Part 1115 waiver exercise has been a key space of curiosity within the last weeks of the Trump Administration. Part 1115 authority permits the HHS Secretary to waive sure provisions of federal regulation in state Medicaid packages to check insurance policies which might be prone to promote program goals. These waivers usually replicate administration priorities, though the Secretary’s discretion will not be limitless. The incoming Biden Administration might rescind current waiver steerage (resembling steerage associated to work necessities and capped financing) and/or problem new steerage. It might additionally assessment provisions in presently accredited waivers and renewal requests and transfer to withdraw or not renew waivers that don’t promote program goals. Though CMS usually reserves the fitting to withdraw accredited waiver and/or expenditure authorities at any time, precedent for withdrawing accredited waivers is proscribed.
In its last days, the Trump Administration has accredited controversial waivers that had been pending (most not too long ago for Tennessee), prolonged different waivers greater than a 12 months earlier than expiration, and took steps to attempt to delay the method for withdrawing or amending accredited waivers. This problem transient takes a more in-depth have a look at this current exercise to grasp implications for the Biden Administration.
Tennessee Approval
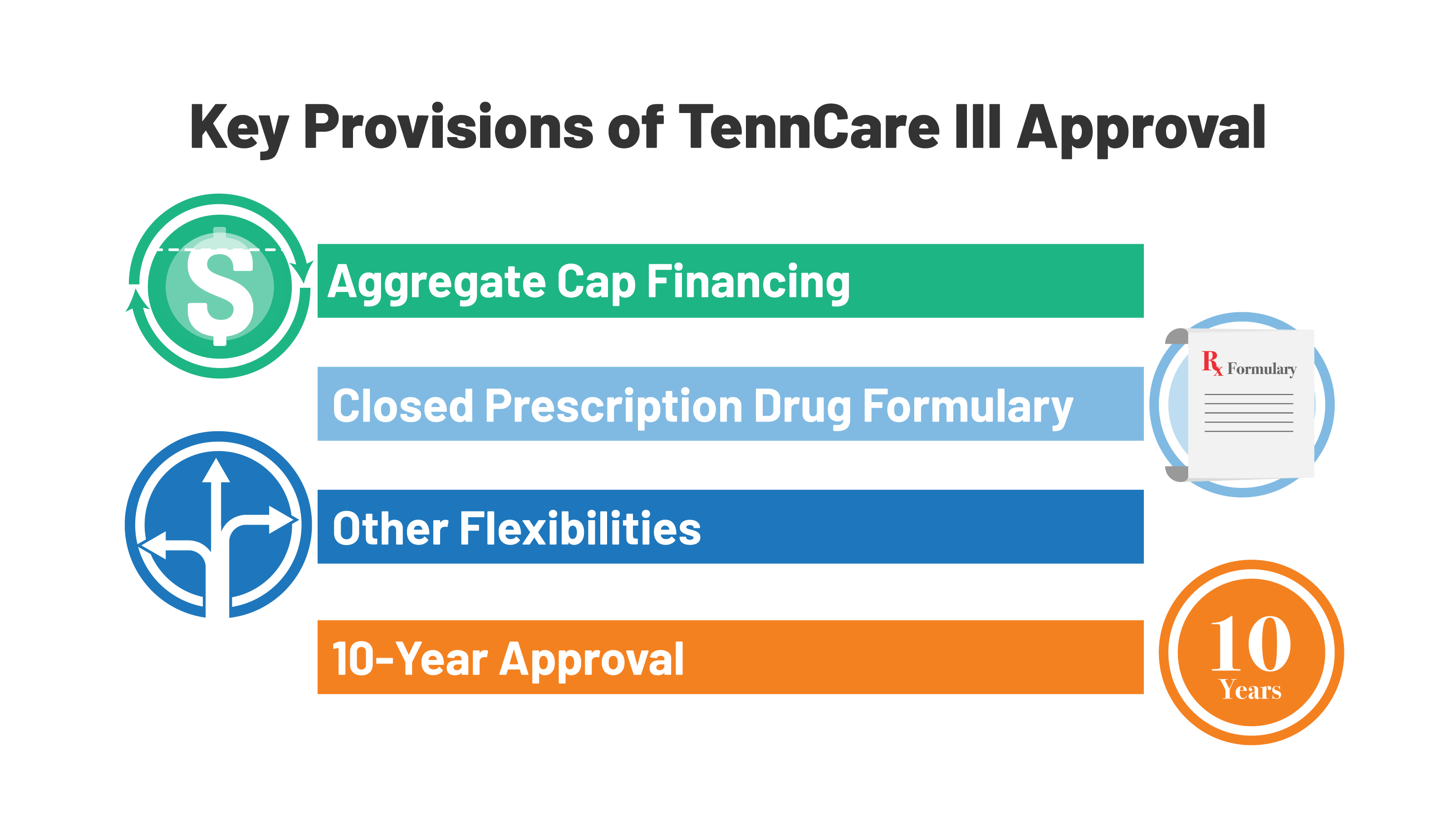
On January 8, 2021, CMS accredited a waiver request from Tennessee that might transition practically the entire state’s Medicaid program presently coated by its long-standing TennCare II waiver into a brand new TennCare III program. This waiver contains most TennCare enrollees, together with kids, dad and mom, and pregnant ladies in addition to many seniors and other people with disabilities. This advanced approval is especially important nationally as a result of provisions associated to financing, drug protection, and the length of the waiver (Determine 1). These elements make Tennessee’s waiver a primary candidate for assessment by the Biden Administration.

Determine 1: Key Provisions of TennCare III Approval
Financing: The TennCare III waiver units an mixture cap on federal spending and offers a chance for the state to maintain a portion of any federal financial savings (Determine 2). Each of those options differ from the best way Medicaid financing works beneath present regulation the place prices and financial savings are shared by the states and the federal authorities as a result of formulation that ensures federal matching {dollars} at a charge set in statute with no pre-set restrict. Whereas Part 1115 waivers have to be price range impartial to the federal authorities, that price range neutrality is usually decided on a per enrollee foundation fairly than