaid and protection loss with partial advantages, utilizing the variety of months of partial and no protection variable. Sensitivity Analyses: Sensitivity analyses included utilizing the twin eligibility code as a substitute of the month-to-month restricted advantages code to find out full vs. partial MME standing; utilizing a 12-month follow-up interval; and excluding MMEs who had been eligible via a medically-needy pathway (eligibility is set month-to-month for these enrollees). |
This work was supported partially by Arnold Ventures. KFF maintains full editorial management over all of its coverage evaluation, polling, and journalism actions.