In Medicaid, states are required to cowl all screening providers in addition to any providers “essential… to appropriate or ameliorate” a baby’s bodily or psychological well being situation beneath Medicaid’s Early and Periodic Screening, Diagnostic and Therapy (EPSDT) profit (see Field 1). Many of those screening providers together with immunizations are supplied at well-child visits. These visits are a key a part of complete preventive well being providers designed to maintain youngsters wholesome and to determine and deal with well being situations in a well timed method. Varied research have additionally proven that youngsters who forego their well-child visits have an elevated likelihood of going to the emergency room or being hospitalized. Effectively-child visits are beneficial yearly for youngsters ages three to 21 and a number of occasions a 12 months for youngsters beneath age three based on the Brilliant Futures/American Academy of Pediatrics (AAP) periodicity schedule.
A current Facilities for Medicare and Medicaid Companies (CMS) evaluation exhibits that half of youngsters beneath age 19 obtained a Medicaid or CHIP funded well-child go to in 2020. The onset of the pandemic in 2020 had a considerable impression on well being and well being care service utilization, however analysis has proven that many Medicaid-covered youngsters weren’t receiving beneficial screenings and providers even earlier than the pandemic. This subject transient examines well-child go to charges total and for chosen traits earlier than and after the pandemic started and discusses current state and federal coverage modifications that might impression youngsters’s preventive care. The evaluation makes use of Medicaid claims information which monitor the providers enrollees use and should differ from survey information. In future years, claims information will probably be used to observe adherence to beneficial screenings. Key findings embody:
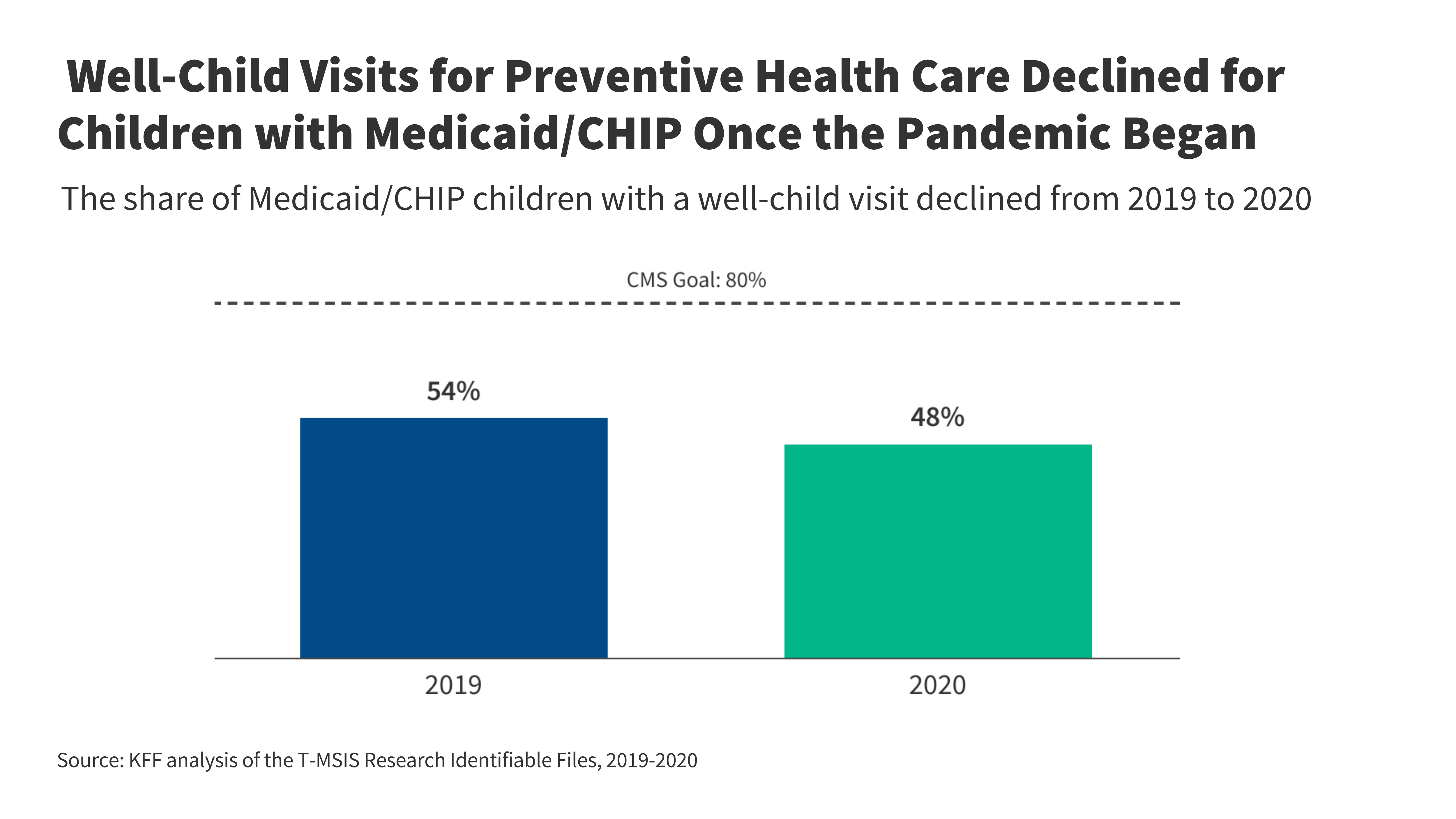
- Greater than half (54%) of youngsters beneath age 21 enrolled in Medicaid or CHIP obtained a well-child go to in 2019, however the share fell to 48% in 2020, the beginning of the COVID-19 pandemic.
- Regardless of having the very best well-child go to charges in comparison with different ethnic and racial teams, Hispanic and Asian youngsters enrolled in Medicaid or CHIP noticed the most important share level declines in well-child go to charges from 2019 to 2020.