an mixture foundation. Previously, capped demonstrations have been accredited in Rhode Island, Vermont, and Virginia (for a restricted inhabitants), however they’re now not in place in these states. CMS is specific that its approval of Tennessee’s waiver will not be part of the Trump Administration’s Wholesome Grownup Alternative (HAO) initiative, which permits for capped financing. The match charge is an space of Medicaid that is probably not modified beneath Part 1115 waiver authority. Key financing parts of TennCare III embrace:
- Setting the Cap. The combination cap could be adjusted annually to replicate the anticipated development in federal Medicaid spending within the President’s price range and adjusted for optimistic or unfavourable modifications in enrollment which might be better than one share level in magnitude.
- Spending Above the Cap. Usually, capped financing would pose fiscal dangers to states and will decrease a state’s efficient match charge as a result of any state spending above the cap wouldn’t obtain federal matching funds, as is the case with capped financing for Puerto Rico and the opposite Territories. Nevertheless, changes to Tennessee’s cap tied to the expansion charge for Medicaid within the President’s price range (which has traditionally been larger than inflation and better than the Tennessee’s historic development) and to elevated enrollment mitigate the danger of this capped financing mannequin to Tennessee. Whereas Tennessee should submit an modification to cut back the extent of advantages or coated populations beneath what was in place on the finish of 2020, the TennCare III approval doesn’t prohibit such modifications.
- Spending Under the Cap. If expenditures are beneath the cap in a given demonstration 12 months, Tennessee might entry as much as 55% of the federal share of financial savings to reinvest in state well being packages (together with these not eligible for Medicaid funding) if the state meets sure high quality metrics, along with retaining 100% of the financial savings the state would usually get beneath Medicaid matching formulation. Beneath this provision, Tennessee might see a larger efficient match charge than statutory ranges since this chance for shared financial savings permits the state to obtain extra federal Medicaid {dollars} with out extra state spending. Prior CMS steerage associated to the usage of federal Medicaid funds for non-Medicaid state packages has been combined. Steerage from 2017 famous that CMS would now not enable federal matching funds for designated state well being packages (DSHP); nonetheless, in its approval of TennCare III CMS defined that it might enable for federal funds for non-Medicaid state well being packages consistent with coverage ideas established in its Well being Grownup Alternative (HAO) steerage.

