Introduction
Steerage from the Division of Well being and Human providers identifies people with restricted English proficiency (LEP) as those that don’t converse English as their major language and who’ve a restricted capability to learn, write, converse, or perceive English. People with LEP disproportionately expertise gaps in medical insurance protection and poor well being outcomes, associated to difficulties in comprehending and speaking well being care data. People with LEP make up a disproportionate share of the Medicaid inhabitants and are extra doubtless than English proficient enrollees to expertise administrative limitations to finishing Medicaid renewal processes, which can lead to them dropping protection regardless of remaining eligible. As a result of individuals of colour are considerably extra prone to have LEP than White individuals, these limitations can even exacerbate racial and ethnic well being disparities.
Provisions within the Households First Coronavirus Response Act (FFCRA) require states to take care of steady Medicaid enrollment for enrollees till the top of the month when the COVID-19 public well being emergency (PHE) ends. The present PHE was prolonged in January 2022. The Biden Administration has stated that it’ll give states a 60 day discover earlier than the PHE expires. Since that discover was not issued in February, it’s anticipated that the PHE will likely be prolonged once more by means of mid-July which might imply that the continual enrollment provisions might expire firstly of August 2022 (if laws doesn’t go to set an earlier finish date), except the PHE is prolonged once more.
When the continual enrollment necessities finish and states resume redeterminations and disenrollments, people with LEP could also be at elevated danger of dropping Medicaid protection or experiencing a niche in protection on account of limitations finishing these processes, even when they continue to be eligible for protection. Along with the continual enrollment provisions, many states have leveraged Medicaid emergency authorities to broaden eligibility or streamline enrollment processes in the course of the pandemic. Nonetheless, it stays to be seen whether or not states will keep these processes after the general public well being emergency ends.
This transient examines points to think about for sustaining protection for eligible individuals with LEP when the PHE ends, together with:
- Who’re Medicaid enrollees with LEP?
- What limitations would possibly individuals with LEP face to sustaining protection when the PHE ends?
- How can states mitigate protection gaps and losses for eligible individuals with LEP?
Who’re Medicaid enrollees with LEP?
Medicaid households embody a disproportionate share of nonelderly adults with LEP. General, 16% of nonelderly adults residing in households with a minimum of one Medicaid enrollee have LEP, that means they reported talking English lower than very properly, in comparison with 7% of nonelderly adults in households by which no member is enrolled in Medicaid (Determine 1). Furthermore, practically 1 / 4 (23%) of kids enrolled in Medicaid have a dad or mum that speaks English lower than very properly.
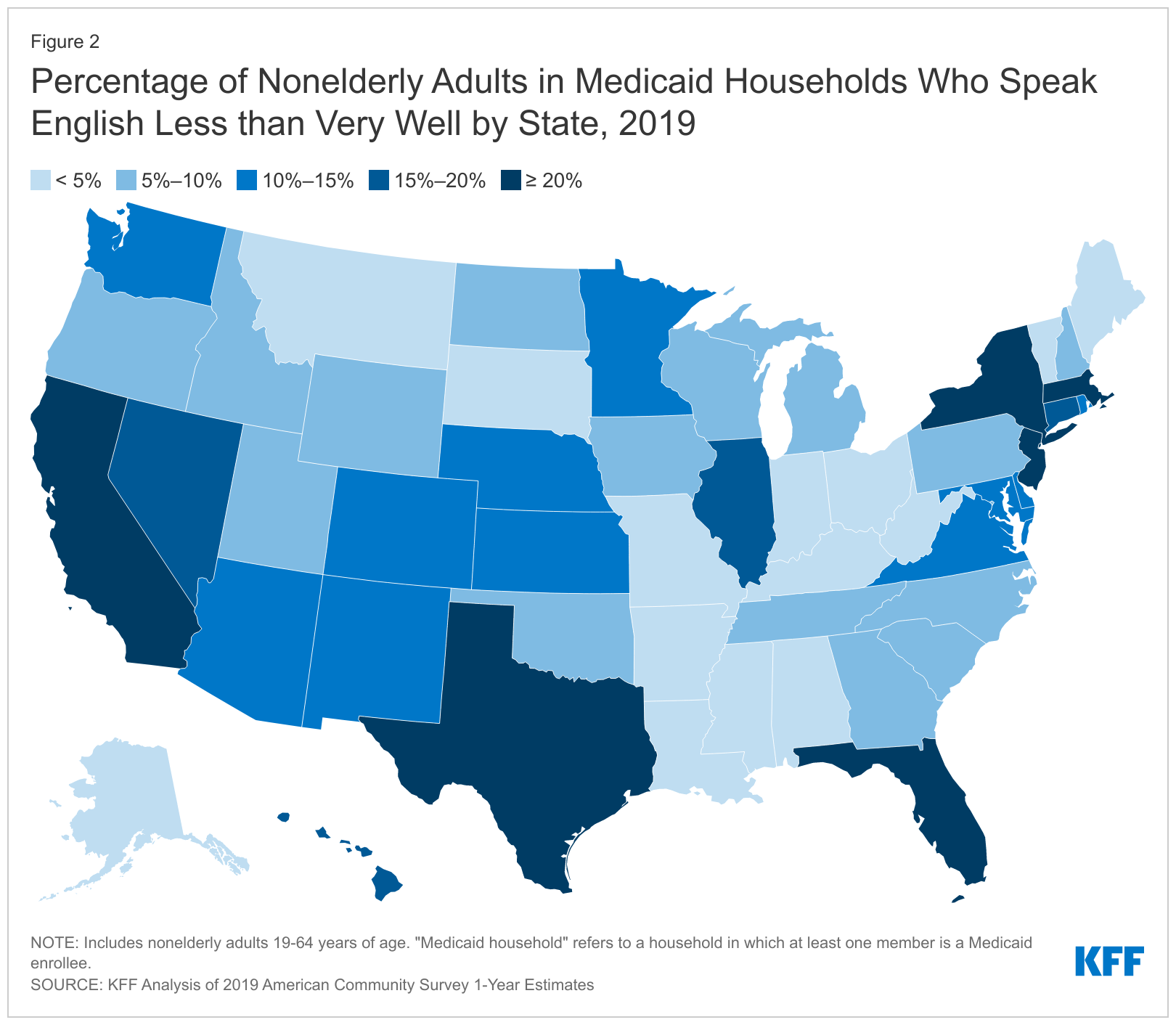