- Youngsters over age three enrolled in Medicaid or CHIP have decrease charges of well-child visits and skilled bigger declines in well-child visits in the course of the pandemic than youngsters beneath age three.
- Effectively-child go to charges are decrease for Medicaid/CHIP youngsters in rural areas, however charges in city areas declined extra in the course of the pandemic.
| What’s the EPSDT profit?
Medicaid’s Early and Periodic Screening, Diagnostic and Therapy (EPSDT) profit offers a set of complete well being care providers to Medicaid enrollees beneath age 21. Beneath EPSDT, states are required to cowl all screening providers for youngsters in addition to any providers “essential… to appropriate or ameliorate” a baby’s bodily or psychological well being situation. States should present screenings for developmental and behavioral well being situations, in addition to for imaginative and prescient, listening to, and dental situations, on a periodic foundation that meets cheap requirements of medical apply. These providers should be supplied for youngsters, no matter whether or not a state chooses to cowl them for adults. What’s the aim of the EPSDT profit and why is it vital? The EPSDT profit goals to determine well being situations that may impede youngsters’s progress and improvement early and is essential in making certain low-income youngsters obtain the care they want. Whereas the EPSDT profit is vital to all youngsters, it has been particularly helpful for youngsters with particular well being care wants. By way of the EPSDT profit, Medicaid offers extra complete protection for these youngsters than the everyday personal insurance coverage plan and will increase entry to wanted providers that enhance the standard of every day life. Medicaid covers nearly half of all youngsters with particular well being care wants. As well as, EPSDT facilitates larger entry to take care of youngsters with behavioral well being wants, as youngsters identified with psychological or different behavioral well being situations should obtain any service out there beneath federal Medicaid legislation essential to handle the situation, even when the state doesn’t cowl the behavioral well being service for adults. |
How did use of well-child visits change in the course of the pandemic?