Determine 2: TennCare III makes use of an mixture cap financing construction that enables for changes and “shared financial savings” if spending is beneath the cap.
Closed Formulary: Beneath federal guidelines, in alternate for important rebates on prescribed drugs, state Medicaid packages should cowl practically all medicine accredited by the FDA, basically requiring an “open formulary” (not like non-public insurers, who can enter into negotiations with producers about whether or not or to not embrace medicine on the insurers’ formularies). The TennCare III approval would enable Tennessee to as a substitute cowl the better of both one drug per therapeutic class or the identical variety of medicine per class as a particular Important Well being Advantages benchmark plan within the Inexpensive Care Act alternate, with an exceptions course of for protection of non-formulary medicine. Tennessee might nonetheless gather statutory rebates for coated medicine. CMS beforehand rejected the same proposal in Massachusetts.
10-Yr Approval: In November 2017 steerage, CMS indicated it might take into account approving “routine, profitable, non-complex” Part 1115 extension requests for as much as 10 years. Since then, CMS has accredited 10-year waiver extensions for 3 non-family planning demonstrations (WI, ME, and IN). CMS accredited TennCare III for 10 years although it doesn’t seem to satisfy the situations within the 2017 steerage: it was accredited as a brand new waiver (not an extension), acquired 6,186 feedback (of which “the overwhelming majority” opposed the waiver), and incorporates advanced financing and provisions.
Different Key Waiver Points to Watch
Different current exercise beneath the Trump Administration might hamper the Biden Administration’s efforts to assessment sure waivers.
Expedited and Early Approval of Waivers. On January 15, 2020 CMS accredited a ten-year extension for the Texas Healthcare Transformation and High quality Enchancment Program (THTQIP) waiver following a “quick observe” extension course of which allowed the state to waive public discover and remark necessities (citing the immediacy of the COVID-19 public well being emergency). The THTQIP waiver had been set to run out on September 30, 2022. On the identical day, CMS renewed Florida’s Managed Medical Help waiver (which had been set to run out in June 2022) by June 2030. These renewals embrace provisions that the Biden Administration might assessment, together with uncompensated care swimming pools which offer funding for individuals who may very well be coated by the Medicaid enlargement. Early approvals of those requests beneath the Trump Administration might make it harder for the Biden Administration to switch or withdraw these provisions subsequently.
Course of to Withdraw Waiver Authorities. Outgoing CMS Administrator Seema Verma has inspired states to signal a “letter of settlement” that specifies that any future CMS dedication suspending, terminating, or withdrawing a waiver will need to have an efficient date no earlier than 9 months after the preliminary dedication. The letter additionally specifies timelines for hearings and a briefing schedule for states to problem these determinations. These agreements might make it harder for the Biden Administration to amend or withdraw waivers that it determines to be inconsistent with Medicaid program goals, relying upon how they’re construed. Congressional Democrats have famous that these “letters of settlement” battle with current laws that require CMS to ascertain such a course of as a part of every waiver’s phrases and situations and requested that CMS rescind them instantly.
Pending Litigation. The Supreme Courtroom is reviewing appeals courtroom choices setting apart work requirement waivers in Arkansas and New Hampshire, with the opening briefs filed by the Trump Administration and states on January 19, 2021. Though the Biden Administration is prone to rescind steerage associated to Medicaid work necessities and will transfer to withdraw different presently accredited work requirement waivers, a Supreme Courtroom ruling in favor of the HHS Secretary’s authority to approve work necessities might nonetheless go away these waivers open to future administrations.