For privately insured sufferers, shock medical payments can come up from both having to pay a excessive deductible, or from “stability billing.” Usually, well being plans negotiate funds to in-network suppliers. Out-of-network suppliers might instantly invoice privately insured sufferers the distinction between the standard in-network well being plan cost and the total cost, often known as “stability payments”. In these circumstances, sufferers could be accountable for the stability invoice along with any deductible, coinsurance, or copay underneath the well being plan.
The No Surprises Act prohibits many of those stability payments beginning in 2022. Privately insured sufferers (together with these with employer-based protection, non-group plans, and grandfathered plans) are protected against sure shock stability payments. The shock stability billing protections require non-public well being plans to cowl out-of-network claims and apply in-network value sharing (deductibles, copayments) for sure lined advantages. The regulation prohibits sure suppliers, hospitals, and air ambulance from shock stability billing sufferers for out-of-network care, except the affected person consents forward of time.
The brand new protections require plans and suppliers to take the sufferers out of most of the most typical cost disputes. Although it’s potential that sufferers nonetheless get stability payments, together with due to plan or supplier billing errors, the invoice shouldn’t be lined underneath the brand new regulation (for instance, floor ambulance rides, non-covered companies, affected person consents to out-of-network care prices), or the well being plan denies the declare utterly as not lined by the plan.
The affected person may get balanced payments, as an example, if the affected person’s plan incorrectly processes a declare or applies out-of-network cost-sharing quantity when the NSA prohibits it. A affected person may get billed greater than they must be, for instance, if the plan doesn’t acknowledge {that a} declare is topic to the No Surprises Act, or due to a billing oversight. Sufferers can attraction these errors utilizing the plan’s inside claims and appeals process. Underneath the federal regulation, the affected person has the fitting to attraction a well being plan denial (referred to as an opposed profit willpower or “ABD”). ABDs additionally embody plan selections to use the inaccurate cost-sharing quantity. As soon as the opposed profit willpower has been made, the well being plan should give the affected person at the very least 180 days to file an inside attraction. For post-service claims, the plan should then full the interior attraction no later than 60 days after it’s filed. If the plan upholds its denial, the affected person has a brand new proper underneath the NSA to ask for an unbiased exterior attraction for NSA compliance points. Federal rules present a number of examples for when NSA-related selections could be reviewed by an exterior reviewer, together with a choice about whether or not a particular declare entails an merchandise or service that’s lined by the NSA as a shock invoice.
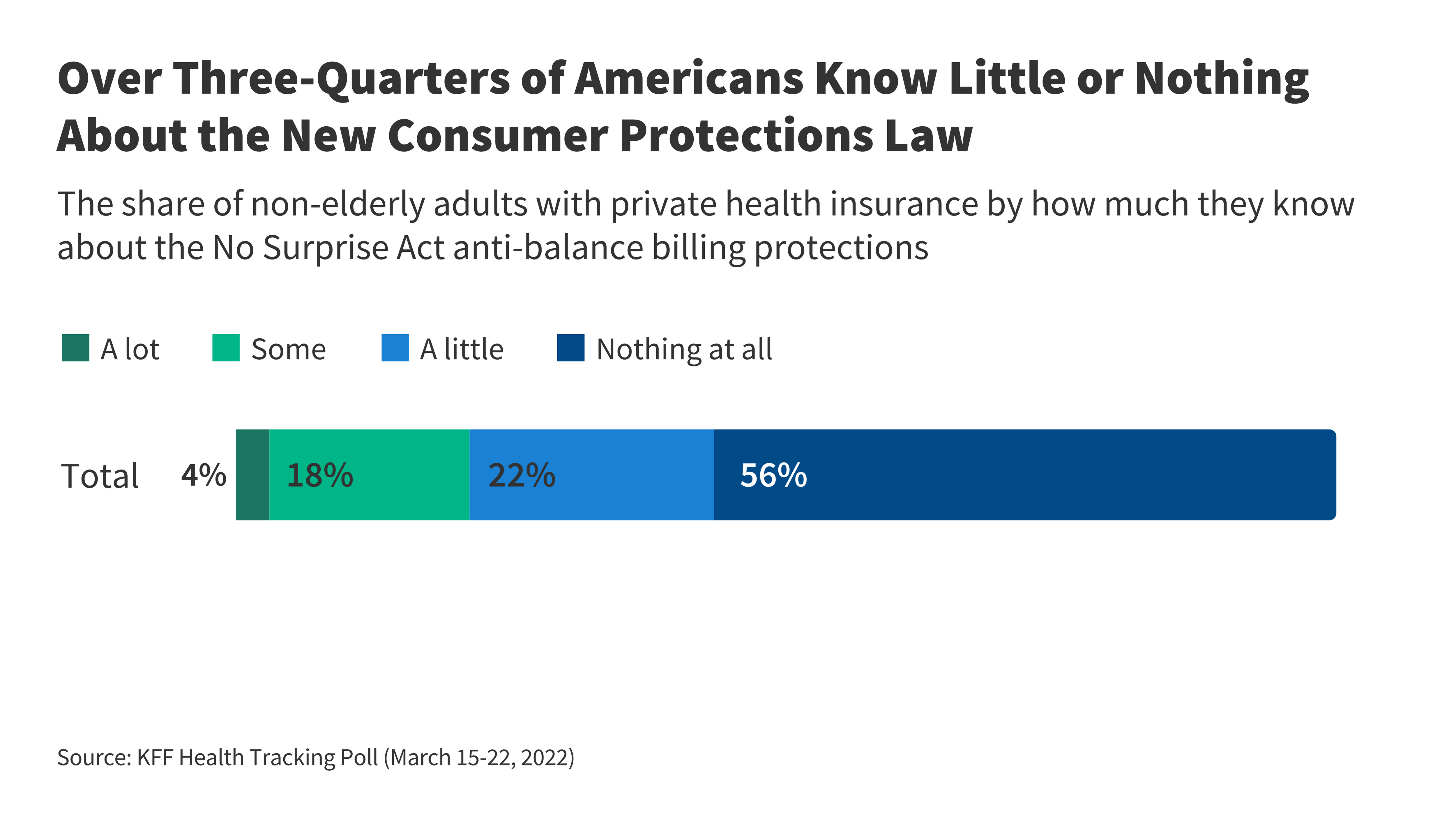
For sufferers who obtain a shock invoice when they need to not, what follows could also be extra difficult. To right the scenario, sufferers would first want to acknowledge that the plan’s determination was incorrect and that the supplier invoice is topic to the No Surprises Act. KFF polling finds the overwhelming majority of Individuals (78%) know little or nothing concerning the new client protections regulation, so the effectiveness of self-advocacy by shoppers might be restricted if issues come up. Underneath present regulation, any well being plan ABDs should embody contact info for state client help packages (CAPs) and spot that such packages (in states the place they exist) may help folks file an attraction. Shoppers may attain out to CAPs to get an evaluation of whether or not the invoice they obtained is legitimate. Moreover, as a part of the No Surprises Act, the Facilities for Medicare and Medicaid Companies (CMS) has established sources for sufferers to hunt evaluation of their medical payments (via this web site: https://www.cms.gov/medical-bill-rights/assist/submit-a-complaint or by calling the No Surprises Assist Desk at 1-800-985-3059 which is accessible 24/7 and thru holidays). This no-wrong-door complaints system is accessible for shoppers who’re involved their plan might have incorrectly denied or lined a shock medical invoice.