Greater than half (54%) of youngsters beneath 21 enrolled in Medicaid or CHIP obtained a well-child go to in 2019, however the share fell to 48% in 2020, the primary 12 months of the COVID-19 pandemic (Determine 1). Charges examined right here use Medicaid claims information which differ considerably from survey information (see Field 2). Whereas the overwhelming majority of youngsters within the evaluation (91% in 2019 and 88% in 2020) used a least one Medicaid service, together with preventive visits, sick visits, filling prescriptions, or hospital or emergency division visits, well-child go to charges remained low and are considerably beneath the CMS aim of no less than 80%. One current evaluation discovered that 4 in 10 youngsters enrolled in Medicaid or CHIP skilled no less than one problem when accessing well being care. Boundaries to Medicaid/CHIP youngsters receiving wanted care can embody lack of transportation, language limitations, disabilities, and fogeys having problem discovering childcare or taking break day for an appointment in addition to the provision of and distance to major care suppliers. Some states have seen a loss in Medicaid pediatric suppliers, and one current story reported that households with Medicaid in California have been touring lengthy distances and experiencing lengthy wait occasions for major care appointments. Information have additionally proven slight declines within the share of kindergarten youngsters updated on their routine vaccinations because the COVID-19 pandemic, which can, partially, be related to the decline in well-child visits. The nationwide measles, mumps, and rubella (MMR) vaccination price is beneath the aim of no less than 95%, and a few states are actually seeing measle outbreaks amongst youngsters.
Regardless of having the very best well-child go to charges in comparison with different ethnic and racial teams, Hispanic and Asian youngsters enrolled in Medicaid or CHIP noticed the most important share level declines in well-child go to charges from 2019 to 2020 (Determine 2). Previous to the pandemic in 2019, about half or extra of youngsters throughout most racial and ethnic teams had a well-child go to, with charges highest for Hispanic (60%) and Asian (57%) youngsters. The speed for American Indian and Alaska Native (AIAN) youngsters lagged behind at simply over one in three (36%), though this may occasionally mirror that some providers obtained from Indian Well being Service suppliers not being captured within the evaluation (see Strategies). Between 2019 and 2020, the well-child go to price fell for all racial and ethnic teams. Hispanic and Asian youngsters skilled the most important share level declines in well-child charges (9 share factors for each teams), however they nonetheless had increased charges in comparison with different teams as of 2020. Black, Native Hawaiian, and Different Pacific Islander (NHOPI), and AIAN youngsters additionally skilled bigger share level declines of their well-child go to charges in contrast with White youngsters, and AIAN youngsters had the most important relative decline on account of their decrease beginning price. As of 2020, charges remained lowest for NHOPI (42%) and AIAN youngsters (29%). Twenty-two states, together with some states which are dwelling to bigger shares of AIAN and NHOPI youngsters, have been excluded from the race/ethnicity evaluation attributable to information high quality points (see Strategies).
Youngsters ages three and older have decrease charges of well-child visits and skilled bigger declines in well-child visits in the course of the pandemic than youngsters beneath age three (Determine 2). Effectively-child go to charges are highest when youngsters are younger as a result of a number of well-child visits are beneficial for youngsters beneath age three. Though youngsters beneath three have highest charges of a single well-child go to inside the 12 months, it’s unknown whether or not the charges of adherence to beneficial well-child screenings are increased or decrease than that of different teams as a result of this evaluation solely accounts for one well-child go to in a 12 months. Effectively-child go to charges steadily lower as youngsters grow old apart from the 10-14 age group, the place considerably increased charges could mirror college vaccination necessities.
Effectively-child go to charges are decrease in rural areas than city ones, however city areas had bigger declines in the course of the first 12 months of the pandemic (Determine 2). The share of Medicaid/CHIP youngsters dwelling in rural areas with a well-child go to declined from 47% in 2019 to 43% in 2020 whereas the share for city areas fell from 56% in 2019 to 49% in 2020, narrowing the hole between Medicaid/CHIP well-child go to charges in rural and concrete areas. Be aware that 18% of youngsters within the evaluation lived in a rural space, and three states have been excluded from the geographic space evaluation attributable to information high quality points (see Strategies). This evaluation additionally examined modifications for youngsters by eligibility group, managed care standing, intercourse, and presence of a continual situation; information should not proven however well-child go to charges for Medicaid/CHIP youngsters declined throughout all teams from 2019 to 2020.
| There may be substantial variation in youngsters’s well-child go to charges throughout information sources (Appendix Desk 1). Charges range relying on whether or not the information are self-reported survey information or medical claims information. KFF evaluation of 2020 nationwide survey information and Medicaid claims information (used on this evaluation) finds that the share of Medicaid/CHIP youngsters with a well-child go to inside the 12 months can range from 48% in Medicaid claims information to 93% within the Nationwide Well being Interview Survey (NHIS).
