Key Takeaways
The COVID-19 pandemic offered a public well being emergency that was unprecedented in its scope and period and introduced new focus to the long-standing unmet want for house and community-based companies (HCBS) amongst seniors and other people with disabilities and direct care workforce shortages. Recognizing Medicaid’s position as the first payer for HCBS, this challenge transient presents early findings from the newest KFF 50-state survey of Medicaid HCBS applications. It focuses on state insurance policies adopted in response to challenges posed by the pandemic, the pandemic’s influence on Medicaid HCBS enrollees and suppliers, and states’ early plans for the brand new American Rescue Plan Act (ARPA) 10 proportion level momentary improve in federal Medicaid matching funds for HCBS. We survey states about HCBS supplied by state plan authorities and waivers. There have been 277 HCBS waivers in FY 2018. General, 41 states responded to the survey by mid-July 2021, accounting for 87% of whole HCBS spending nationally in FY 2018, although response charges for particular questions diverse. We spotlight some particular state examples the place states supplied further info with their responses. Key discovering embody the next:
- Essential knowledge gaps stay, with just below half of responding states monitoring COVID-19 vaccination charges amongst Medicaid HCBS enrollees. On the identical time, state HCBS applications are taking part in a job in facilitating vaccine entry for HCBS enrollees, with most responding states adopting a number of insurance policies on this space. Over one-third of responding states have publicly accessible knowledge on COVID-19 circumstances and deaths amongst HCBS enrollees.
- The Medicaid HCBS supplier infrastructure declined in the course of the pandemic, with two-thirds of responding states reporting a everlasting closure of not less than one supplier. Most of those states reported everlasting closures amongst multiple HCBS supplier sort. States most often cited workforce shortages because the pandemic’s main influence on in-home and group house companies, whereas closures on account of social distancing measures was probably the most often reported main influence on grownup day well being and supported employment applications.
- Over half of responding states reported early plans for the brand new ARPA momentary enhanced federal funds for Medicaid HCBS. Probably the most often reported actions have been supplier fee fee will increase and workforce recruitment.
Increasing HCBS entry and strengthening the direct care workforce would assist to enhance care as pandemic restoration efforts proceed and past, whereas additionally rising public spending. Whereas the ARPA enhanced funds can be found just for one 12 months, further federal funding for HCBS is a part of the funds reconciliation package deal proposed by Democratic leaders, although the small print will likely be labored out by Congressional committees. President Biden earlier this 12 months proposed a $400 billion federal funding in Medicaid HCBS, although it’s unclear how a lot of that funding improve will likely be authorised by Congress because it considers competing priorities within the funds package deal.
Introduction
The COVID-19 pandemic offered a public well being emergency (PHE) that was unprecedented in its scope and period. Key Medicaid populations, together with seniors and nonelderly individuals with disabilities who use long-term companies and helps (LTSS), are disproportionately prone to critical sickness or demise from COVID-19 in comparison with the final inhabitants. This danger is heightened for individuals who obtain LTSS in congregate settings and for the direct care employees who present these companies. The pandemic’s influence on these populations introduced new focus to pre-existing points, together with unmet want for house and community-based companies (HCBS) and workforce shortages. Drawing on Medicaid’s position as the first payer for LTSS, together with HCBS, federal and state policymakers have adopted a lot of insurance policies to help pandemic response.
This challenge transient presents early findings from the newest KFF survey of Medicaid HCBS applications in all 50 states and the District of Columbia. It focuses on state insurance policies adopted in response to challenges posed by the pandemic, the pandemic’s influence on Medicaid HCBS enrollees and suppliers, and states’ preliminary plans for the brand new American Rescue Plan Act 10 proportion level momentary improve in federal Medicaid matching funds for HCBS accessible from April 2021 by March 2022. Further survey findings and state-level knowledge associated to Medicaid HCBS enrollment, spending, and key state insurance policies will likely be launched later. We survey states about HCBS supplied by state plan authorities and waivers. There have been 277 HCBS waivers in FY 2018. General, 41 states responded to the survey by mid-July 2021, although response charges for particular questions diverse. The 41 responding states account for 87% of whole HCBS spending nationally in FY 2018. We spotlight particular state examples the place states supplied further info with their responses.