In the meantime, nevertheless, if a plan incorrectly denies or covers a shock invoice and the affected person doesn’t acknowledge the error so as to have the ability to both attraction or ask for a state or federal evaluation, the affected person may get caught with the invoice.
Whereas sufferers attraction, there isn’t any federal rule stopping suppliers from making an attempt to gather the excellent invoice. For incorrect payments, if the affected person appeals, the out-of-network supplier may be capable to invoice the affected person for the total cost whereas the attraction is underway. Sufferers who’re unable to pay the excellent invoice could also be referred to assortment businesses. Although the Shopper Finance Safety Bureau (CFPB) has outlined extra tips proscribing coercive practices from assortment businesses. KFF polling has discovered that 41% of adults have well being care debt in response to a broader definition, which incorporates well being care debt on bank cards or owed to relations. KFF evaluation of a census survey suggests Individuals might owe at the very least $220 Billion in medical debt. Folks with medical debt report slicing spending on meals, clothes, and different home items, spending down their financial savings to pay for medical payments, borrowing cash from mates or relations, or taking over extra money owed. Medical debt might make it tough for sufferers to get loans for every day dwelling like housing or automotive.
Later, if the affected person prevails on the attraction, the well being plan would wish to reprocess the declare, this time following the No Surprises Act guidelines, and the out-of-network supplier would then be required to refund the affected person for any quantity collected in extra of the relevant in-network value sharing quantity.
Underneath the Inexpensive Care Act and the No Surprises Act, federal businesses can impose penalties on well being plans and suppliers for incorrectly billing sufferers. For plans who incorrectly course of claims, they are often charged as much as $100 per day per affected beneficiary underneath federal regulation. State regulators might have extra authority and enforcement instruments they will use to handle billing issues. On the supplier aspect, the penalty for incorrect billing is as much as $10,000 per violation. That’s, if a supplier sends 200 incorrect payments, the supplier might be penalized $2 million. However for these penalties to occur, the affected person must efficiently lodge a grievance with federal regulators and the regulators would wish to analyze and implement.
Via October 2023, about 11,000 affected person complaints have been filed via the federal suggestions portal. The federal authorities has stated 248 complaints concerned a violation and resulted in $3 million in financial reduction paid to shoppers or suppliers. At this level, it’s unclear whether or not the federal authorities has issued penalties to suppliers or well being plans for incorrect billing practices.
Dialogue
Most sufferers have no idea concerning the new shock billing protections and certain additionally have no idea of sources accessible to hunt recourse for incorrect medical payments. It’s advisable to ask about the fee forward of time, when potential. Moreover, when sufferers get a big, sudden invoice, a very good first step is to name the well being plan. New federal sources enable sufferers to submit complaints and get a response from the federal authorities. The federal course of doesn’t present a willpower or assist the buyer battle a invoice with the payer. Sufferers might have little recourse, nevertheless, if their plan doesn’t cowl sure gadgets or companies, or if their shock stability invoice shouldn’t be protected underneath federal regulation.
Plans and suppliers can now arbitrate disagreements over funds for out-of-network care by way of the No Surprises Act unbiased dispute decision. Most cost determinations via the arbitration course of have been in favor of the suppliers’ asking worth. But many of the lawsuits in opposition to the No Surprises Act are additionally being introduced by suppliers. The federal authorities lately proposed a number of adjustments with the purpose of creating the IDR course of extra environment friendly and rising early communication between the events. Within the midst of the authorized disputes over the dispute decision course of for cost charges, sufferers are required to be held innocent for shock, out-of-network stability payments.
Sufferers usually are not alleged to get shock stability payments, except there’s a mistake or the shock invoice shouldn’t be protected. In these conditions, sufferers have some recourses, although they’re solely useful if folks learn about them.