Research have discovered that utilization charges can range considerably between self-reported survey information and claims information, seemingly due partially to recall bias in surveys and the sorts of claims being included. Analysis has proven that the accuracy of self-reported utilization in survey information decline over lengthy recall durations and/or for extra routine providers. Claims information solely seize well-child visits that have been billed to the payer, on this case Medicaid, and a few settings similar to group clinics, colleges, or Indian Well being Service amenities could not all the time invoice Medicaid. There can be variation in utilization charges throughout survey sources due partially to completely different survey query designs. Nationwide surveys similar to NHIS and the Nationwide Survey of Youngsters’s Well being (NSCH) each acquire data on youngsters’s well-child visits, although there are variations within the questions requested. NHIS asks a collection of questions on how lengthy it has been since a baby has seen a “physician or different well being skilled for a properly little one go to, bodily, or common objective checkup” whereas NSCH asks about “what number of occasions (up to now 12 months) did this little one go to a health care provider, nurse, or different well being care skilled to obtain a preventive check-up?”. Developments in well-child go to charges by race and ethnicity or protection sort range throughout information sources. This evaluation exhibits Hispanic and Asian youngsters enrolled in Medicaid/CHIP have the very best well-child go to charges. Nevertheless, NHIS exhibits that well-child go to charges in Medicaid/CHIP have been comparable throughout racial and ethnic teams in 2020 (Appendix Desk 1). NSCH exhibits that White and AIAN youngsters enrolled in Medicaid/CHIP had the very best charges throughout all racial and ethnic teams in 2020. Additional, completely different information sources present various tendencies by medical insurance protection sort. Information from NHIS in 2020 present comparable charges for Medicaid/CHIP in comparison with personal insurance coverage whereas information from the NSCH exhibits charges are increased for youngsters with personal insurance coverage in contrast with Medicaid/CHIP. Healthcare Effectiveness Information and Info Set (HEDIS) measures for little one and adolescent well-care visits additionally present increased charges in industrial HMO and PPO plans in contrast with Medicaid HMO plans. This evaluation makes use of claims information (T-MSIS), not self-reported survey information, to look at tendencies in well-child visits due to the usage of T-MSIS in EPSDT and Baby Core Set reporting. States can now choose to have CMS generate their EPSDT CMS-416 studies utilizing T-MSIS; 28 states opted for this in 2021. CMS can also be investigating the usage of T-MSIS for Baby Core Set reporting, which is now necessary, in try and alleviate the reporting burden for states. These studies are meant to observe the supply of the EPSDT profit and determine gaps in addition to measure well being care outcomes and are more and more utilizing T-MSIS to take action. |
What to look at?
Effectively-child go to charges for Medicaid/CHIP youngsters total fall beneath the aim price, with bigger gaps for AIAN, Black and NHOPI youngsters in addition to older youngsters and youngsters dwelling in rural areas, highlighting the significance of outreach and different focused initiatives to handle disparities. Addressing entry limitations and creating group partnerships have been proven to extend well-child go to charges and scale back disparities. It will likely be vital to trace, as information turn out to be out there, the extent to which well-child go to charges in addition to vaccination charges (typically administered at well-child visits) rebounded in the course of the pandemic restoration and the place gaps stay.
Latest state and federal actions might assist promote entry, high quality and protection for youngsters that might improve well-child go to charges. The Bipartisan Safer Communities Act included quite a few Medicaid/CHIP provisions to make sure entry to complete well being providers and strengthen state implementation of the EPSDT profit. CMS additionally launched an up to date school-based providers claiming information, and states have taken motion to broaden Medicaid protection of school-based care lately. In 2024, it turned necessary for states to report the Baby Core Set, a set of bodily and psychological well being high quality measures, with the aim of enhancing well being outcomes for youngsters. As well as, as of January 2024, all states are actually required to offer 12-month steady eligibility for Medicaid and CHIP youngsters, which might assist stabilize protection and assist youngsters stay related to care. Three states additionally lately obtained approval to increase steady eligibility for youngsters in Medicaid for a number of years, which might assist youngsters keep protection past one 12 months. Within the lately launched FY 2025 price range, the Biden Administration proposes establishing the choice for states to offer steady eligibility in Medicaid and CHIP for youngsters from delivery to age six or for 36 month durations for youngsters beneath 19.