COVID-19 Affect on Medicaid HCBS Enrollees
Over one-third of responding states reported having publicly accessible knowledge on COVID-19 circumstances and deaths amongst Medicaid HCBS enrollees. Although states are monitoring COVID-19 circumstances and deaths usually, and a few are monitoring general circumstances and deaths by demographic traits equivalent to age, race, and intercourse, fewer are amassing these knowledge particularly for Medicaid HCBS enrollees. Among the many 14 states reporting publicly accessible knowledge particular to HCBS enrollees, 12 states’ responses to this query diverse by waiver program. This implies that even when states are monitoring COVID-19 circumstances and deaths amongst HCBS enrollees, monitoring is probably not uniform throughout all HCBS applications. For instance, Illinois reported that it makes COVID-19 circumstances and deaths knowledge publicly accessible for 3 HCBS waivers serving individuals with mental and developmental disabilities (I/DD) however not for its HCBS waivers serving different populations. Rhode Island reported that efforts to trace COVID-19 circumstances and deaths amongst its HCBS waiver enrollees are underneath improvement, although knowledge aren’t but publicly accessible.
Slightly below half of responding states reported monitoring COVID-19 vaccination charges for Medicaid HCBS enrollees. Almost all of those states indicated that these knowledge are used internally to tell outreach efforts, whereas two states (Delaware and Indiana) famous that they make these knowledge publicly accessible. Seven states’ responses to this query diverse by HCBS program, once more suggesting that monitoring is probably not uniform throughout all HCBS enrollees. As well as, Washington reported that it’s starting to trace COVID-19 vaccination standing amongst its Part 1115 HCBS waiver enrollees as a part of the useful evaluation course of.
All responding states reported having not less than one coverage in place to facilitate entry to COVID-19 vaccines for Medicaid HCBS enrollees and suppliers, with 8 in 10 responding states reporting multiple coverage. Probably the most often reported coverage was partnering with public well being companies on vaccine outreach and training initiatives (Determine 1). For instance, West Virginia supplied a listing of homebound HCBS enrollees to native well being departments to rearrange for appointments to manage vaccines in enrollees’ houses. Different often reported insurance policies included leveraging Medicaid’s non-emergency transportation profit to offer enrollees with entry to vaccination appointments and enlisting HCBS suppliers in vaccine outreach and training efforts (Determine 1). Further insurance policies to facilitate vaccine entry reported by states included putting sure HCBS populations in increased vaccine entry precedence teams, having Medicaid managed care plans contact enrollees to offer training and schedule vaccination appointments, and partnering with pharmacies to offer vaccination clinics for HCBS enrollees. Washington reported having “strike groups” journey to some HCBS settings to supply vaccinations to employees and enrollees.