The share of nonelderly adults in a family with Medicaid who converse English lower than very properly is larger in some states. For instance, the share of nonelderly adults in Medicaid households with LEP ranges from a low of lower than 1% in West Virginia to a excessive of 29% in California (Determine 2). Different states with comparatively excessive shares of nonelderly adults in Medicaid households with LEP embody New Jersey (25%), New York (24%), Texas (25%), Massachusetts (21%) and Florida (21%).
Most nonelderly adults in Medicaid households who’ve LEP are Hispanic and converse Spanish as their major language (Determine 3). Nonetheless, 16% are Asian, 7% are White and 4% are Black. Whereas Spanish is the commonest language spoken amongst nonelderly adults in Medicaid households who’ve LEP, Chinese language and Vietnamese are every spoken by 3% of those adults, and there are a various set of languages spoken general by this group. The opposite high ten languages spoken amongst these adults, embody Arabic, Haitian, Tagalog, Korean, Portuguese, Russian and French. Furthermore, the focus of major languages amongst this group will fluctuate throughout areas.
What limitations would possibly enrollees with LEP face to sustaining Medicaid protection when the PHE ends?
All Medicaid enrollees might face administrative limitations to finishing renewal and eligibility redetermination processes, however enrollees with LEP face elevated danger of encountering difficulties on account of language limitations. Complicated enrollment and renewal processes have traditionally been limitations to acquiring and sustaining Medicaid protection. Beneath present guidelines, states should first search to resume eligibility mechanically or on an ex parte foundation, by checking all accessible knowledge sources to substantiate if eligibility will be renewed with out contacting or requesting data from the household. Nonetheless, on account of variations in IT capabilities, states fluctuate broadly in what number of renewals they’re processing mechanically. When a state is unable to substantiate eligibility by means of accessible knowledge sources, it should ship requests for data and, in some instances, documentation to enrollees. All Medicaid enrollees might face potential challenges associated to understanding redetermination processes, offering data and documentation when requested, and assembly required timeframes that may end up in protection losses amongst individuals who stay eligible. Enrollees with LEP are at specific danger for experiencing difficulties, as they might face added challenges understanding and finishing duties or types on account of language limitations, significantly if they don’t seem to be offered supplies translated into their language. For instance, one research of Medicaid enrollees with LEP in Illinois discovered LEP respondents have been over 5 instances as prone to lose their Medicaid advantages in comparison with English proficient respondents at redetermination. Nearly all of LEP respondents reported having issue comprehending Medicaid renewal documentation and felt that finishing the advantages renewal type was tough or very tough. Practically half of LEP respondents additionally reported restricted consciousness of the redetermination course of.
How can states mitigate Medicaid protection gaps and losses for eligible individuals with LEP?