Lastly, hundreds of thousands of youngsters are shedding Medicaid protection in the course of the unwinding of the continual enrollment provision, which might have implications for entry. Information as much as March 2024 present that youngsters’s web Medicaid enrollment has declined by over 4 million. In some circumstances, youngsters dropped from Medicaid could have transitioned to different protection, however they could additionally turn out to be uninsured, regardless of in lots of circumstances remaining eligible for Medicaid or CHIP. Whereas individuals of coloration usually tend to be lined by Medicaid, information on disenrollment patterns by race and ethnicity are restricted. KFF evaluation exhibits people with out insurance coverage protection have decrease entry to care and usually tend to delay or forgo care attributable to prices. A lack of protection or gaps in protection will be particularly problematic for younger youngsters who’re beneficial to obtain frequent screenings and check-ups.
| Information: This evaluation used the 2019-2020 T-MSIS Analysis Identifiable Information together with the inpatient (IP), long-term care (LT), different providers (OT), and pharmacy (RX) claims recordsdata merged with the demographic-eligibility (DE) recordsdata from the Continual Situation Warehouse (CCW).
Figuring out Effectively-Baby Visits: This evaluation used the process and prognosis codes listed within the Annual Early and Periodic Screening, Diagnostic, and Therapy (EPSDT) Participation Report (CMS-416) reporting directions (see line 6) to determine when a well-child go to occurred. This technique of figuring out well-child visits mirrors the current CMS well-child go to evaluation. Figuring out Utilization of Any Medicaid Companies: To find out if a baby within the evaluation utilized any Medicaid providers inside the 12 months, all fee-for-service or managed care encounter claims throughout the IP, LT, OT, and RX claims recordsdata have been flagged (claims for capitated funds or any funds not billed on the enrollee degree have been excluded). If a baby had any flagged claims, the kid was recognized as using a service inside the 12 months. Defining Rural and City Areas: This evaluation makes use of enrollee zip code data and the US Division of Agriculture (USDA) Rural-City Commuting Areas (RUCA) codes (based mostly on 2010 census information) to designate rural and concrete areas. Zip codes with a RUCA worth larger than or equal to 4 are designated as rural. Enrollee Inclusion Standards: This evaluation contains youngsters ages 0 to 21 who have been enrolled in Medicaid or CHIP with full advantages for 12 months. The 12-month enrollment interval is according to the current CMS evaluation, however that evaluation solely included youngsters beneath the age of 19. State Inclusion Standards: To evaluate the usability of states’ information, the evaluation examined high quality assessments from the DQ Atlas for restricted advantages code, claims quantity, and managed care encounters and in contrast the share of youngsters with a well-child go to in T-MSIS to the share of youngsters receiving no less than one preliminary or periodic screening within the annual EPSDT reporting information recordsdata. The evaluation excluded any states that, for a specific 12 months, had each a “Excessive Concern/Unusable” DQ Atlas evaluation and a greater than 10-percentage level distinction between the share of youngsters with a well-child go to in T-MSIS and the share reported within the state’s annual EPSDT report. One state (WV) was excluded based mostly on these standards, leaving 50 states (together with DC) in the principle evaluation. For reporting by race/ethnicity, we excluded states with “Excessive Concern/Unusable” DQ Atlas assessments in 2019 or 2020. Amongst states in the principle evaluation, 21 states have been excluded (AL, AZ, AK, CO, CT, DC, HI, IA, KS, LA, MD, MA, MO, MT, NY, OR, RI, SC, TN, UT, and WY). This left 29 states for reporting by race/ethnicity (Determine 2). For reporting by geographic space, we excluded states with “Excessive Concern/Unusable” DQ Atlas assessments for zip code in 2019 or 2020. Amongst states in the principle evaluation, two states have been excluded (RI and VT). This left 48 states (together with DC) for reporting by geographic area. Limitations:
|