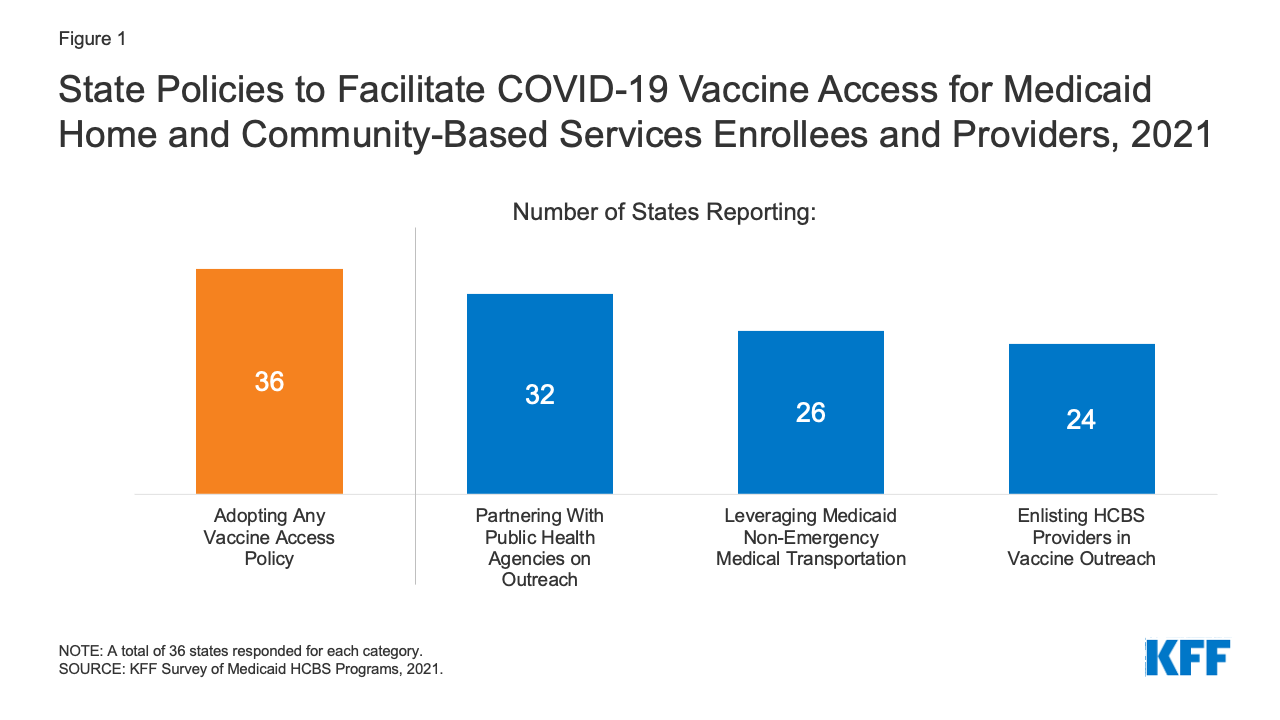
Determine 1: State Insurance policies to Facilitate COVID-19 Vaccine Entry for Medicaid Residence and Group-Primarily based Companies Enrollees and Suppliers, 2021
The pandemic affected all Medicaid HCBS settings, although the first influence recognized by states diverse considerably by setting sort. States most often reported that the pandemic resulted in workforce shortages for HCBS supplied in an enrollee’s house and in group houses, whereas closures on account of social distancing measures was probably the most often reported influence for grownup day well being applications and supported employment applications (Determine 2). For HCBS supplied in an enrollee’s house, workforce shortages was intently adopted by enrollees declining to have employees of their houses (Determine 2). States reported that some HCBS enrollees and their relations declined companies on account of concern of coronavirus publicity and had issues about receiving in-person companies till enrollees and suppliers could possibly be vaccinated. To attenuate service interruptions, some states reported utilizing Medicaid emergency authorities to offer HCBS by way of telehealth the place doable to enrollees at house and in grownup day well being applications. Some states additionally famous that utilization of supported employment companies dropped on account of job loss in the course of the pandemic among the many enrollees who acquired these companies.