States can take a variety of actions to mitigate protection gaps and losses for eligible individuals once they resume eligibility determinations and renewals on the finish of the PHE. The Facilities for Medicare and Medicaid Providers (CMS) outlined a variety of coverage and operational methods for states to think about to take care of steady protection for eligible people when regular eligibility willpower operations resume and particular methods for Medicaid enrollees with LEP, together with:
Streamlining renewal processes to attenuate actions required by enrollees. As a result of enrollees with LEP might face elevated issue understanding and finishing types or directions, minimizing the actions individuals must take to take care of protection could also be significantly useful. States can reduce required actions by rising the shares of Medicaid/CHIP renewals performed mechanically and simplifying processes for different renewals. CMS has recognized steps states can take to extend the shares of renewals accomplished mechanically, together with increasing the kinds of knowledge sources used for renewal and creating an information supply hierarchy to prioritize the latest and dependable knowledge sources. For these renewals that can not be accomplished mechanically, CMS notes that states can assist continuity of protection by offering a number of modes for individuals to submit data (e.g., telephone, mail, on-line, and in-person) and prepopulating types, as required below federal guidelines, and by taking over different choices, comparable to extending deadlines for response.
Facilitating entry to clear and linguistically accessible communications, together with notices and requests for extra data in addition to throughs web site and name facilities. Beneath Title VI of the Civil Rights Act and Part 1557 of the Inexpensive Care Act, state Medicaid companies are required to offer significant entry to individuals with LEP. Steerage from the Division of Well being and Human Providers clarifies that state Medicaid companies should take cheap steps to make sure significant entry to their applications by individuals with LEP by balancing 4 components, together with “1) The quantity or proportion of LEP individuals eligible to be served or prone to be encountered by this system or grantee; (2) the frequency with which LEP people are available contact with this system; (3) the character and significance of this system, exercise, or service offered by this system to individuals’s lives; and (4) the assets accessible to the grantee/recipient and prices.”
Sharing and implementing greatest practices utilized by states in assembly language entry necessities. Earlier work has recognized promising practices amongst states to facilitate entry for individuals with LEP, together with designating employees to coordinate language providers actions; involving the group to help with planning and implementing providers; creating written language entry plans that establish language wants and description methods to fulfill these wants; introducing availability of language providers at people’ first level of contact by means of posters or indicators; using bilingual employees and properly as contracting out for interpreters and translators, together with phone language traces; and translating paperwork or offering taglines on paperwork to tell people about interpreter availability when assets will not be accessible for full translation. For instance, Colorado requires all Medicaid shopper correspondence to be precisely translated into the second mostly spoken language within the state and embody a tagline, translated into the highest 15 languages spoken in Colorado by people with LEP, informing enrollees find out how to search additional help in understanding the content material of correspondence. Past these methods to facilitate communication with enrollees, states can even design insurance policies to attenuate protection gaps for individuals with LEP. For instance, Tennessee permits good trigger extensions for people who don’t full the Medicaid eligibility willpower paperwork in a well timed method in the event that they require and will not be offered help with English translation.
Adopting CMS advised methods for speaking successfully with individuals who have LEP to take care of protection of eligible people when the PHE ends. These methods embody:
- Overview their language entry plans to offer written translation and oral interpretation of data and recommendation to people with LEP on how they’ll entry free language providers;
- Translate notices, types, and different communications into a number of languages by certified translators and evaluate these supplies for cultural competence;
- Overview and improve entry to and availability of certified oral interpreters who converse incessantly spoken languages in individual and thru certified telephonic interpreters, and
- Replace web sites with taglines in non-English languages to advise individuals with LEP on how they’ll entry language providers freed from cost.
The Division of Justice (DOJ), additionally lately launched really helpful methods from a federal interagency working group for enhancing entry to public web sites and digital providers for individuals with LEP. These embody making very important digital data accessible to individuals with LEP by translating content material, prominently displaying multilingual content material on web sites and translating dropdown menus and search bars, guaranteeing translated content material hyperlinks to different content material that’s translated or speaking that the hyperlink results in English content material, and guaranteeing web site and digital providers inform individuals of find out how to entry language help providers.
Partaking with trusted group companions to conduct outreach and supply help. A mix of broad and focused outreach methods will likely be necessary for serving to enrollees perceive renewal necessities and keep protection. Working intently with group companions to conduct outreach and supply help will likely be significantly necessary for successfully reaching enrollees with LEP. CMS suggests states work with community-based organizations, software assisters, and suppliers to remind enrollees to offer up to date contact data and about renewal or eligibility redetermination necessities. CMS additionally advises states to conduct outreach by means of a number of modalities, together with utilizing textual content messaging to ship reminders to enrollees about requested data or required actions. In August 2021, CMS introduced $80 million in funding for 60 Navigator applications in 30 states with Federally-Facilitated Marketplaces for the 2022 plan yr, considerably larger than the annual funding awarded in 2018-2020. Navigator applications should present data that’s culturally and linguistically acceptable. Navigators can help people with renewing Medicaid protection and assist those that are not eligible for Medicaid transition to protection by means of the marketplaces, which can be significantly necessary for individuals with LEP.