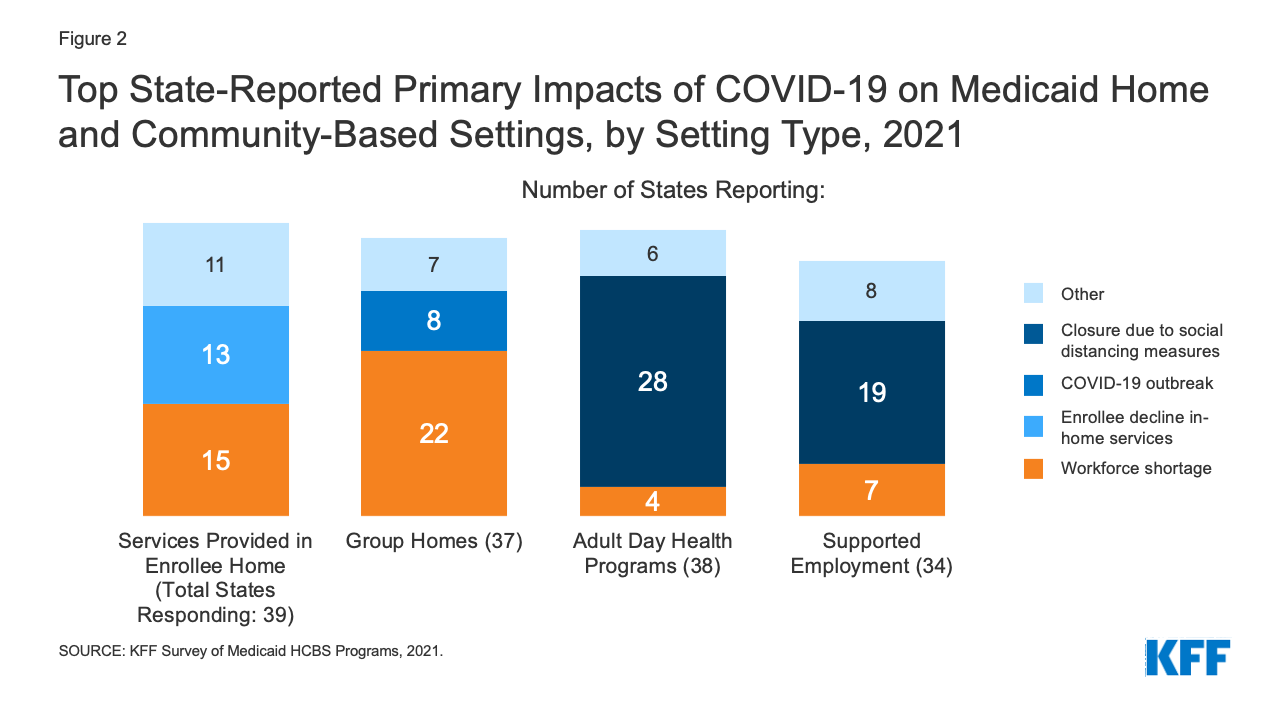
Determine 2: Prime State-Reported Major Impacts of COVID-19 on Medicaid Residence and Group-Primarily based Settings, by Setting Sort, 2021
Eight states recognized COVID-19 outbreaks because the pandemic’s main influence in group houses (Determine 2). (Different states additionally could have skilled outbreaks however didn’t establish them because the pandemic’s “main” influence on group houses of their survey response.) Arizona supplied further element in regards to the pandemic’s influence on group houses, noting that group houses needed to improve staffing to help HCBS enrollees in the course of the day when exterior day habilitation and supported employment applications turned much less accessible. As well as, Arizona famous that its group houses needed to establish various locations to quarantine residents uncovered to coronavirus to mitigate the chance of spreading an infection to different residents and employees.
COVID-19 Affect on Medicaid HCBS Suppliers
Two-thirds of responding states reported a everlasting closure of not less than one Medicaid HCBS supplier in the course of the pandemic (Determine 3). Most of those states (16) reported everlasting closures amongst multiple HCBS supplier sort. Grownup day well being applications have been probably the most often reported HCBS supplier sort to have completely closed, adopted by suppliers of in-home companies, supported employment suppliers, and group houses (Determine 3). A number of states indicated that workforce shortages already existed previous to pandemic and worsened in the course of the COVID-19 PHE. For instance, Oregon famous that HCBS suppliers skilled challenges with remaining financially viable because of the pandemic, which is able to influence their capability to reopen. Particular challenges cited by Oregon associated to suppliers’ capability to keep up leased house, retain educated employees, and supply supported employment companies equivalent to job search, placement, and training.
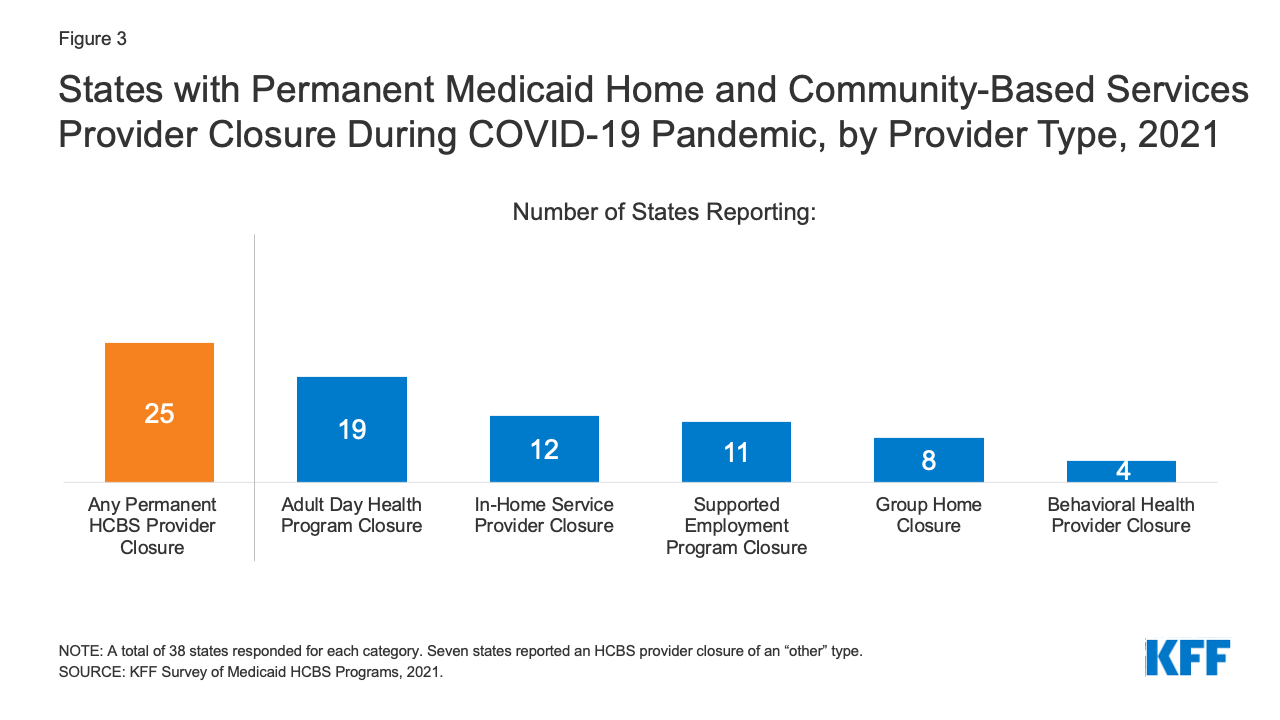
Determine 3: States with Everlasting Medicaid Residence and Group-Primarily based Companies Supplier Closure Throughout COVID-19 Pandemic, by Supplier Sort, 2021
About three-quarters of responding states reported that they used CMS-approved authority to offer retainer funds to financially help Medicaid HCBS suppliers in the course of the pandemic. Retainer funds enable suppliers to proceed to invoice and be paid for habilitation and private care companies which might be approved in enrollee service plans, which is meant to assist suppliers preserve capability when circumstances forestall enrollees from really receiving these companies. For instance, some HCBS suppliers equivalent to grownup day well being facilities needed to briefly near adjust to social distancing orders in the course of the COVID-19 PHE, and a few HCBS enrollees could have needed to briefly cease receiving in-home companies on account of self-quarantine.
Most responding states (20 of 29) reported that the preliminary federal restrict of three 30-day episodes for retainer funds was inadequate to completely help HCBS suppliers in the course of the pandemic. Some states’ responses to this query diverse by HCBS program, indicating that the federal retainer fee restrict could have been enough to help some service supplier varieties however not others. For instance, Pennsylvania reported the federal retainer fee restrict was inadequate for I/DD service suppliers however was enough for suppliers serving enrollees in its waiver for seniors and other people with bodily disabilities. CMS’s preliminary steering allowed states to make as much as three 30-day episodes of retainer funds in the course of the COVID-19 PHE. This steering was in impact after we started fielding our survey in March 2021. Subsequent CMS steering revised federal coverage to permit states to supply retainer funds for as much as three further 30-day durations in calendar 12 months 2021, recognizing the prolonged period of the COVID-19 PHE.
Early State Plans for ARPA HCBS Funding Enhance
Almost six in 10 responding states recognized the highest initiatives that they have been planning to focus on with the brand new momentary enhanced federal Medicaid matching funds for HCBS within the American Rescue Plan Act (ARPA). The ARPA will increase the federal matching fee for state spending on HCBS by 10 proportion factors from April 1, 2021 by March 31, 2022. States should preserve their present HCBS spending and use the improved funds for actions that develop or strengthen Medicaid HCBS. KFF beforehand estimated that this ARPA provision might improve federal Medicaid HCBS spending by about $11.4 billion nationally. The rise will likely be distributed proportional to the scale of state HCBS applications, reflecting variation in each state dimension and elective coverage decisions. The ARPA was enacted simply as our survey went into the sphere in March 2021, and survey responses replicate states’ early plans. States’ plans for the ARPA funds could change in gentle of CMS implementation steering issued in mid-Might 2021, and based mostly on stakeholder enter as states develop their formal plans to undergo CMS.
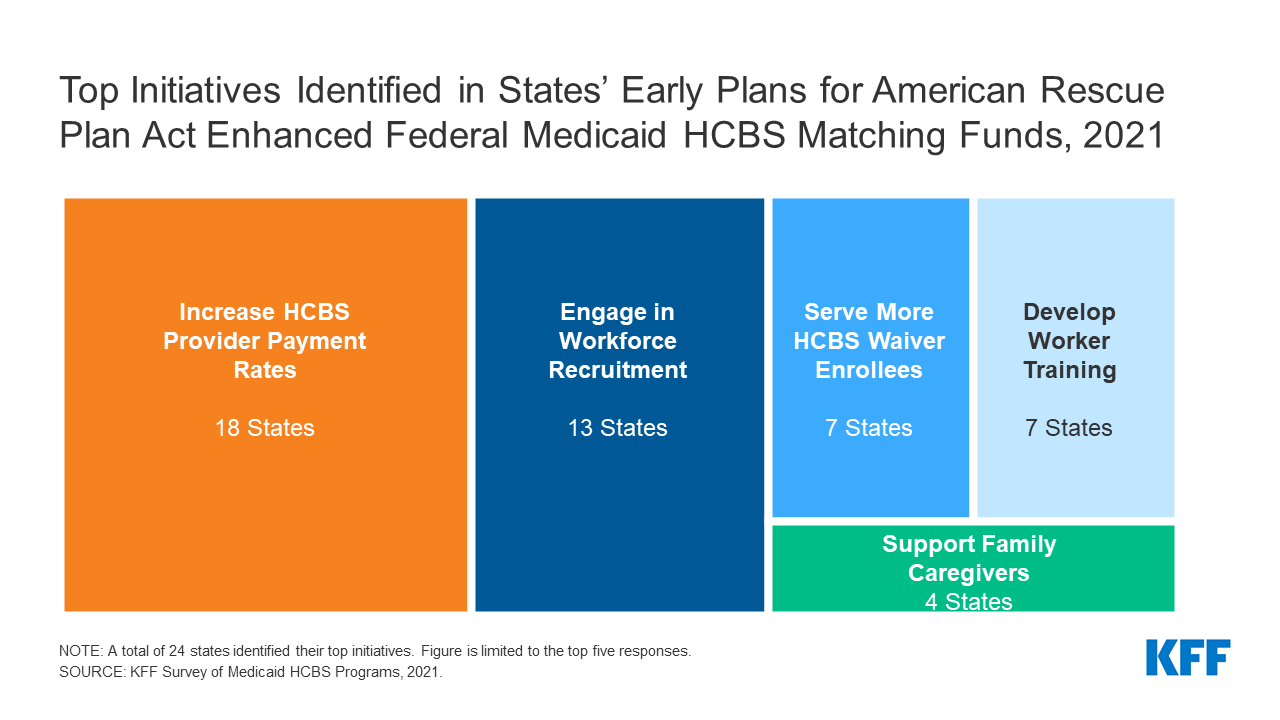
The 2 initiatives most often reported by states as potential makes use of of the brand new APRA funds have been rising HCBS supplier fee charges and workforce recruitment (Determine 4). Different initiatives rounding out the highest 5 included serving further HCBS waiver enrollees, investing in employee coaching, and supporting household caregivers (Determine 4). Fewer states reported offering emergency gear and provides (4 states), offering employee hazard or extra time pay (3 states), offering retainer funds (3 states), offering companies to mitigate enrollee isolation because of the pandemic (2 states), including or rising waiver companies (2 states), and funding nursing house to group transitions (2 states) amongst their prime anticipated makes use of of APRA funds. We requested states to establish their prime two initiatives, although a lot of states’ responses to this query diverse by HCBS program with 14 states reporting three or extra initiatives throughout completely different applications. The Might 2021 CMS steering clarified that states can also use ARPA funds to facilitate entry to COVID-19 vaccines, so some states could embody this initiative of their remaining plans.
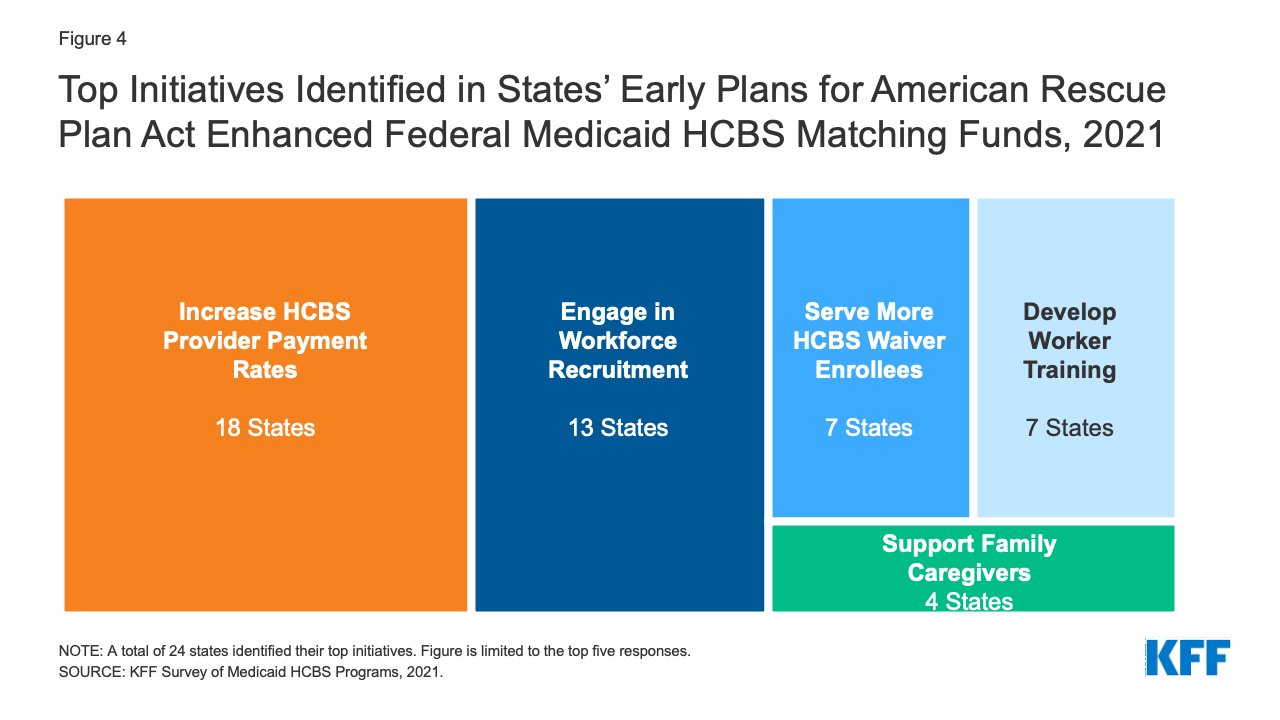
Determine 4: Prime Initiatives Recognized in States’ Early Plans for American Rescue Plan Act Enhanced Federal Medicaid HCBS Matching Funds, 2021
Trying Forward
Understanding the pandemic’s influence on Medicaid HCBS enrollees and suppliers might help to tell ongoing pandemic response and restoration efforts. Essential knowledge gaps stay, with most states missing publicly accessible knowledge on COVID-19 circumstances and deaths amongst HCBS enrollees. Whereas the provision of vaccines has led to substantial decreases in circumstances and deaths amongst these in LTSS settings, CMS has famous that ongoing vaccination efforts will likely be needed on account of workforce turnover and to make sure widespread vaccine entry. Our survey outcomes point out that whereas some states are monitoring vaccination charges amongst Medicaid HCBS enrollees, monitoring shouldn’t be but uniform throughout all states and amongst all HCBS applications inside states. A latest interim remaining rule adopting necessities for sure LTSS settings to report on, present training about, and provide the COVID-19 vaccine to residents and employees applies to nursing houses however deferred establishing comparable necessities for congregate community-based settings like group houses and grownup day well being facilities. Till knowledge, useful resource, and oversight gaps throughout the LTSS continuum are stuffed, nonelderly individuals with disabilities could proceed to expertise disproportionate obstacles to vaccine entry in comparison with individuals in nursing houses, and the complete influence of COVID-19 on this inhabitants won’t be understood fully. Regardless of restricted efforts to trace vaccination charges, our survey additionally discovered that state HCBS applications are taking part in a job in facilitating vaccine entry for HCBS enrollees, with most states adopting a number of insurance policies on this space. These efforts could possibly be expanded if states select to direct a portion of their ARPA enhanced HCBS funds to actions supporting COVID-19 vaccine entry as permitted in latest CMS steering.
The pandemic has introduced new consideration amongst policymakers and the general public to the longstanding unmet want for HCBS and direct care workforce scarcity, pushed by low wages, excessive turnover, and restricted alternatives for profession development. Most states reported workforce shortages because the pandemic’s main influence on HCBS supplied in an enrollee’s house and in group houses. Many states additionally reported everlasting closure of Medicaid HCBS suppliers in the course of the pandemic, affecting grownup day well being facilities, in-home service suppliers, supported employment suppliers, and group houses. Most states that reported supplier closures skilled the lack of multiple supplier sort. Although many states reported utilizing retainer fee authority to financially help suppliers, the unique federal episode restrict could have been inadequate to satisfy some suppliers’ wants, notably these with slim working margins. Medicaid suppliers additionally confronted challenges accessing federal supplier aid funds, each within the quantity of funding acquired and delays in allocations in comparison with different supplier varieties.
Sustaining and rising the HCBS supplier infrastructure is vital to assembly enrollee want and increasing entry to those companies as pandemic restoration efforts proceed and past. The APRA one-year enhanced funds for HCBS represents the primary new federal funding in Medicaid HCBS for the reason that Inexpensive Care Act in 2010. States have adopted a lot of insurance policies to develop entry to Medicaid HCBS in the course of the PHE, equivalent to increasing eligibility standards, streamlining enrollment processes, including companies, and rising supplier fee charges, however their capability to proceed many of those insurance policies after the PHE ends could also be restricted by budgetary constraints. Our survey discovered that states’ preliminary plans for the brand new ARPA funds centered on supplier fee fee will increase and workforce recruitment, two areas which expertise in the course of the pandemic has confirmed are essential to sustaining and increasing entry to HCBS. Whereas the ARPA enhanced funds can be found just for one 12 months, further federal funding for HCBS is a part of the funds reconciliation package deal proposed by Democratic leaders, although the small print will likely be labored out by Congressional committees. President Biden earlier this 12 months proposed a $400 billion federal funding in Medicaid HCBS, although it’s unclear how a lot of that funding improve will likely be authorised by Congress because it considers competing priorities within the funds package deal.